Cardiac Action Potential - The Heart's Electrical Dance
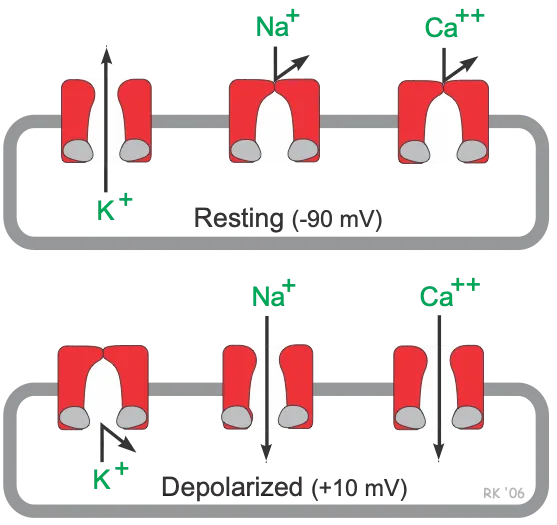
- Non-pacemaker (Ventricular/Atrial): Fast response, stable Phase 4.
- Pacemaker (SA/AV nodes): Slow response, unstable Phase 4 (funny current, $I_f$)
⭐ The slope of Phase 4 in pacemaker cells determines the heart rate. Steeper slope = faster heart rate.
Class I Agents - Salty Blockade Crew
- Mechanism: State-dependent Na⁺ channel blockade, slowing the phase 0 upstroke. This decreases conduction velocity in non-nodal tissue.
- Subclasses are based on the strength of blockade and effect on action potential duration (APD).
- IA (e.g., Quinidine, Procainamide): Moderate blockade; ↑ APD.
- IB (e.g., Lidocaine, Mexiletine): Weak blockade; ↓ APD. Targets ischemic tissue.
- IC (e.g., Flecainide, Propafenone): Strong blockade; no change in APD.
📌 Mnemonic: "Queen Proclaims Diso's pyramid" (IA), "Lettuce & Mayo" (IB), "Fries Please" (IC).
⭐ Use-Dependence: Blockade intensifies with faster heart rates. Class IC has the strongest use-dependence and is contraindicated post-MI due to increased mortality from proarrhythmia.
Class II Agents - Beta Block Party
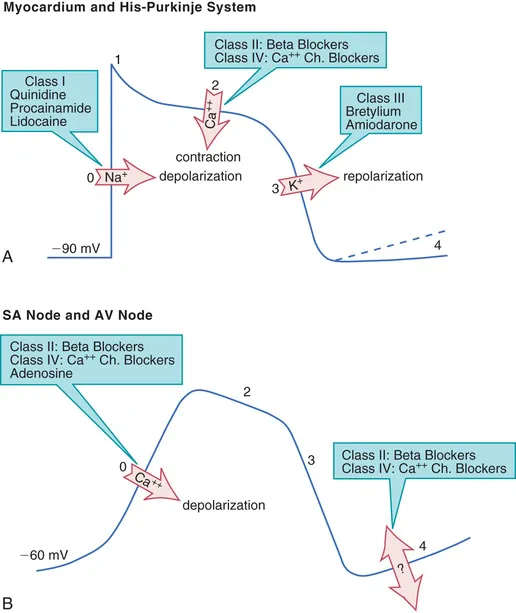
- Mechanism: Primarily act on nodal tissue by blocking β-adrenergic receptors. This ↓ cAMP, leading to ↓ Ca²⁺ currents.
- Slows phase 4 diastolic depolarization (pacemaker potential).
- Increases PR interval.
- Agents: Metoprolol, Labetalol, Propranolol, Esmolol (short-acting).
- Use: Rate control (atrial fibrillation/flutter), post-MI, thyrotoxicosis.
⭐ Esmolol's very short half-life makes it ideal for critically ill patients or when short-term β-blockade is desired.
