Coronary Flow Basics - The Heart's Own Supply
- Origin: Right & Left coronary arteries (RCA, LCA) arise from the aortic root.
- Supply Dominance:
- RCA: Supplies RA, RV, SA/AV nodes, posterior 1/3 of septum.
- LCA: Divides into LAD and LCX. Supplies LA, LV, anterior 2/3 of septum.
- Flow Timing: Unlike other circulations, coronary flow is maximal during diastole.
- During systole, intramyocardial pressure compresses the vessels, impeding flow, especially in the subendocardium.
- Coronary Perfusion Pressure (CPP): $CPP = P_{aortic, diastolic} - LVEDP$.
⭐ Subendocardial Ischemia: The subendocardium is most vulnerable to ischemia due to maximal systolic compression and distance from epicardial vessels.

Metabolic Regulation - The Oxygen Sensor
Coronary blood flow is tightly coupled to myocardial oxygen ($O_2$) demand. The heart has a very high $O_2$ extraction rate (~75%), so any increased demand must be met primarily by increased flow, not by further extraction.
- Primary Driver: Myocardial oxygen consumption is the main determinant of coronary flow.
- Mechanism: When $O_2$ demand exceeds supply, local metabolic factors trigger vasodilation.
- ↓ Tissue $p_O2$ (hypoxia) is the initiating signal.
- Key Local Vasodilators:
- Adenosine: The most critical link; produced from ATP degradation.
- Nitric Oxide (NO)
- $CO_2$, $H^+$, $K^+$
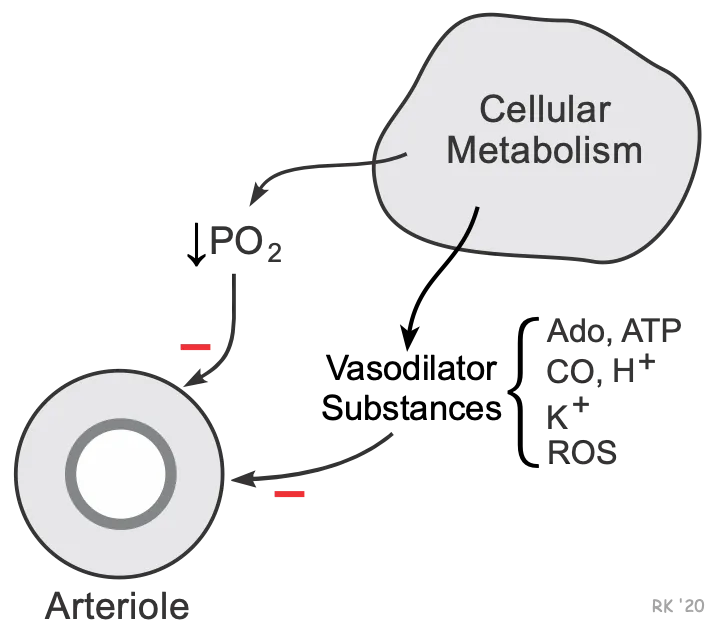
⭐ Adenosine is the primary metabolic vasodilator linking myocardial $O_2$ consumption to coronary blood flow. Its powerful vasodilatory effect is utilized in pharmacologic cardiac stress testing.
Neural & Myogenic Control - The Autonomic Grip
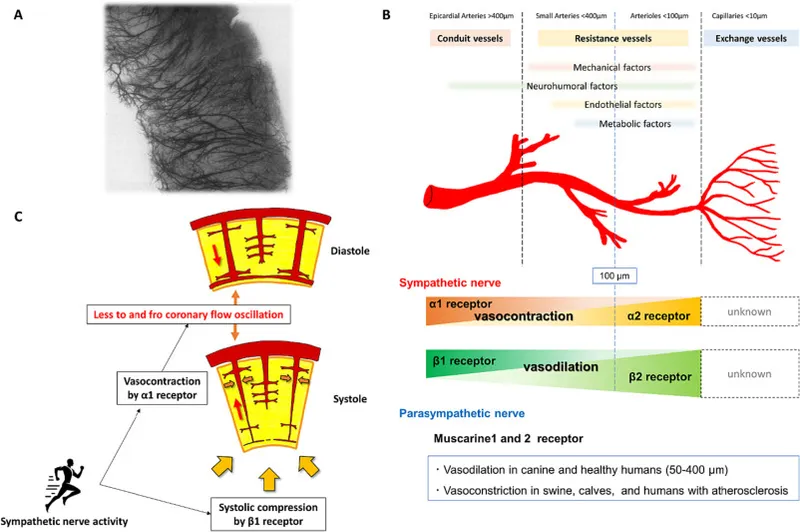
-
Sympathetic Control (Dual Effect):
- Direct Effect: α₁-receptors cause mild vasoconstriction.
