Estrogens - The Feminine Architects
- Types: Estradiol (most potent), estrone, and estriol. Synthesized from androgens by aromatase.
- Mechanism: Binds to nuclear estrogen receptors (ER-α, ER-β) to modulate gene transcription.
- Key Effects:
- Promotes development of female secondary sexual characteristics.
- Stimulates endometrial proliferation.
- Maintains bone density by ↓ osteoclast activity.
- ↑ HDL & ↓ LDL; ↑ coagulation factors (risk of thrombosis).
- Clinical Uses:
- Hormone replacement therapy (HRT) in menopause.
- Combined oral contraceptives.
- Primary hypogonadism.
⭐ Unopposed estrogen therapy (without progestin) significantly increases the risk of endometrial cancer in women with a uterus.
Progestins - The Cycle Stabilizers
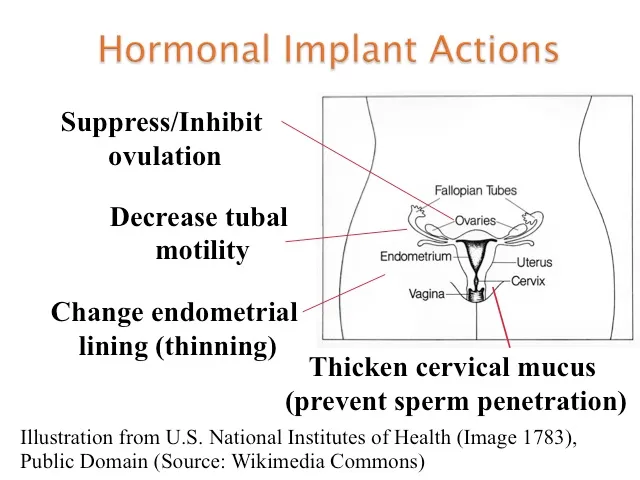
- Mechanism: Bind progesterone receptors → ↓ GnRH pulse frequency, thicken cervical mucus, and decidualize the endometrium, making it hostile to implantation.
- Agents: Levonorgestrel, medroxyprogesterone acetate, etonogestrel, norethindrone.
- Clinical Use: Contraception (alone or combined), HRT (to oppose estrogen), dysfunctional uterine bleeding (DUB), endometriosis.
- Adverse Effects: Breakthrough bleeding, headache, weight gain. ⚠️ Depot medroxyprogesterone acetate (DMPA) may cause ↓ bone mineral density.
⭐ Progestin Challenge Test: Used to evaluate amenorrhea. Withdrawal bleeding after a progestin course indicates anovulation with adequate estrogen. No bleeding suggests low estrogen or an outflow tract obstruction.
SERMs & Antagonists - The Hormone Hackers
| Drug | Mechanism | Agonist Activity | Antagonist Activity | Clinical Use |
|---|---|---|---|---|
| Tamoxifen | SERM | Bone, Endometrium | Breast | ER+ breast cancer. ⚠️ ↑ risk of endometrial cancer & DVT. |
| Raloxifene | SERM | Bone | Breast, Endometrium | Osteoporosis, breast cancer prophylaxis. |
| Clomiphene | SERM | - | Hypothalamus | Ovulation induction (PCOS); blocks E₂ negative feedback, ↑FSH/LH. |
| Anastrozole | Aromatase Inhibitor | - | - | ER+ breast cancer (postmenopausal). Blocks peripheral estrogen production. |
| Mifepristone | Progestin Antagonist | - | Progesterone Receptors | Pregnancy termination; causes decidual necrosis. |
Contraception - The Cycle Controllers
- Combined Hormonal Contraceptives (CHCs): Estrogen + Progestin
- Mechanism: Suppress GnRH, LH & FSH secretion → inhibit ovulation.
- Also thicken cervical mucus & alter the endometrium, making it hostile to implantation.
- Progestin-Only Contraceptives (POPs or "Minipill")
- Mechanism: Primarily thicken cervical mucus. Ovulation is inhibited inconsistently.
- Fewer contraindications than CHCs, especially regarding thrombosis risk.
⭐ The estrogen component of CHCs increases the risk of venous thromboembolism (VTE), MI, and stroke. This risk is significantly amplified in women >35 years of age who smoke.
High‑Yield Points - ⚡ Biggest Takeaways
- Unopposed estrogen significantly increases the risk of thromboembolic events and endometrial cancer.
- Tamoxifen acts as a breast antagonist but a uterine agonist, raising endometrial cancer risk.
- Raloxifene is a bone agonist used for osteoporosis and does not carry the same uterine risk.
- Clomiphene induces ovulation by acting as a hypothalamic estrogen antagonist.
- Progestins are key for contraception and endometrial protection from unopposed estrogen.
- Aromatase inhibitors like anastrozole treat ER+ breast cancer in postmenopausal women.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

