Cardiac Output - The Heart's Work Rate
- Cardiac Output (CO): Volume of blood pumped by the ventricle per minute.
- Formula: $CO = Heart,Rate,(HR) \times Stroke,Volume,(SV)$.
- Normal CO is 4-8 L/min.
📌 Mnemonic SV CAP: Stroke Volume is determined by:
- Contractility
- Afterload
- Preload

⭐ Fick Principle: $CO = \frac{Rate,of,O_2,consumption}{Arterial,O_2,content - Venous,O_2,content}$. This principle is used to calculate CO clinically.
Stroke Volume - Preload, Afterload, Squeeze
Stroke Volume (SV) is the volume of blood pumped from the ventricle per beat. $SV = EDV - ESV$. It is determined by three primary factors:
-
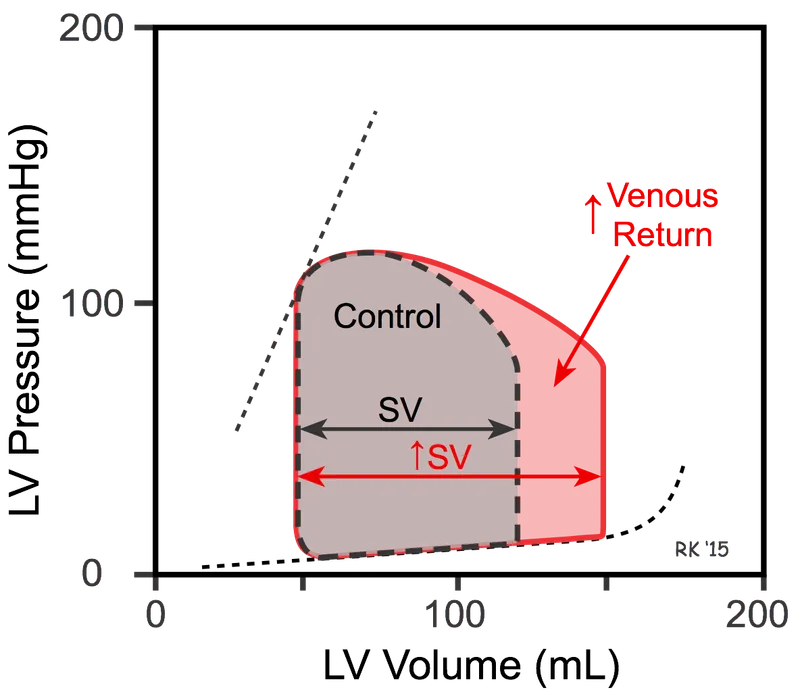
Preload: Ventricular stretch at the end of diastole, approximated by End-Diastolic Volume (EDV).
- ↑ Preload: IV fluids, exercise, ↑ venous return.
- ↓ Preload: Nitrates, diuretics, hemorrhage.
-
Afterload: Resistance the ventricle must overcome to eject blood. Approximated by Mean Arterial Pressure (MAP).
- ↑ Afterload: Aortic stenosis, systemic hypertension.
- ↓ Afterload: Vasodilators (e.g., ACE inhibitors), septic shock.
-
Contractility (Squeeze): Intrinsic myocardial contractile force, independent of preload.
- ↑ Contractility: Catecholamines (dobutamine), Digoxin, ↑Ca²⁺.
- ↓ Contractility: β-blockers, heart failure, acidosis.
⭐ Increased contractility causes a decrease in End-Systolic Volume (ESV). The heart empties more effectively, increasing the Ejection Fraction ($EF = SV/EDV$).
📌 Mnemonic: Stroke volume is determined by CAP: Contractility, Afterload, Preload.
