Isovolumetric Contraction (IVC) - The Big Squeeze
- Definition: Initial phase of systole. Ventricles contract against closed valves, so ventricular volume is constant (iso- = same, -volumetric = volume).
- Events:
- Starts immediately after mitral/tricuspid (AV) valves close (producing S1 heart sound).
- Ventricles contract, causing left ventricular pressure to rise sharply from <10 mmHg to ~80 mmHg.
- Ends when ventricular pressure exceeds aortic/pulmonic pressure, forcing semilunar valves to open.
- EKG Correlation: Corresponds to the QRS complex.
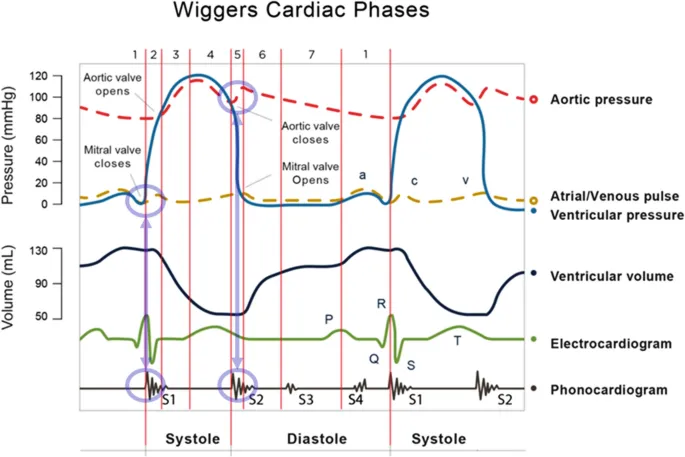
⭐ The duration of IVC is a key indicator of myocardial contractility. It is prolonged by conditions that increase afterload (like hypertension) as the ventricle needs more time to build pressure.
Isovolumetric Relaxation (IVR) - The Chill Out Phase
- Definition: Period between aortic valve closure and mitral valve opening.
- Events:
- Ventricles relax after ejecting blood; pressure plummets (diastole).
- All valves (aortic, pulmonary, mitral, tricuspid) are closed.
- Ventricular volume remains constant at its lowest level (End-Systolic Volume or ESV).
- Heart Sounds: Aortic valve closure creates the second heart sound (S2).
- Pressure Changes: Aortic pressure shows a brief rise (dicrotic notch) from valve closure recoil.
⭐ The v-wave of the jugular venous pressure (JVP) trace peaks during IVR, reflecting the atria filling against a closed tricuspid valve.
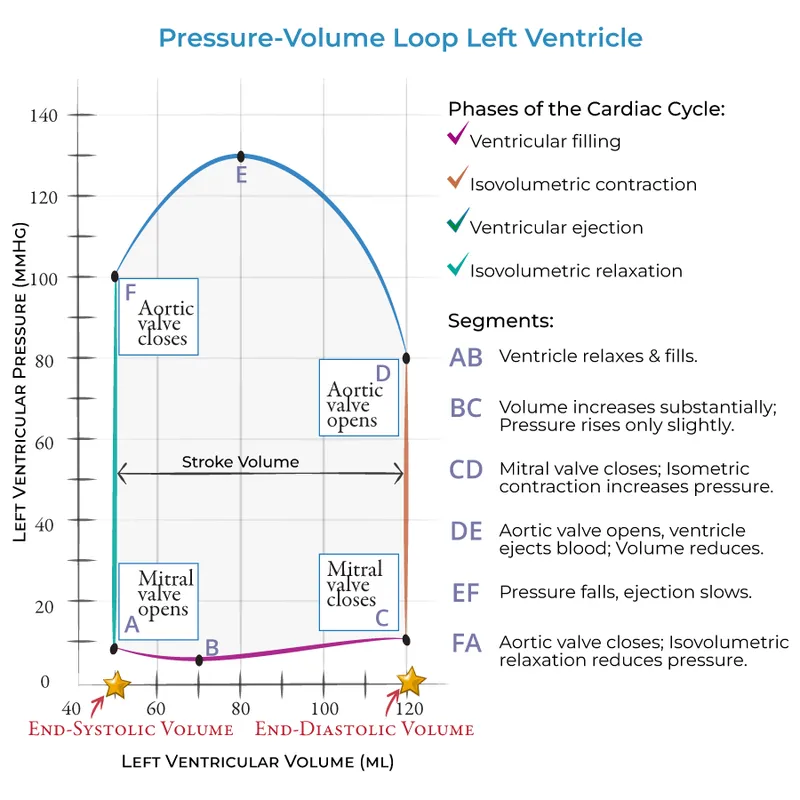
Pressure-Volume Loop - Mapping the Squeeze
Represents one complete cardiac cycle for the left ventricle. The area within the loop signifies the ventricular stroke work.