- Indirect Effect (Dominant): β₁-receptors ↑ heart rate & contractility → ↑ metabolic demand (e.g., adenosine, NO) → profound vasodilation.
-
Parasympathetic (Vagal) Control: Minor role; M₃ receptors cause slight vasodilation via Nitric Oxide (NO).
-
Myogenic Control: Intrinsic response of coronary smooth muscle to stretch. ↑Pressure → vasoconstriction; ↓Pressure → vasodilation. Helps maintain constant flow.
⭐ During exercise, sympathetic stimulation causes a net increase in coronary blood flow. The powerful vasodilation from metabolic autoregulation (driven by ↑myocardial O₂ demand) overwhelmingly overrides direct α₁-mediated vasoconstriction.
Mechanical Factors - The Systolic Squeeze
- Throttling Effect: Myocardial contraction compresses coronary arteries, mechanically impeding blood flow.
- Left Ventricle (LV) Flow:
- During systole, flow is minimal as high intraventricular pressure squeezes vessels shut.
- Flow peaks in early diastole when the ventricle relaxes, allowing vessel reperfusion.
- Right Ventricle (RV) Flow: Experiences much less systolic compression due to lower RV pressures; flow is more continuous.
- Subendocardial Vulnerability: This deeper layer is most compressed and has the highest O₂ demand, making it most prone to ischemia.
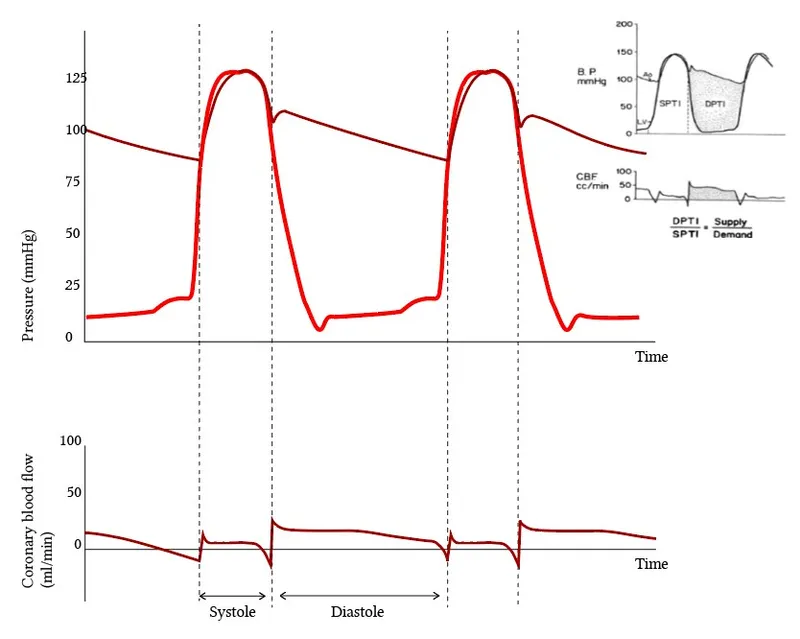
⭐ The subendocardium is the watershed zone of the heart, most vulnerable to ischemia during tachycardia (due to reduced diastolic time) and hypotension.
High‑Yield Points - ⚡ Biggest Takeaways
- Local metabolic demand is the primary driver of coronary blood flow, with adenosine being the key vasodilator.
- Most coronary perfusion, especially for the left ventricle, occurs during diastole due to systolic compression.
- The heart has a very high resting O₂ extraction (≈75%), so ↑demand must be met by ↑flow.
- Autoregulation maintains stable flow despite fluctuating aortic pressures.
- Sympathetic stimulation's metabolic override: ↑HR & contractility cause vasodilation via local metabolites, overpowering direct vasoconstriction.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

