Indications - Why Double Up?
- Synergism (1+1 > 2): To achieve a more effective bactericidal effect.
- e.g., Beta-lactam + Aminoglycoside for Enterococcal endocarditis.
- Empiric "Broad-Spectrum" Coverage: In critically ill patients (e.g., septic shock, neutropenic fever) before the pathogen is identified.
- Prevent Resistance: To suppress the emergence of resistant microbial strains.
- e.g., Multi-drug therapy for Tuberculosis (RIPE).
- Polymicrobial Infections: To cover multiple pathogens with different susceptibility profiles.
- e.g., Intra-abdominal abscesses.
⭐ Exam Favorite: Cell wall agents (Penicillins, Vancomycin) damage the bacterial cell wall, which ↑ the intracellular uptake of aminoglycosides, leading to a synergistic bactericidal effect.
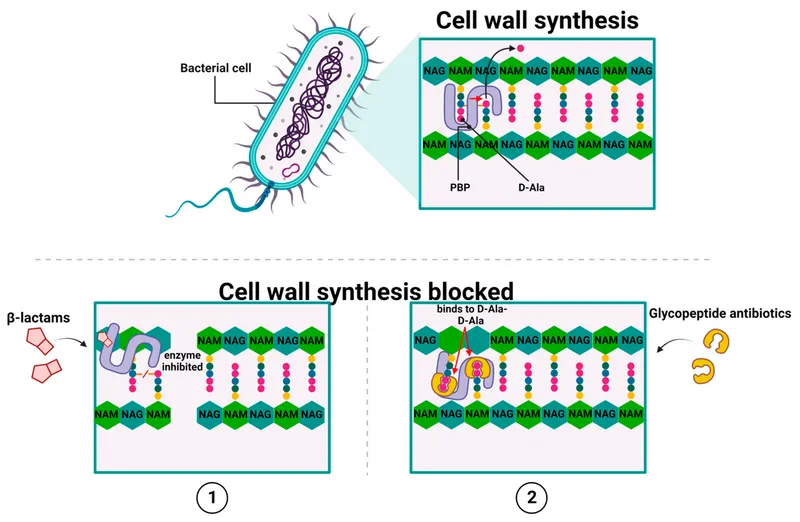
Mechanisms of Interaction - Better Together
Synergism: Combined effect is greater than the sum of individual effects ($1+1 > 2$).
-
Sequential Blockade: Inhibiting successive steps in one metabolic pathway.
- Example: Trimethoprim-Sulfamethoxazole (TMP-SMX) blocks sequential steps in folate synthesis.
-
Inhibition of Enzymatic Inactivation: One drug protects the active drug from enzymes.
- Example: Clavulanate (a β-lactamase inhibitor) protects Amoxicillin from inactivation by β-lactamase.
-
Enhanced Antimicrobial Uptake: One drug facilitates the entry of another.
- Example: Penicillins or Vancomycin damage the cell wall, ↑ uptake of Aminoglycosides.
⭐ The combination of a cell wall synthesis inhibitor (like Ampicillin or Vancomycin) and an aminoglycoside (like Gentamicin) is a classic synergistic pairing essential for treating infective endocarditis, especially by Enterococcus species.
Synergistic Pairs - The A-Team
-
Beta-lactams + Aminoglycosides
- Mechanism: Beta-lactam damages the bacterial cell wall, facilitating the entry of the aminoglycoside, which then inhibits protein synthesis at the 30S ribosome. Essential for gram-positive synergy.
-
Trimethoprim + Sulfamethoxazole (TMP-SMX)
- Mechanism: Sequential blockade of folate synthesis. Sulfamethoxazole inhibits dihydropteroate synthase; trimethoprim inhibits dihydrofolate reductase.
-
Amphotericin B + Flucytosine
- Mechanism: Amphotericin B creates pores in the fungal cell membrane, increasing entry of flucytosine which inhibits fungal DNA and RNA synthesis.
-
Quinupristin + Dalfopristin (Streptogramins)
- Mechanism: Bind to separate sites on the 50S ribosomal subunit, synergistically interrupting protein synthesis.
⭐ For serious enterococcal infections (e.g., endocarditis), aminoglycosides are combined with a cell wall active agent (penicillin or vancomycin). This is crucial as enterococci have low-level intrinsic resistance to aminoglycosides; the cell wall agent facilitates aminoglycoside entry.
Disadvantages - When More is Less
- ↑ Toxicity & Adverse Effects: Cumulative risk from multiple agents (e.g., aminoglycoside + vancomycin nephrotoxicity).
- Antagonism: Efficacy of one drug is reduced by another.
- Bacteriostatic drugs (e.g., tetracycline) inhibit bactericidal drugs (e.g., penicillin) that require cell growth.
- Superinfection: Elimination of normal flora risks opportunistic infections like C. difficile.
- Promotes Resistance: Encourages multidrug-resistant (MDR) organism emergence.
⭐ Avoid combining penicillins (bactericidal) with tetracyclines (bacteriostatic). The bacteriostatic effect halts the cell division required for penicillin efficacy, risking treatment failure.
High‑Yield Points - ⚡ Biggest Takeaways
- Synergy is the primary goal, where the combined effect is greater than the sum of individual effects (1+1 > 2).
- Classic synergy: Aminoglycosides + β-lactams (e.g., Penicillin) for enhanced uptake, crucial for Enterococcal endocarditis.
- Sequential blockade: Trimethoprim-Sulfamethoxazole inhibits two key steps in bacterial folate synthesis.
- Antagonism is a risk, especially combining bacteriostatic (e.g., tetracycline) with bactericidal (e.g., penicillin) agents.
- Key uses: Broaden empiric coverage (sepsis), prevent resistance (TB, HIV), and treat polymicrobial infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

