Global Vax Orchestrators - WHO's Grand Plan
- WHO - Expanded Programme on Immunization (EPI): Launched in 1974. Aims to ensure universal access to all relevant vaccines for all at risk.
- Gavi, the Vaccine Alliance: A public-private partnership. Key functions include financing new/underused vaccines, strengthening health systems, and shaping vaccine markets.
- Immunization Agenda 2030 (IA2030): The current global strategy. Vision: "A world where everyone, everywhere, at every age, fully benefits from vaccines for good health and well-being."
⭐ IA2030 Target: Aims to prevent over 50 million deaths through vaccination by 2030.
Disease Eradication Efforts - Endgame for Germs
- Eradication: Permanent reduction to zero of the worldwide incidence of infection caused by a specific agent. Intervention measures are no longer needed.
- Elimination: Reduction to zero of the incidence of a specified disease in a defined geographical area. Continued intervention is required to prevent re-establishment.
- Diseases Eradicated
- Smallpox (1980): The only human disease successfully eradicated globally.
- Rinderpest (Cattle plague, 2011): Second disease eradicated.
- Eradication Targets
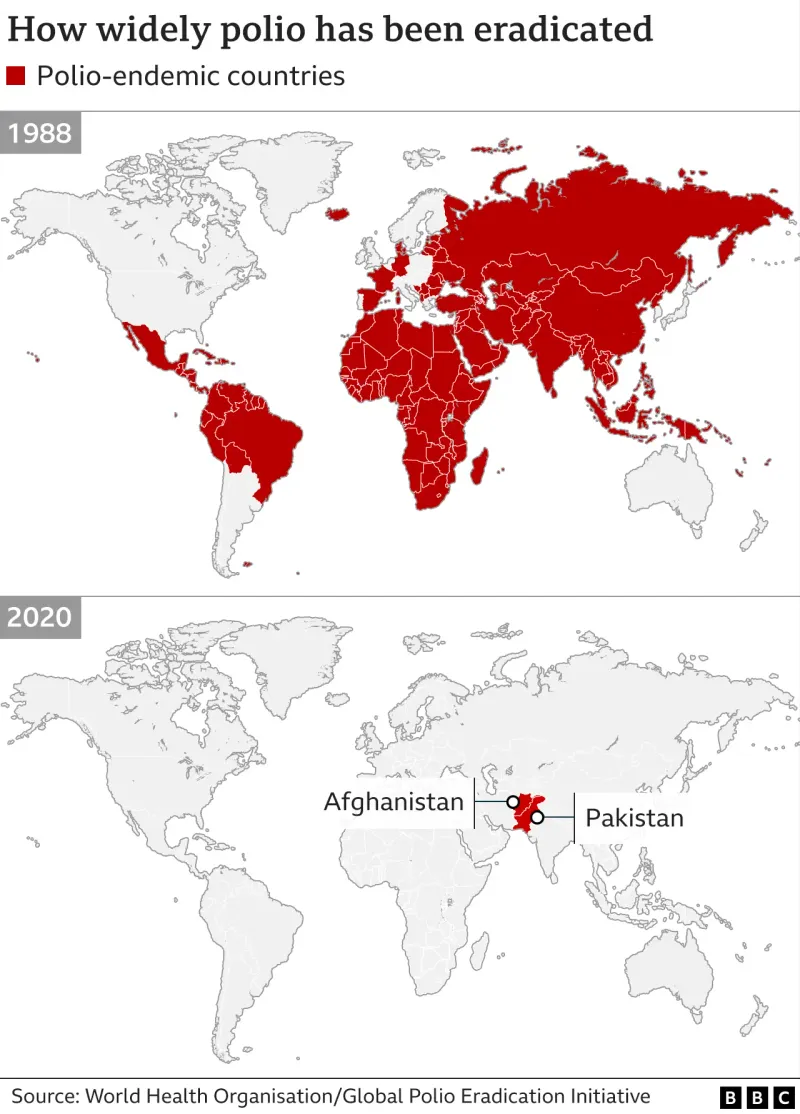
- Poliomyelitis: GPEI Endgame Strategy focuses on switching from tOPV to bOPV, and finally to an IPV-only schedule.
- Guinea Worm (Dracunculiasis): Nearing eradication, with cases confined to a few African countries.
⭐ For a disease to be eradicable, it must have: no non-human reservoir, an effective intervention (e.g., vaccine), and specific diagnostic tools to detect cases.
Modern Vax Alliances - Pandemic Power-Ups
-
Gavi (The Vaccine Alliance): A public-private partnership focused on increasing vaccine access in low-income countries. Core partners include WHO, UNICEF, the World Bank, and the Bill & Melinda Gates Foundation.
-
CEPI (Coalition for Epidemic Preparedness Innovations): A global alliance that finances and coordinates the development of new vaccines to prevent and contain infectious disease epidemics.
-
COVAX (COVID-19 Vaccines Global Access): Co-led by Gavi, CEPI, and WHO, it was the vaccines pillar of the Access to COVID-19 Tools (ACT) Accelerator, aimed at ensuring equitable global distribution of COVID-19 vaccines.
⭐ CEPI's "100 Days Mission" is a key global health security goal, aiming to have safe, effective vaccines ready for manufacturing at scale within 100 days of a pandemic threat being identified.
India's UIP & Global Sync - Desi Vax, Global Beat
- Universal Immunization Programme (UIP): India's cornerstone program, providing free, universal access to vaccines nationwide.
- Key Introductions: Pentavalent, Rotavirus, PCV, Measles-Rubella (MR).
- Mission Indradhanush (MI): Special drives to achieve >90% full immunization coverage.
- GAVI (The Vaccine Alliance): Key global partner supporting UIP by co-financing newer, expensive vaccines (e.g., PCV, Rotavirus).
- CEPI (Coalition for Epidemic Preparedness Innovations): Global alliance accelerating vaccine development for epidemic threats; India is a founding member.
⭐ GAVI support is time-limited. As a country's economy (GNI) grows, it transitions to self-financing. India is in an accelerated transition phase.
High-Yield Points - ⚡ Biggest Takeaways
- The Universal Immunization Programme (UIP) was launched in 1985 to provide free, universal vaccination against key diseases.
- Mission Indradhanush (MI), launched in 2014, targets unvaccinated/partially vaccinated children and pregnant women to boost coverage.
- India was declared polio-free by the WHO in March 2014; the last case was reported in January 2011.
- Newer vaccines like Pentavalent, Rotavirus, and Pneumococcal Conjugate Vaccine (PCV) are now part of the national schedule.
- GAVI (The Vaccine Alliance) is a key global partner supporting India's immunization program.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