Class III Agents - K+ Channel Kickers
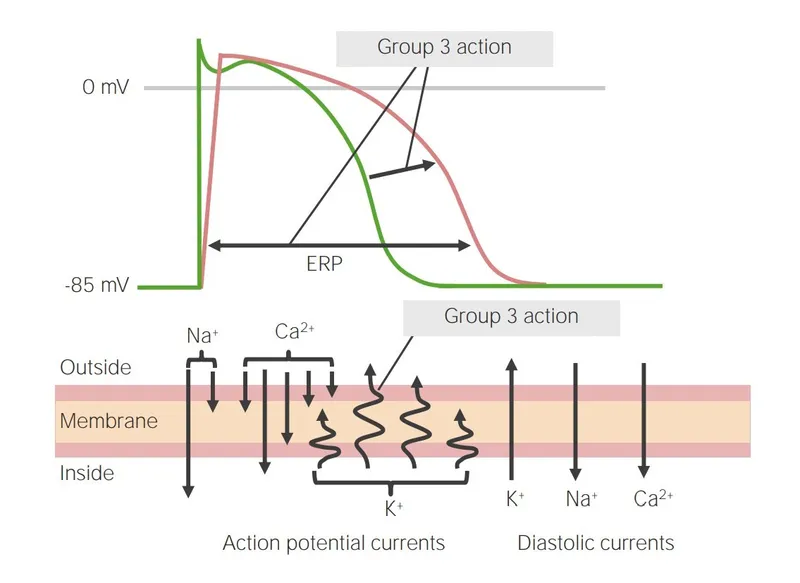
- Mechanism: Block delayed rectifier K+ channels ($I_K$).
- Effect: Prolong action potential duration (APD) & effective refractory period (ERP).
- EKG: ↑ QT interval.
- Agents: Amiodarone, Ibutilide, Dofetilide, Sotalol (📌 AIDS).
- Toxicity: Risk of Torsades de Pointes (TdP) due to QT prolongation.
⭐ Amiodarone uniquely exhibits effects of all four antiarrhythmic classes. Monitor for its classic pulmonary fibrosis, hepatotoxicity, and thyroid dysfunction (hypo/hyper).
Class IV Agents - Calcium Channel Chillers
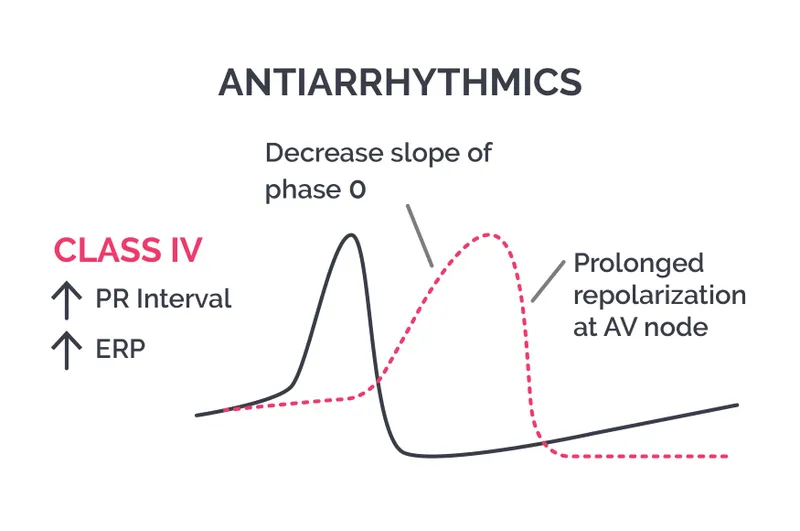
- Mechanism: Block voltage-gated L-type Ca²⁺ channels, primarily affecting SA and AV nodes.
- Effect: Slows phase 4 spontaneous depolarization and phase 0 upstroke. This leads to ↓ heart rate and ↓ conduction velocity.
- EKG: ↑ PR interval.
- Agents: Verapamil, Diltiazem.
⭐ Use-dependence: These drugs show greater effect at faster heart rates, as they bind more effectively to open or inactivated Ca²⁺ channels.
Other Agents - The Odd Squad
- Adenosine: Activates A1 receptors → ↑ K+ out, ↓ Ca2+ in → hyperpolarizes AV node. Terminates SVT. Effects blunted by caffeine/theophylline.
- Magnesium ($Mg^{2+}$): Blocks influx through L-type Ca2+ channels. Drug of choice for Torsades de Pointes.
- Ivabradine: Inhibits funny current ($I_f$) in SA node.
⭐ Adenosine causes transient asystole for diagnostics and can provoke bronchospasm in asthmatics.
High‑Yield Points - ⚡ Biggest Takeaways
- Class I drugs exhibit use-dependence, preferentially targeting channels in rapidly depolarizing tissue.
- Class II (β-blockers) and Class IV (Ca²⁺ blockers) primarily slow conduction through the AV node, increasing the PR interval.
- Class III K⁺ blockers prolong the action potential, which increases the QT interval and the risk of Torsades de Pointes.
- Amiodarone has properties of all four classes and carries significant pulmonary and thyroid toxicity.
- Adenosine is extremely short-acting, used to terminate supraventricular tachycardias.
- Digoxin increases vagal tone to slow AV conduction in atrial fibrillation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