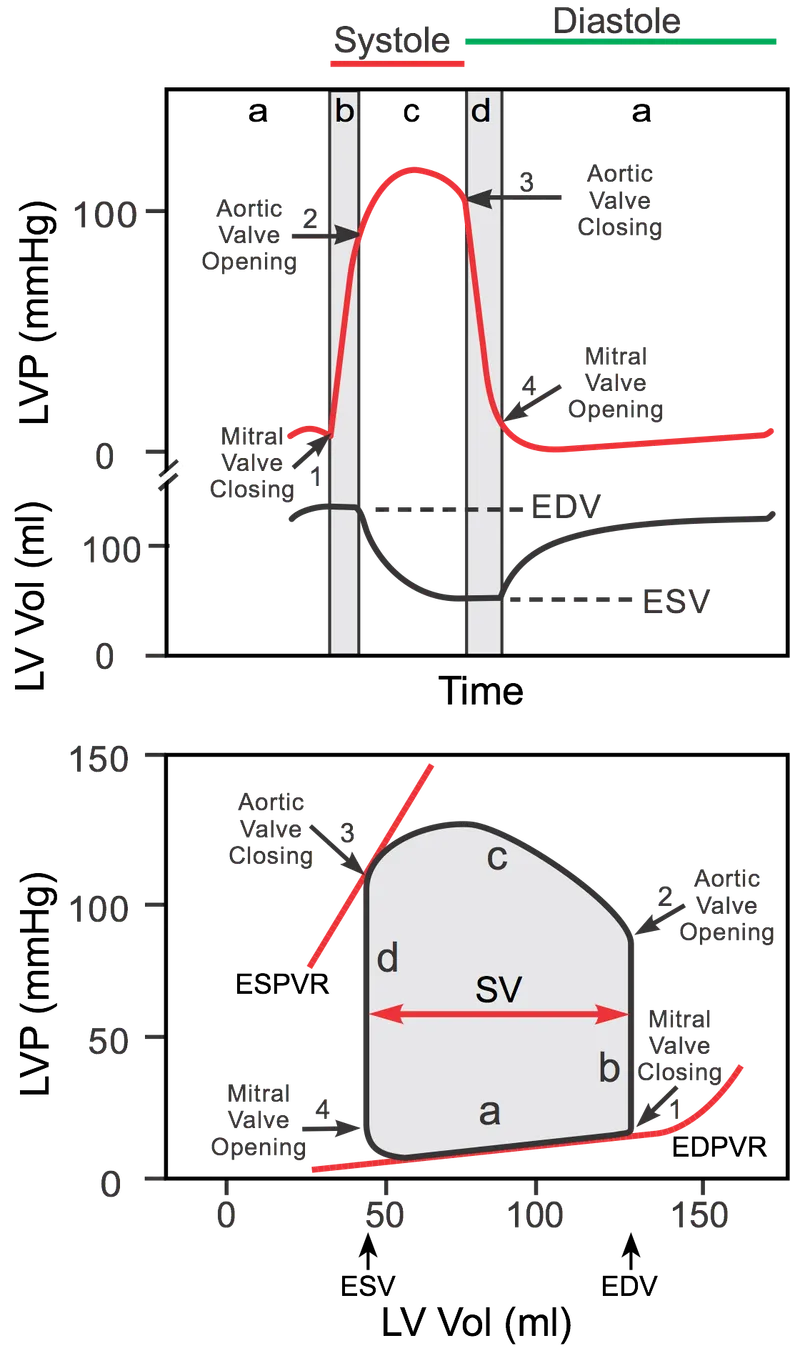
- Phase A → B (Isovolumetric Contraction): Mitral valve closes (S1). Ventricle contracts, pressure ↑, volume is constant.
