Cardiac Cycle Overview - The Heart's Rhythm
- The cardiac cycle describes the sequence of events in one heartbeat, lasting about 0.8 seconds at 75 bpm.
- Systole: Ventricular contraction and blood ejection.
- Diastole: Ventricular relaxation and filling.
- Cycle length is inversely related to heart rate: $Cycle Length = 60 / Heart Rate$.
- Events on the right side of the heart mirror the left but at lower pressures.
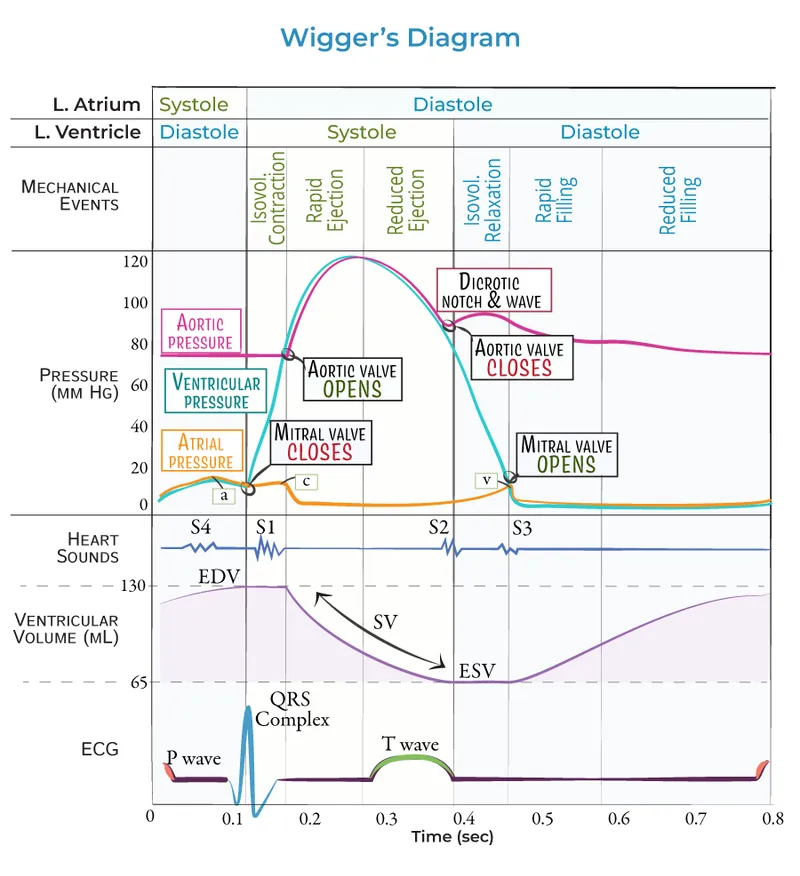
⭐ Clinical Pearl: The third heart sound (S3) is associated with rapid ventricular filling in early diastole, while the fourth heart sound (S4) is from atrial contraction against a stiff ventricle in late diastole.
Ventricular Systole - The Big Squeeze
-
Isovolumetric Contraction (IVC):
- Ventricles contract post-QRS, causing ventricular pressure to exceed atrial pressure.
- Mitral and tricuspid (AV) valves snap shut → S1 heart sound.
- All valves are closed. Ventricular volume is constant (isovolumetric) at its maximum (End-Diastolic Volume).
-
Ventricular Ejection:
- Ventricular pressure rises above aortic/pulmonary artery pressure.
- Aortic and pulmonic (semilunar) valves open.
- Blood is rapidly ejected. Aortic pressure peaks at ~120 mmHg.
