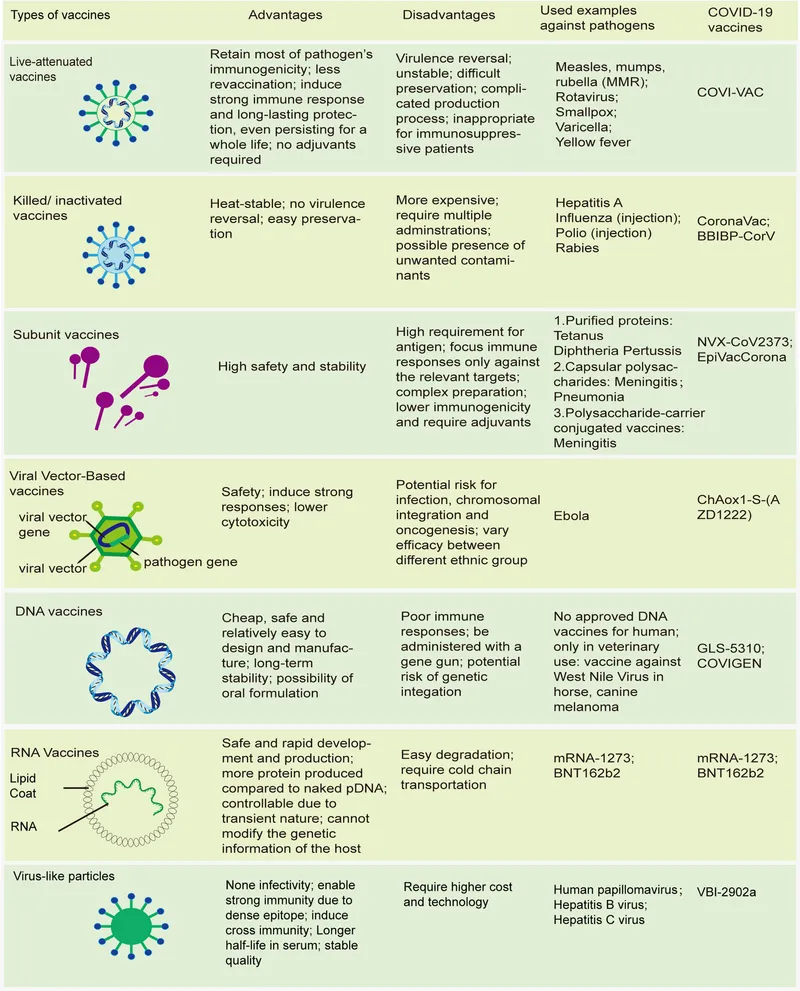
Live vs Inactivated - The Great Divide
A fundamental concept distinguishing vaccine types is crucial for understanding schedules, contraindications, and immune response.
| Feature | Live Attenuated Vaccines | Inactivated (Killed) Vaccines |
|---|---|---|
| Composition | Weakened (attenuated) pathogen | Whole or fractional killed pathogen |
| Booster Doses | Single dose often sufficient | Multiple doses & boosters needed |
| Immunity | Humoral & Cellular (IgG, IgA) | Mainly Humoral (IgG) |
| Durability | Long-lasting, often lifelong | Shorter duration, immunity wanes |
| Safety | Risk of reversion to virulence | No risk of causing disease |
| Contraindication | Immunocompromised, Pregnancy | Safe in immunodeficiency |
| Stability | Less stable (requires cold chain) | More stable |
| Adjuvant | Not required | Required to enhance immunogenicity |
⭐ High-Yield: Live attenuated vaccines produce a strong, long-lasting cellular (T-cell) and humoral (antibody) immune response, mimicking natural infection. Inactivated vaccines primarily stimulate a humoral response.
Live Vaccines - The Attenuated Crew
- Mechanism: Weakened (attenuated) but viable organisms that replicate in the host.
- Immunity: Potent, long-lasting; stimulates both humoral (IgG, IgA) & cell-mediated immunity. Often single-dose efficacy (exceptions: oral vaccines).
- Risks: Potential to revert to virulence; risk of disease in immunocompromised hosts.
- Contraindications: Pregnancy, immunodeficiency (e.g., SCID, HIV with CD4 < 200/μL).
- Examples: 📌 Roman Is Best Man To Call Your Vacancy: Rotavirus, Influenza (nasal), BCG, Measles, Mumps, Rubella, Typhoid (oral), Cholera (oral), Yellow Fever, Varicella.
⭐ Sabin (Oral Polio Vaccine - OPV) can rarely revert to cause Vaccine-Associated Paralytic Poliomyelitis (VAPP).
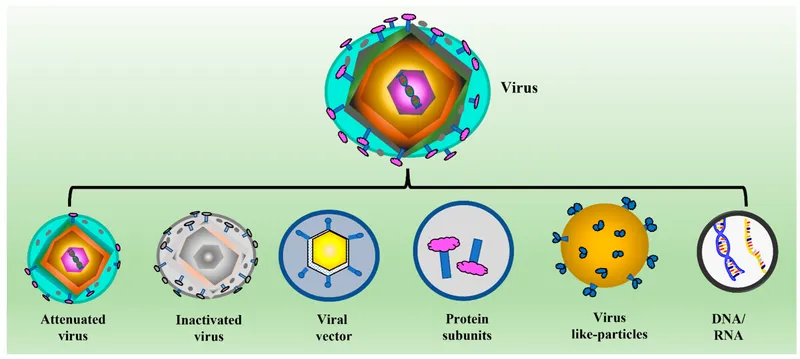
Inactivated Vaccines - The Killed Squad
- Made from whole bacteria/viruses killed by heat or chemicals (e.g., formalin). Cannot replicate or cause disease, making them safer.
- Immunity Profile:
- Less immunogenic than live vaccines.
- Require multiple doses & adjuvants (e.g., alum) to boost response.
- Primarily stimulate humoral (antibody) immunity; weak cell-mediated immunity.
- Shorter-lasting immunity, needing booster doses.
- 📌 Mnemonic: "R.I.P. H.A." → Rabies, Influenza (injectable), Polio (Salk), Hepatitis A.
- Examples (Bacterial): Whole-cell Pertussis, Typhoid, Cholera.
⭐ Inactivated vaccines predominantly induce a Th2-mediated response, leading to humoral immunity (antibody production), unlike live vaccines which stimulate a broader Th1 and Th2 response.

Contraindications - Handle With Care
- Live Vaccines:
- Anaphylaxis to a vaccine component.
- Pregnancy (theoretical risk to fetus).
- Severe immunodeficiency (e.g., SCID, high-dose steroids >2 mg/kg/day for >14 days, chemotherapy).
- Inactivated Vaccines:
- Severe anaphylaxis to a previous dose is the only true contraindication.
- Moderate-to-severe illness is a precaution (defer until stable).
⭐ Withhold live vaccines (MMR, Varicella) for 3-11 months after immunoglobulin/blood product administration.
High‑Yield Points - ⚡ Biggest Takeaways
- Live attenuated vaccines provide stronger, lifelong immunity (Cell-Mediated & Humoral) but risk causing disease in immunocompromised patients.
- Inactivated vaccines are safer but offer weaker, shorter-lived immunity (mainly Humoral), requiring multiple doses and boosters.
- Live vaccines are generally not given to pregnant women or immunocompromised individuals.
- Inactivated vaccines are the preferred choice in pregnancy and immunosuppression.
- Antibody interference can affect the efficacy of live vaccines.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