CO Regulation - Nerves & Hormones
-
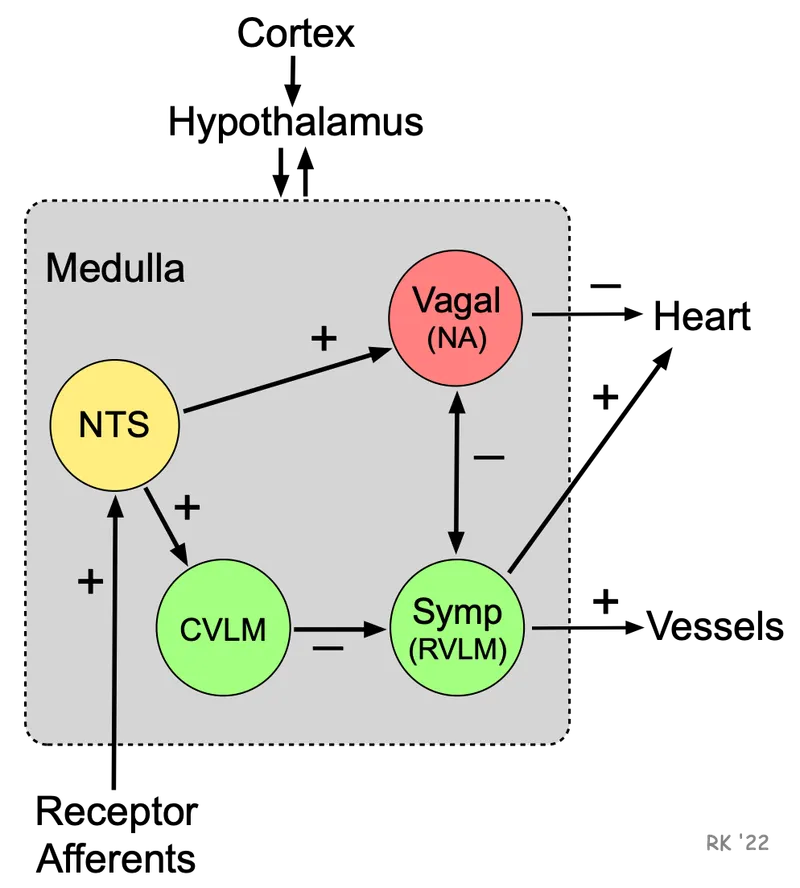
Autonomic Nervous System (ANS): The primary, rapid regulator of cardiac output.
-
Hormonal Control: Slower, more sustained effects.
- Catecholamines (Epi, NE): From adrenal medulla; reinforce sympathetic tone.
- Thyroid Hormone (T3/T4): Upregulates myocardial β1 receptors, ↑ CO and sensitivity to catecholamines.
- Glucagon: In β-blocker OD, activates adenylyl cyclase independently of β-receptors → ↑cAMP → ↑HR/inotropy.
⭐ Vagal (parasympathetic) stimulation primarily decreases heart rate (chronotropy) with minimal effect on ventricular contractility (inotropy), as ventricles have sparse vagal innervation.
Measurement - Fick's Slick Trick

- Based on the principle that oxygen uptake by the lungs equals its consumption by the body.
- Calculated as: $CO = \frac{\text{O}_2 \text{ consumption}}{\text{Arterial O}_2 \text{ content} - \text{Mixed Venous O}_2 \text{ content}}$
- Arterial blood is sampled from a systemic artery.
- Mixed venous blood MUST be sampled from the pulmonary artery.
⭐ The use of mixed venous blood from the pulmonary artery is critical, as it represents the average oxygen saturation after tissue extraction throughout the body.
High‑Yield Points - ⚡ Biggest Takeaways
- Cardiac Output (CO) is the product of Heart Rate (HR) and Stroke Volume (SV).
- SV is determined by three key factors: preload, afterload, and contractility (inotropy).
- Preload is the end-diastolic volume that stretches the ventricle; it's primarily set by venous return.
- Afterload is the resistance the heart pumps against, like systemic vascular resistance. ↑ Afterload ↓ SV.
- Contractility is the heart's intrinsic pumping strength. ↑ Contractility ↑ SV.
- Frank-Starling mechanism: ↑ preload leads to ↑ stroke volume.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