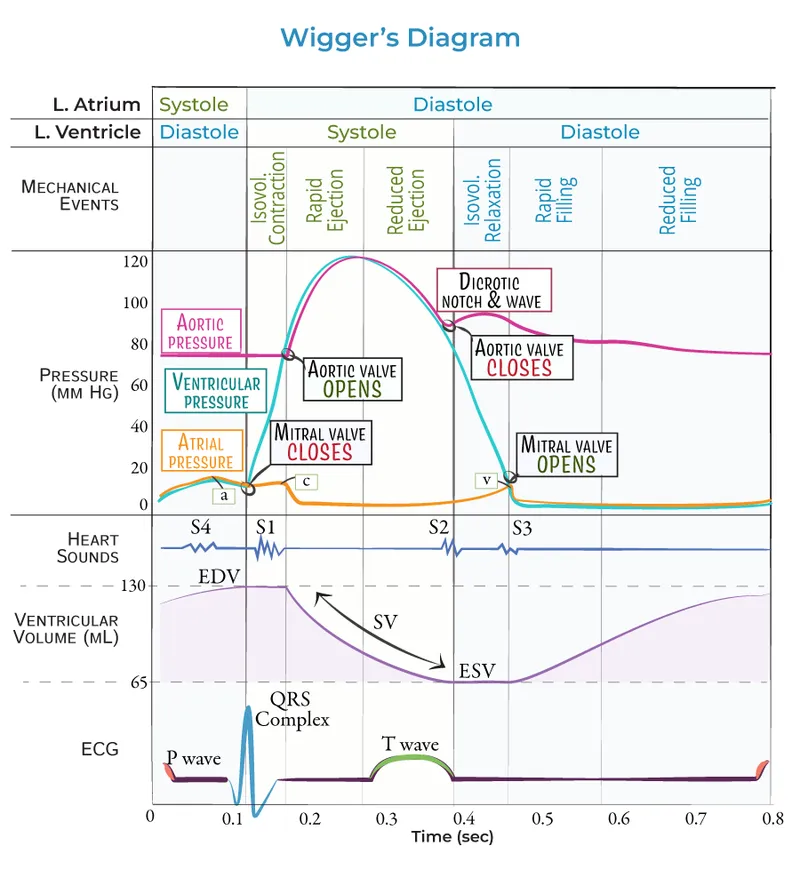
⭐ Increased contractility (e.g., sympathetic stimulation, digoxin) ↑ ejection fraction by ↓ end-systolic volume. The ventricle squeezes more forcefully, leaving less blood behind.
Ventricular Diastole - Relax & Refill
-
Isovolumetric Relaxation:
- Ventricles relax; pressure drops rapidly (↓ Ventricular P).
- Aortic/Pulmonary valves close as ventricular pressure falls below aortic/pulmonic pressure → S2 heart sound.
- All valves are closed; volume is constant (isovolumetric) at End-Systolic Volume (ESV).
-
Ventricular Filling:
- Ventricular P < Atrial P → Mitral/Tricuspid (AV) valves open.
- Rapid Passive Filling: Majority of filling occurs.
- Diastasis (Reduced Filling): Inflow slows as pressures start to equalize.
-
Atrial Systole ("Atrial Kick"):
- Atria contract, pushing final blood volume (~10-20%) into ventricles.
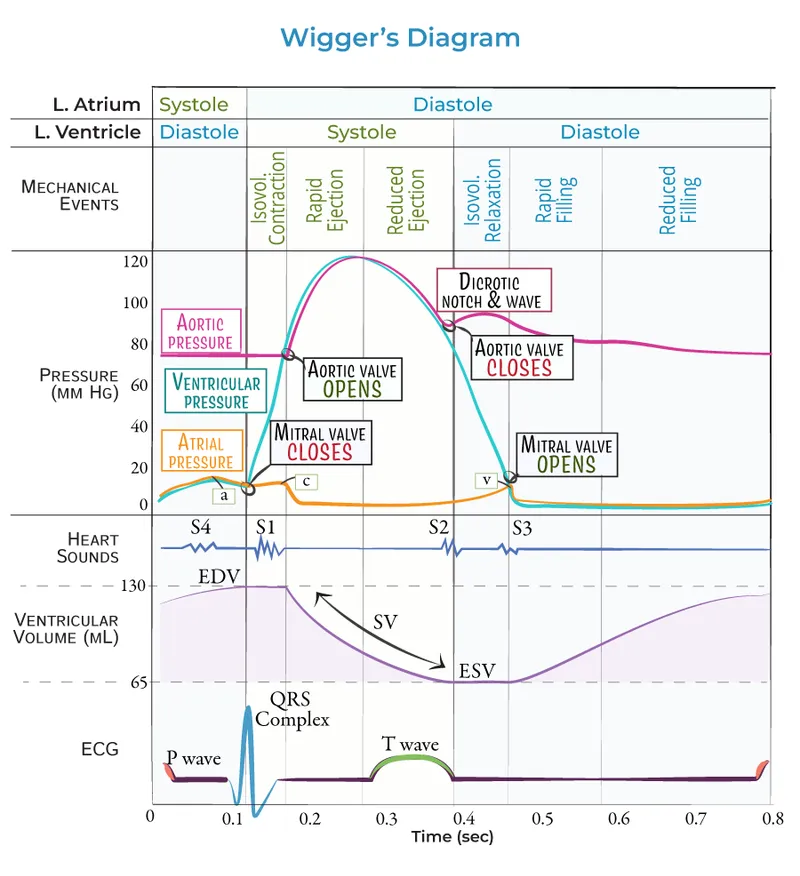
⭐ The atrial kick is crucial in patients with stiff, noncompliant ventricles (e.g., ventricular hypertrophy, elderly). Loss of the kick (as in atrial fibrillation) can significantly reduce cardiac output and cause decompensation.
Wiggers Diagram - The Ultimate Cheat Sheet
