Baroreceptor Basics - The Pressure Sensors
- What: Stretch-sensitive mechanoreceptors in the walls of major arteries.
- Function: Sense moment-to-moment changes in mean arterial pressure (MAP) & pulse pressure.
- ↑ Arterial Pressure → ↑ Stretch → ↑ Afferent firing rate
- ↓ Arterial Pressure → ↓ Stretch → ↓ Afferent firing rate
- Key Locations:
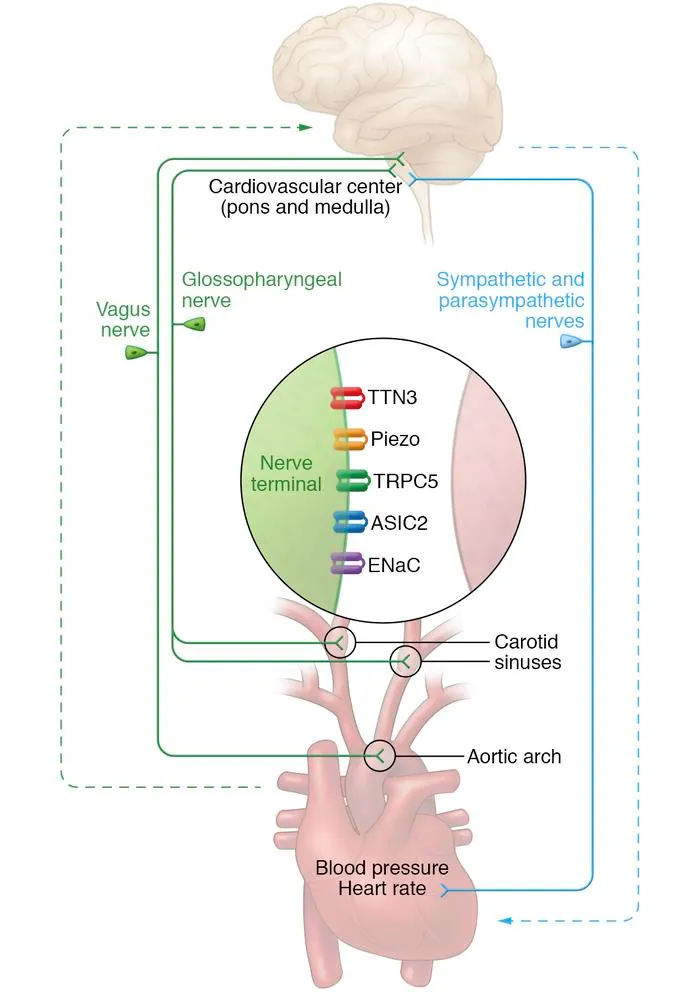
- Carotid Sinus: At the bifurcation of the common carotid artery. Innervated by the glossopharyngeal nerve (CN IX).
- Aortic Arch: Innervated by the vagus nerve (CN X).
⭐ The carotid sinus baroreceptors are most crucial for regulating cerebral blood flow, responding rapidly to both increases and decreases in blood pressure.

Baroreflex Pathway - BP's Balancing Act

- Primary Goal: Maintain stable blood pressure on a beat-to-beat basis.
- Sensors (Mechanoreceptors):
- Carotid Sinus: Responds to both increases (↑) and decreases (↓) in BP. Afferent via Glossopharyngeal nerve (CN IX).
- Aortic Arch: Responds primarily to ↑BP. Afferent via Vagus nerve (CN X).
- Central Integrator: Nucleus Tractus Solitarius (NTS) in the medulla.
⭐ In chronic hypertension, baroreceptors adapt or "reset" to a higher pressure set point, becoming less sensitive to high pressures. This is why the reflex doesn't permanently correct chronic high BP.
Clinical Correlations - When Signals Scramble
-
Carotid Sinus Syncope:
- Hypersensitivity of the carotid sinus baroreceptors, often in older adults.
- Triggers: Shaving, tight collars, head-turning.
- Mechanism: Exaggerated reflex response → abrupt ↑parasympathetic tone (bradycardia) and ↓sympathetic tone (vasodilation) → transient cerebral hypoperfusion → syncope.
-
Orthostatic (Postural) Hypotension:
- Baroreflex impairment on standing; gravity pools blood in lower extremities.
- Causes: Autonomic neuropathy (diabetes), age-related changes, medications (α-blockers), volume depletion.
⭐ A key diagnostic criterion for orthostatic hypotension is a sustained drop in blood pressure within 3 minutes of standing: SBP ↓ by ≥20 mmHg or DBP ↓ by ≥10 mmHg.
- Baroreflex Failure:
- Often iatrogenic (e.g., neck surgery, radiation) or from neurodegeneration.
- Leads to highly volatile blood pressure with labile hypertension and episodes of hypotension.
High‑Yield Points - ⚡ Biggest Takeaways
- Baroreceptors are stretch receptors in the carotid sinus (CN IX) and aortic arch (CN X) that manage beat-to-beat BP.
- High BP increases firing, causing reflex ↓ in HR, contractility, and SVR.
- Low BP decreases firing, causing reflex ↑ in HR, contractility, and SVR.
- Crucial for buffering acute BP fluctuations (e.g., orthostatic changes).
- In chronic hypertension, baroreceptors reset to a higher pressure setpoint.
- Carotid sinus massage mimics high BP to reflexively slow the heart rate.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