- Phase B → C (Ejection): Aortic valve opens. Ventricle ejects blood. Volume ↓.
- Phase C → D (Isovolumetric Relaxation): Aortic valve closes (S2). Ventricle relaxes, pressure ↓, volume is constant.
- Phase D → A (Filling): Mitral valve opens. Ventricle fills with blood. Volume ↑.
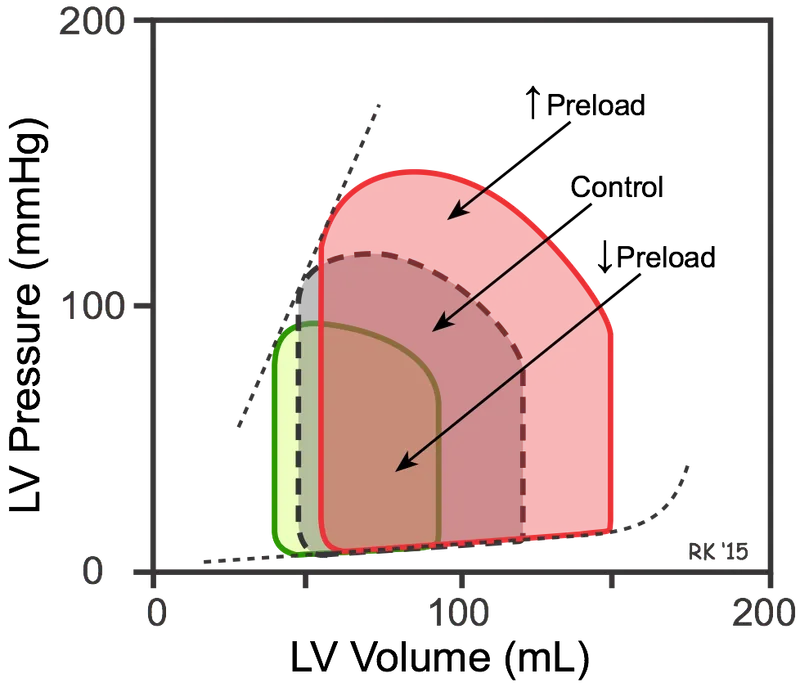
⭐ Exam Favorite: Increased afterload (e.g., hypertension) causes an ↑ in aortic pressure. The ventricle must generate more pressure to open the aortic valve, leading to a ↑ ESV and a ↓ stroke volume, narrowing the PV loop.
Clinical Correlations - Pressure Problems
- ↑ Afterload (e.g., Hypertension, Aortic Stenosis):
- LV must generate much higher pressure to overcome aortic/systemic resistance.
- Prolongs the isovolumetric contraction phase.
- Leads to concentric hypertrophy over time.
- Impaired Myocardial Relaxation (e.g., Diastolic Dysfunction, LVH):
- A stiff ventricle relaxes slowly, increasing the time for pressure to fall.
- Prolongs the isovolumetric relaxation phase.
- Can lead to elevated left atrial pressure.
⭐ In severe aortic stenosis, isovolumetric contraction is markedly prolonged because the LV must generate extreme pressure (e.g., >180 mmHg) to force open the calcified, stenotic aortic valve.
High‑Yield Points - ⚡ Biggest Takeaways
- Isovolumetric contraction is the interval between mitral valve closure (S1) and aortic valve opening.
- During this phase, all four heart valves are closed, and ventricular pressure rapidly increases while volume is constant.
- It aligns with the QRS complex on an EKG.
- Isovolumetric relaxation occurs after aortic valve closure (S2) and ends with mitral valve opening.
- All valves are again closed as ventricular pressure sharply falls with no change in volume.
- This phase corresponds to the latter part of the T wave.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