- Relates: ECG, heart sounds, pressures (aortic, ventricular, atrial), & ventricular volume.
- Key Events Mapped:
- P wave → Atrial contraction (a-wave).
- QRS complex → Ventricular depolarization → Isovolumetric contraction (S1 sound) → Ejection phase.
- T wave → Ventricular repolarization → Isovolumetric relaxation (S2 sound).
- Valves & Sounds:
- S1: Mitral/Tricuspid valve closure.
- S2: Aortic/Pulmonic valve closure.
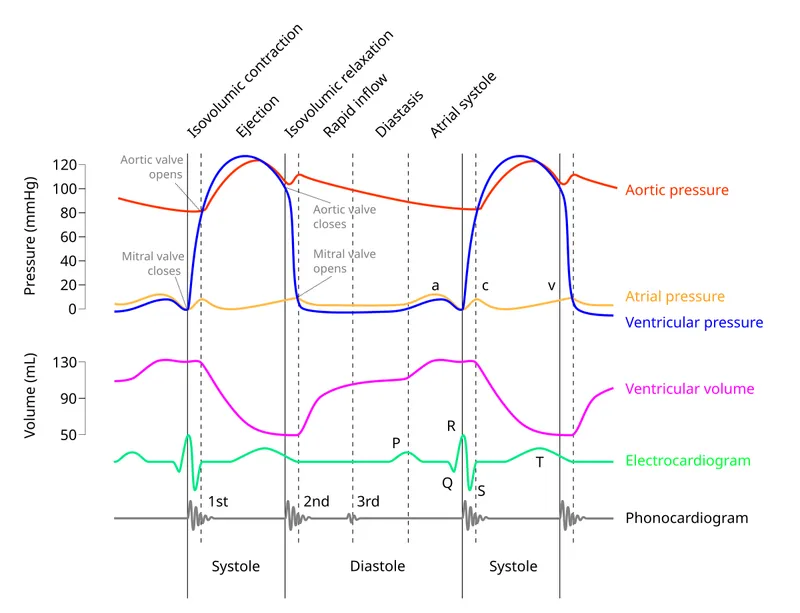
⭐ The dicrotic notch (incisura) on the aortic pressure curve reflects the transient ↑ in aortic pressure upon closure of the aortic valve, marking the beginning of diastole.
- Isovolumetric contraction and relaxation are periods where all four heart valves are closed.
- The S1 sound ("lub") marks the start of systole (mitral/tricuspid valve closure), while the S2 sound ("dub") marks the end of systole (aortic/pulmonic valve closure).
- Most ventricular filling is passive; the atrial kick contributes the final ~20% of ventricular volume.
- The dicrotic notch on the aortic pressure curve corresponds to the closure of the aortic valve.
- Mechanical events of the left heart slightly precede those of the right heart.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

