PALS Basics - The First Few Seconds
-
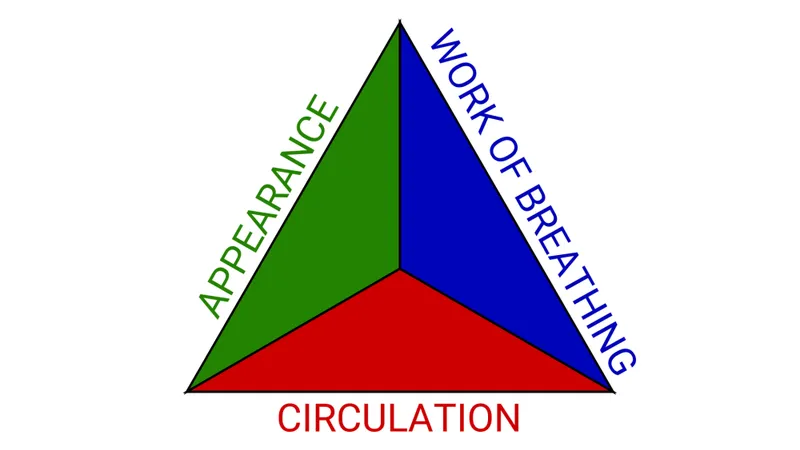
Initial Impression (First 60s): Use the Pediatric Assessment Triangle (PAT) to assess severity.
- Appearance: Tone, Interactiveness, Consolability, Look/Gaze, Speech/Cry (📌 TICLS).
- Work of Breathing: Rate, retractions, abnormal sounds.
- Circulation to Skin: Pallor, mottling, cyanosis.
-
Immediate Sequence:
⭐ If pulse is <60/min with poor perfusion despite oxygenation & ventilation, START chest compressions.
Bradycardia & Tachycardia - When the Heart Skips
-
Bradycardia (HR <60/min): Primarily caused by hypoxia. Always manage Airway & Breathing first.
- If HR remains <60/min with poor perfusion despite oxygenation & ventilation, start chest compressions.
- Epinephrine IV/IO: 0.01 mg/kg.
- Atropine IV/IO: 0.02 mg/kg (for ↑ vagal tone).
-
Tachycardia: Differentiate by QRS duration.
- Key Doses:
- Adenosine (SVT): 0.1 mg/kg (1st dose), then 0.2 mg/kg.
- Synchronized Cardioversion: 0.5-1 J/kg, then 2 J/kg.
⭐ The most common cause of pediatric bradycardia is hypoxia. Unlike adults, it is rarely a primary cardiac event.

Pulseless Arrest - Code Blue, Tiny Human

- CPR: High-quality compressions (100-120/min, depth ⅓ AP diameter) & ventilation.
- Shock (VF/pVT): Start at $2$ J/kg, may escalate up to $10$ J/kg.
- Epinephrine: $0.01$ mg/kg IV/IO (0.1 mL/kg of 1:10,000) q 3-5 min.
- Amiodarone: $5$ mg/kg bolus for refractory VF/pVT.
- Reversible Causes: Address H’s & T’s (Hypoxia, Hypovolemia, etc.).
⭐ In children, pulseless arrest is most commonly caused by respiratory failure or shock (asphyxial arrest). Asystole/PEA are the most frequent initial rhythms.
PALS Pharmacology - The Potion Cabinet
- Epinephrine (Adrenaline): 0.01 mg/kg IV/IO for cardiac arrest. For bradycardia, anaphylaxis.
- Amiodarone: 5 mg/kg IV/IO bolus for shock-refractory VF/pVT.
- Lidocaine: 1 mg/kg IV/IO as an alternative to amiodarone.
- Adenosine: 0.1 mg/kg rapid IV push (1st dose); 0.2 mg/kg (2nd dose) for SVT.
- Glucose: 0.5-1 g/kg IV for hypoglycemia (use D10W/D25W).
⭐ For endotracheal administration, the epinephrine dose is much higher: 0.1 mg/kg (using the 1:1000 concentration).
Post-ROSC Care - After the Storm
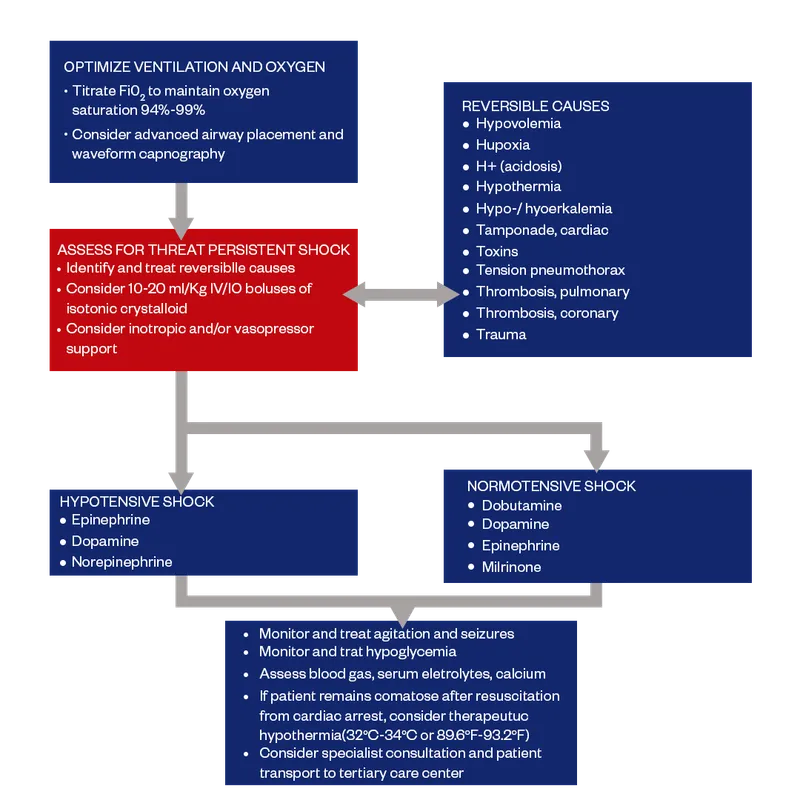
- Optimize Ventilation/Oxygenation: Maintain SpO₂ 94-99%; avoid hyperoxia. Target normocapnia (ETCO₂ 35-45 mmHg).
- Hemodynamic Support: Maintain systolic BP >5th percentile for age. Give crystalloid boluses (10-20 mL/kg); start vasopressors (epinephrine/norepinephrine) if needed.
- Neurological Care: Treat seizures promptly. Initiate Targeted Temperature Management (TTM) for comatose patients (32-36°C for 24 hrs).
- Monitoring: Continuous ECG, BP, SpO₂, ETCO₂, temperature. Monitor and correct glucose and electrolyte abnormalities.
⭐ Actively prevent and treat fever (>37.5°C) in all post-arrest patients, as hyperthermia is linked to worse neurological outcomes.
High-Yield Points - ⚡ Biggest Takeaways
- PALS prioritizes the C-A-B (Compressions-Airway-Breathing) sequence.
- Deliver high-quality chest compressions at 100-120/min to a depth of at least ⅓ the AP diameter of the chest.
- The compression-to-ventilation ratio is 30:2 for a single rescuer and 15:2 for two rescuers.
- For shockable rhythms (VF/pVT), the initial defibrillation dose is 2-4 J/kg; subsequent doses can be increased up to 10 J/kg.
- The standard Epinephrine dose (IV/IO) is 0.01 mg/kg.
- Consider Amiodarone or Lidocaine for refractory VF/pVT.
- Always identify and treat the reversible causes (the H’s and T’s).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

