CV Control Centers - The Body's Governors
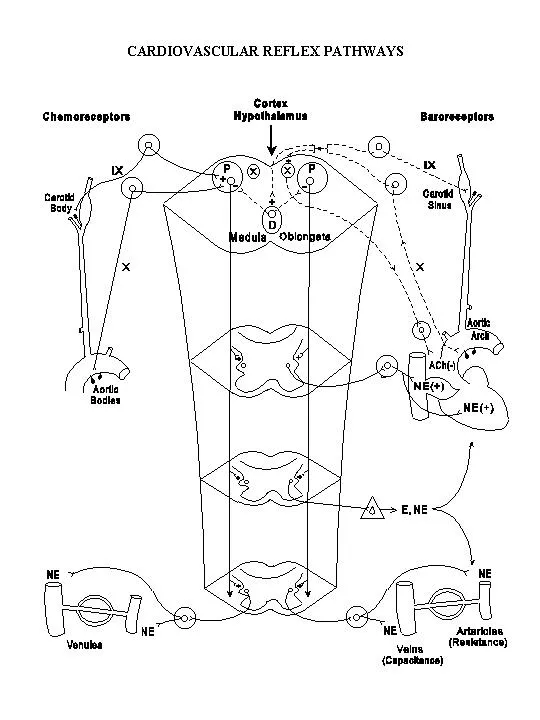
- Primary Sensors & Pathways:
- Baroreceptors (Pressure): Detect stretch. Carotid sinus (via CN IX) & aortic arch (via CN X).
- Chemoreceptors (Chemicals):
- Peripheral (carotid/aortic bodies): Sense ↓ $PO_2$, ↑ $PCO_2$, ↓ pH.
- Central (medulla): Sense CSF pH & $PCO_2$.
- Central Integration: All afferents converge on the Nucleus Solitarius in the medulla.
- Efferent Response: Modulates sympathetic & parasympathetic outflow to control heart rate, contractility, & vascular tone.
⭐ Exam Favorite: Carotid sinus massage artificially stretches the baroreceptors, fooling the body into thinking blood pressure is high. This triggers a reflex increase in vagal tone, slowing AV conduction and heart rate, which can terminate certain supraventricular tachycardias.
Response to Exercise - The Body at Work
- Initiation: Central command (higher brain centers) anticipates exercise, activating the sympathetic nervous system.
- Cardiovascular Effects:
- ↑ Cardiac Output (CO): Driven by an increase in both heart rate (HR) and stroke volume (SV). $CO = HR \times SV$.
- ↑ Heart Rate: Due to ↑ sympathetic and ↓ parasympathetic tone.
- ↑ Stroke Volume: Due to ↑ contractility and ↑ preload (venous return).
- ↑ Pulse Pressure: Systolic BP rises while diastolic BP remains stable or slightly decreases.
- Blood Flow Redistribution:
- Vasodilation in active skeletal muscle via local metabolites (e.g., adenosine, K+, CO₂).
- Vasoconstriction in splanchnic, renal, and cutaneous circulations.
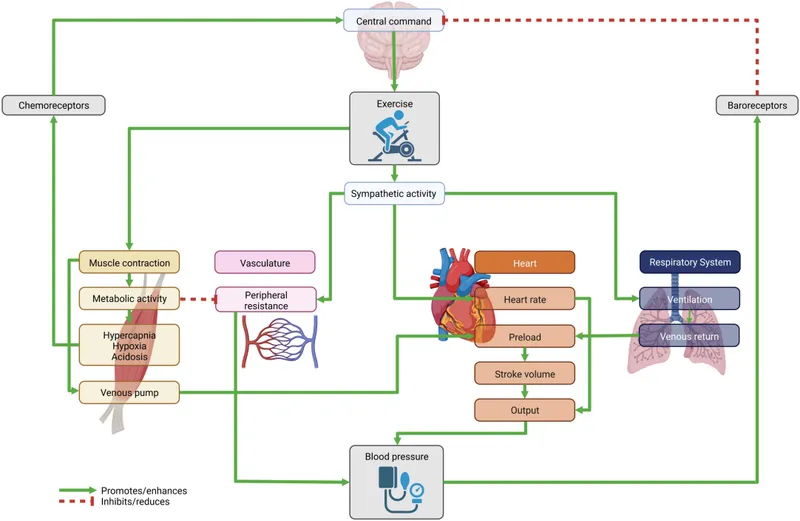
⭐ During dynamic exercise (e.g., running), Total Peripheral Resistance (TPR) decreases. This is due to massive vasodilation in exercising skeletal muscles, which outweighs vasoconstriction in other areas like the gut.
Response to Hemorrhage - The Body Under Siege
Initial insult is hypovolemia (↓ blood volume), leading to ↓ venous return, ↓ cardiac output (CO), and ↓ mean arterial pressure (MAP).
