Half-Life (t½) - Going Halfsies
- Definition: Time required for a drug's plasma concentration to decrease by 50%.
- A key determinant of the dosing interval and time to reach steady state.
- Calculation: $t_{1/2} = (0.693 \times V_d) / CL$
- $V_d$ = Volume of distribution
- $CL$ = Clearance
- Kinetics & Half-Life:
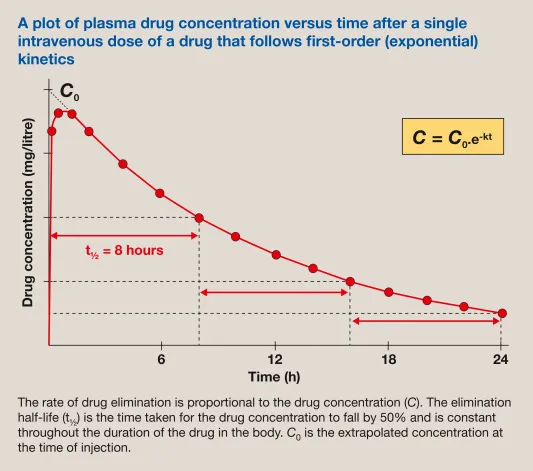
- First-Order: Constant half-life, independent of drug concentration. A constant fraction is eliminated.
- Zero-Order: Half-life varies with concentration. A constant amount is eliminated.
⭐ Rule of Fives: It takes approximately 4-5 half-lives to reach steady-state concentration during continuous infusion, and similarly, 4-5 half-lives to eliminate most of the drug (>90%) after discontinuation.
Steady State (Css) - The Plateau Principle
- Steady state is achieved when the rate of drug administration equals the rate of drug elimination, leading to a constant plasma concentration.
- It takes approximately 4-5 elimination half-lives ($t_{1/2}$) to reach Css, regardless of the dose.
- After 1 $t_{1/2}$ → 50% of Css
- After 2 $t_{1/2}$ → 75% of Css
- After 3 $t_{1/2}$ → 87.5% of Css
- After 4 $t_{1/2}$ → 93.75% of Css
⭐ A loading dose bypasses the accumulation phase to achieve the target plasma concentration ($C_{target}$) faster, but it does not change the time to reach steady state. The maintenance dose dictates the Css.
- For continuous IV infusion: $Css = \text{Infusion Rate} / \text{Clearance}$
Dosing Regimens - The Fast & The Steady
- Loading Dose (LD): The "fast" dose to promptly achieve a target plasma concentration ($C_p$).
- Especially useful for drugs with a long half-life.
- Formula: $LD = (C_p \times V_d) / F$
- $V_d$ = Volume of distribution, $F$ = Bioavailability.
- Maintenance Dose (MD): The "steady" dose to maintain the drug concentration at steady state ($C_{ss}$).
- At $C_{ss}$, Dosing Rate = Rate of Elimination.
- Formula: $MD = (C_{ss} \times CL) / F$
- $CL$ = Clearance.
⭐ A drug reaches steady state concentration in 4-5 half-lives. Similarly, it takes 4-5 half-lives for complete elimination after the drug is stopped.
Clearance & Vd - The Body's Cleanup Crew
- Clearance (CL): The volume of plasma cleared of a drug per unit time (e.g., L/hr or mL/min). It represents the efficiency of drug elimination.
- Formula: $CL = (\text{Rate of elimination}) / C$
- Volume of Distribution (Vd): The theoretical fluid volume that would be required to contain the total amount of drug in the body at the same concentration as in the plasma.
- Formula: $Vd = (\text{Amount of drug in body}) / C$
⭐ Drugs with a high Vd are extensively distributed into tissues and are not efficiently removed by dialysis.
High‑Yield Points - ⚡ Biggest Takeaways
- Half-life (t½) is the time for a drug's plasma concentration to decrease by 50%.
- Reaching steady-state concentration (Css) requires approximately 4 to 5 half-lives of continuous dosing.
- Complete drug elimination from the body also takes about 4 to 5 half-lives after the final dose.
- A loading dose is administered to rapidly achieve the desired plasma concentration, bypassing the usual multi-half-life wait.
- In first-order kinetics, t½ is constant; in zero-order kinetics, a constant amount is eliminated, so t½ varies.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

