RSV Overview - The Tiny Terror
- Virus: Enveloped, negative-sense, single-stranded RNA paramyxovirus.
- Pathogenesis: Infects respiratory epithelium, causing cell fusion and formation of large multinucleated cells (syncytia). This leads to inflammation, mucus production, and airway obstruction.
- Clinical: Leading cause of bronchiolitis and pneumonia in infants <1 year old. Presents with fever, cough, wheezing, and respiratory distress.
- Seasonality: Peaks in winter months.
⭐ High-Yield: RSV is the most common cause of lower respiratory tract illness (LRTI) in children worldwide, hospitalizing millions annually.
Monoclonal Antibodies - Protein Bodyguards
*Passive immunity via lab-engineered antibodies to prevent severe RSV disease in high-risk infants. These do not treat active infection.
-
Palivizumab
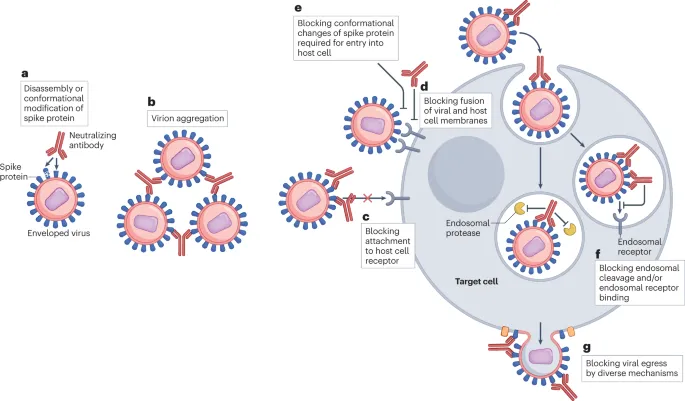
- Mechanism: Humanized IgG1 monoclonal antibody that targets a specific epitope (site A) on the RSV fusion (F) protein. This blocks viral entry into host cells.
- Indication: Prophylaxis for infants at high risk:
- Preterm infants (< 29 weeks gestation)
- Chronic Lung Disease of Prematurity (CLDP)
- Hemodynamically significant congenital heart disease.
- Administration: Given as a monthly intramuscular (IM) injection throughout the RSV season (typically November to March).
-
Nirsevimab
- Mechanism: Next-generation monoclonal antibody, also targets the F protein.
- Advantage: Longer half-life due to a modified Fc region, requiring only a single IM dose for the entire RSV season.
⭐ High-Yield: Palivizumab is a prophylactic antibody, not a vaccine. It provides passive immunity but does not induce an active, long-term memory immune response from the host.
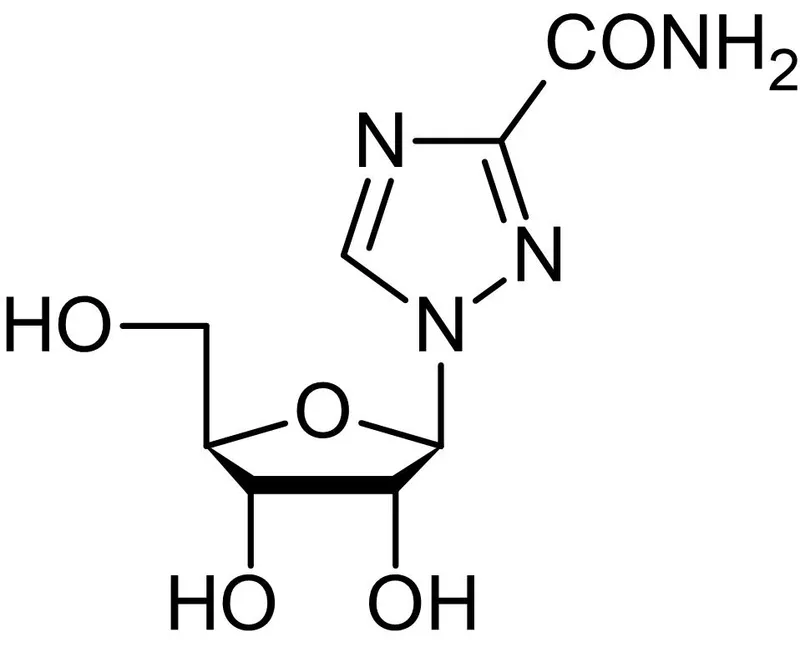
Ribavirin - The Risky Rescue
- Mechanism: Guanosine analog; inhibits viral RNA polymerase & IMP dehydrogenase, depleting GTP and causing lethal viral mutations.
- Use: Reserved for severe RSV infections in immunocompromised adults (e.g., transplant patients). Aerosolized administration.
- Toxicity:
- ⚠️ Extreme Teratogen: Contraindicated in pregnancy (patient or partner).
- Dose-dependent hemolytic anemia.
- Bronchospasm (inhaled route).
⭐ Ribavirin's most tested adverse effect is its teratogenicity, requiring strict contraception for both male and female patients during and for 6 months after therapy.
📌 Mnemonic: RIBA
- RNA polymerase inhibitor
- IMP Dehydrogenase inhibitor
- Bad for Baby
- Anemia
High‑Yield Points - ⚡ Biggest Takeaways
- Palivizumab is a monoclonal antibody used for prophylaxis in high-risk infants; it is not a treatment for active infection.
- It targets the RSV F protein, preventing viral fusion and entry.
- Ribavirin is reserved for severe RSV infections, primarily in immunocompromised patients.
- A major adverse effect of Ribavirin is teratogenicity, making it contraindicated in pregnancy.
- The mechanism of Ribavirin involves inhibiting inosine monophosphate dehydrogenase, depleting GTP.
- Supportive care remains the primary management for most RSV cases.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