- Immediate Compensation (Seconds to Minutes):
- Baroreflex: ↓ MAP unloads baroreceptors → ↑ Sympathetic outflow & ↓ Parasympathetic outflow.
- Results: ↑ Heart rate (tachycardia), ↑ contractility, and intense arteriolar vasoconstriction (cool, clammy skin).
- Hormonal Response (Hours to Days):
- RAAS Activation: ↓ Renal perfusion triggers renin release → Angiotensin II → Vasoconstriction & Aldosterone release (Na⁺/water retention).
- ADH Release: ↑ Plasma osmolality & ↓ atrial stretch → ADH secretion → Water reabsorption in kidneys.
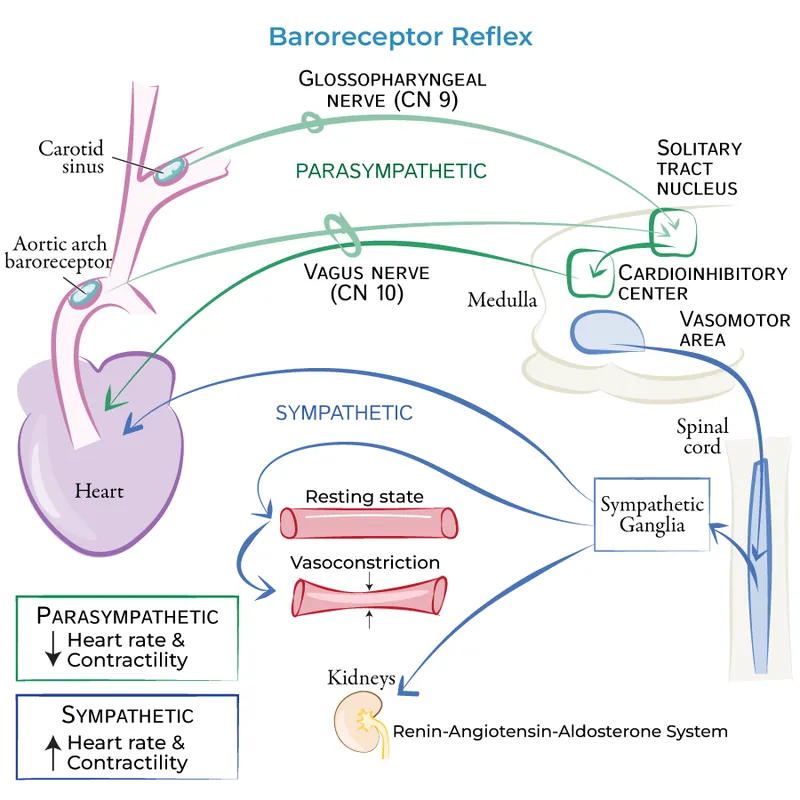
⭐ The body fiercely defends cerebral and coronary perfusion. In response to hemorrhage, blood is shunted away from the skin, kidneys, and splanchnic circulation to preserve flow to the brain and heart.
📌 For hemorrhagic shock classes (I-IV), recall that Class III is where the blood pressure finally drops significantly.
Postural Changes - The Sudden Stand
Upon standing, gravity causes venous pooling (~500-700 mL) in the lower extremities. This leads to a transient decrease in venous return, which in turn reduces cardiac output and arterial blood pressure.
- Baroreflex Response: A healthy baroreflex rapidly compensates by increasing sympathetic outflow, leading to ↑ heart rate and vasoconstriction to restore BP.
- Orthostatic Hypotension: Occurs when this reflex is delayed or insufficient.
- Definition: Sustained BP drop within 3 minutes of standing:
- Systolic: ↓ by ≥20 mmHg
- Diastolic: ↓ by ≥10 mmHg
- Symptoms: Dizziness, syncope from transient cerebral hypoperfusion.
- Definition: Sustained BP drop within 3 minutes of standing:
⭐ The immediate, transient drop in blood pressure upon standing is normal; it is the failure of the baroreflex to rapidly compensate that defines orthostatic hypotension.
High-Yield Points - ⚡ Biggest Takeaways
- Exercise response: Central command and local metabolites drive ↑CO and muscle vasodilation.
- Hemorrhage: Triggers the baroreceptor reflex and RAAS, causing vasoconstriction and tachycardia to preserve BP.
- Valsalva maneuver: Demonstrates autonomic control, with a characteristic reflex bradycardia upon release (Phase IV).
- Orthostasis (standing): Transient ↓BP is rapidly corrected by the baroreceptor reflex.
- Carotid massage: Stimulates baroreceptors, causing a reflex ↓HR via increased vagal output.
- Cushing reflex: Triad of hypertension, bradycardia, and irregular respiration from ↑intracranial pressure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

