Osteomyelitis - Bone Under Siege
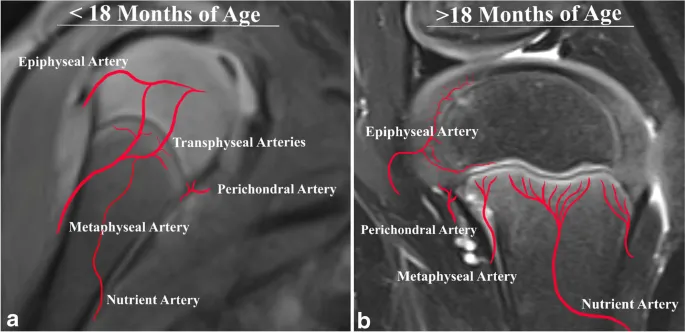
- Pathogenesis: Primarily hematogenous spread to the metaphysis of long bones (e.g., femur, tibia) due to rich, slow-flowing sinusoidal veins.
- Etiology:
- Most common: Staphylococcus aureus.
- Neonates: Group B Streptococcus, E. coli.
- Sickle Cell Disease: Salmonella spp., S. aureus.
- Diagnosis:
- Labs: ↑ ESR & CRP are early indicators.
- Imaging: X-ray findings (periosteal reaction, lytic lesions) appear late (after 10-14 days). MRI is the investigation of choice for early diagnosis.
- Gold Standard: Bone biopsy and culture.
⭐ In neonates, infection often spreads to the epiphysis and joint space, causing concomitant septic arthritis, due to transphyseal blood vessels.
- Management: Prolonged IV antibiotics (typically 4-6 weeks). Surgical drainage is required for abscesses or sequestra (necrotic bone).
Septic Arthritis - Joint Jeopardy
-
Etiology: S. aureus is the most common cause overall.
- Neonates: GBS, S. aureus, Gram-negatives.
- Children <5 yrs: S. aureus, S. pyogenes.
- Adolescents: Consider N. gonorrhoeae.
-
Clinical: Acute fever, severe monoarticular pain (hip/knee), pseudoparalysis, and refusal to bear weight.
-
Diagnosis (Kocher's Criteria for Hip):
- Fever > 38.5°C
- Inability to bear weight
- ESR > 40 mm/hr
- WBC > 12,000/mm³
- ≥3 criteria → 93% probability.
⭐ Gold Standard: Joint aspiration showing purulent fluid (WBC > 50,000/mm³, >75% neutrophils), low glucose, and positive culture.
- Treatment: Urgent surgical drainage (arthrotomy/arthroscopy) + IV antibiotics.
Diagnosis - Infection Detectives
-
Lab Markers:
- ↑ ESR > 40 mm/hr
- ↑ CRP > 20 mg/L
- ↑ TLC (Leukocytosis)
- Blood Culture: Positive in only ~50% cases.
-
Imaging:
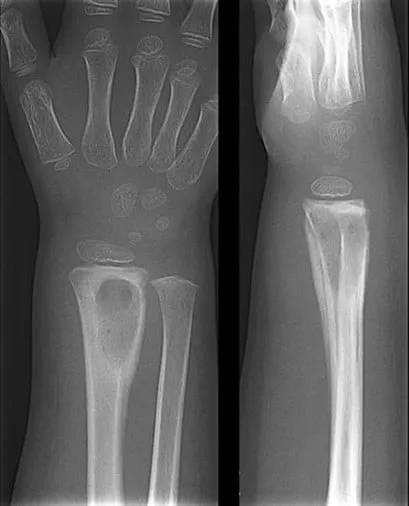
- X-ray: May be normal for 7-10 days. Late signs: lytic lesions, periosteal reaction.
- Ultrasound: Detects joint effusion.
- MRI: Most sensitive for early diagnosis of osteomyelitis.
-
Gold Standard: Aspiration of pus from bone/joint for culture.
💡 Kocher Criteria for Septic Arthritis
⭐ With all 4 Kocher criteria positive, the probability of septic arthritis is 99%. With 3 positive, it's 93%.
Management - Antibiotic Arsenal
- Empirical Therapy: Guided by age and likely pathogens.
- Duration:
- Acute Osteomyelitis: 4-6 weeks (minimum 2 weeks IV).
- Septic Arthritis: 2-3 weeks.
- Special Scenarios:
- Sickle Cell Disease: Add 3rd Gen Cephalosporin (e.g., Ceftriaxone) to cover Salmonella.
- Puncture Wound (foot): Cover Pseudomonas.
⭐ In children < 4 years, Kingella kingae is a common cause of septic arthritis. It is often gram-stain negative and requires nucleic acid amplification tests (NAAT) for diagnosis.
- S. aureus is the most common cause of acute osteomyelitis and septic arthritis in children.
- In neonates, consider Group B Strep and E. coli.
- Salmonella is the classic cause of osteomyelitis in sickle cell disease.
- Kingella kingae is a key pathogen for septic arthritis in children <4 years old.
- MRI is the most sensitive imaging modality for detecting early osteomyelitis.
- Pott's spine (TB) most commonly affects the thoracic spine.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

