AMR Fundamentals - Superbugs 101
- Antimicrobial Resistance (AMR): Microbe's ability to survive standard antimicrobial exposure.
- Mechanisms:
- Intrinsic: Natural insensitivity (e.g., Mycoplasma lacks a cell wall, making it resistant to beta-lactams).
- Acquired: Genetic mutation or Horizontal Gene Transfer (HGT).
- HGT Methods: Plasmids (conjugation), bacteriophages (transduction), naked DNA uptake (transformation).
- Key Resistance Pathways:
- Enzymatic Degradation: Beta-lactamases hydrolyzing penicillins.
- Target Site Alteration: mecA gene in MRSA alters Penicillin-Binding Proteins (PBPs).
- Efflux Pumps: Actively transport antibiotics out of the cell.
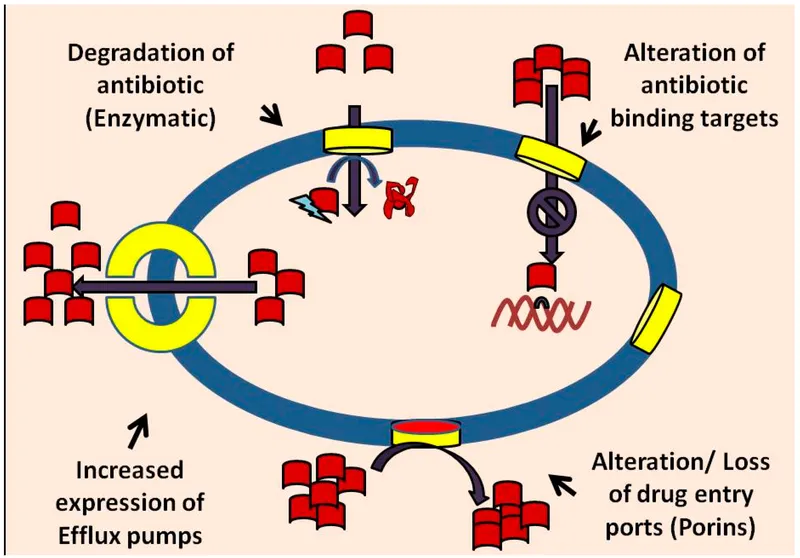
⭐ High-Yield: Plasmid-mediated conjugation is the most common mechanism for transferring resistance genes between bacteria, crucial for the spread of ESBL and carbapenemase resistance.
Resistant Pathogens in India - The Usual Suspects
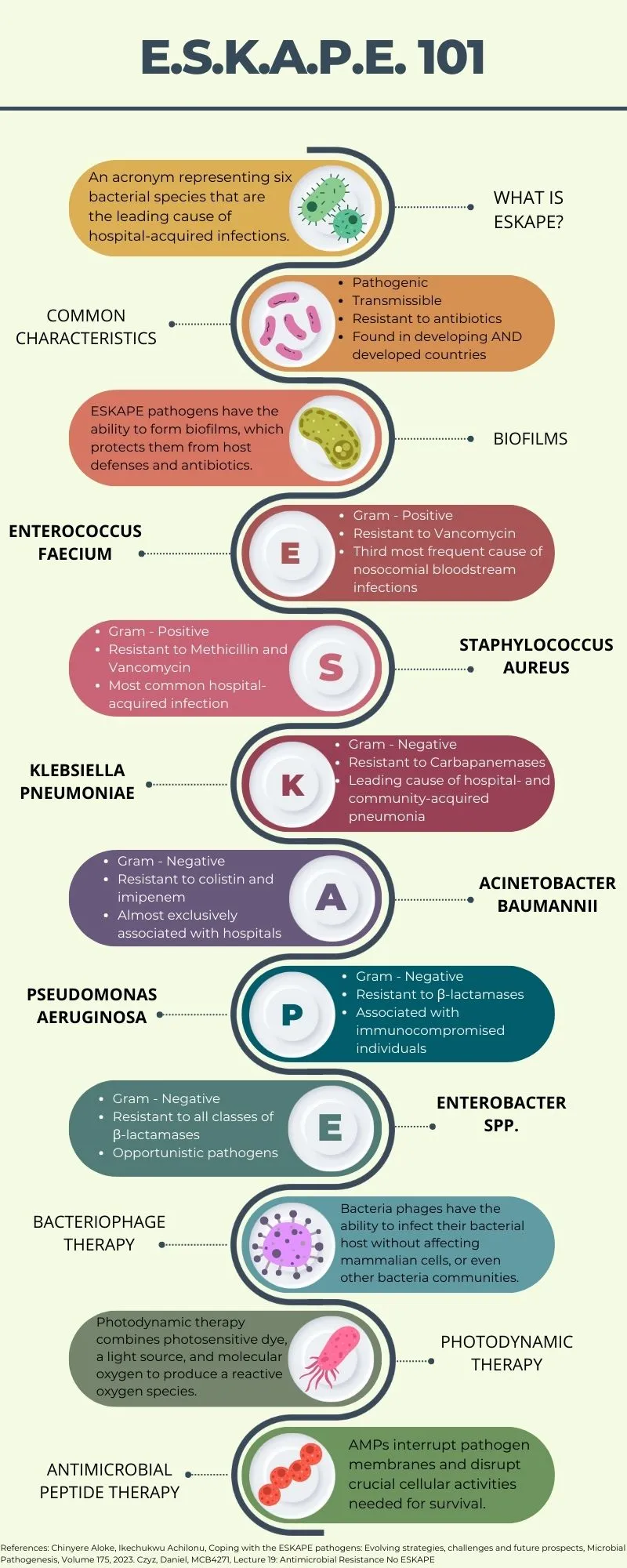
- Focus on "ESKAPE" pathogens, notorious for multidrug resistance (MDR).
- 📌 ESKAPE: Enterococcus, Staph. aureus, Klebsiella, Acinetobacter, Pseudomonas, Enterobacter.
- S. aureus: High prevalence of Methicillin-resistance (MRSA). Vancomycin resistance (VRSA) emerging.
- S. pneumoniae: Penicillin and macrolide resistance is widespread.
- Enterobacteriaceae (Klebsiella, E. coli): Extended-Spectrum β-Lactamase (ESBL) production is common. Carbapenem-Resistant Enterobacteriaceae (CRE) is a major threat.
- P. aeruginosa & A. baumannii: Frequently multidrug-resistant (MDR), especially carbapenem-resistant strains in ICUs.
- Enterococcus faecium: Vancomycin-resistant Enterococcus (VRE) is a significant nosocomial pathogen.
⭐ The New Delhi metallo-beta-lactamase (NDM-1) gene, first identified in India, drives widespread carbapenem resistance in Gram-negative bacteria like E. coli and Klebsiella.
AMR in Clinical Syndromes - When Bugs Fight Back
- Neonatal Sepsis: High resistance in Klebsiella, Acinetobacter.
- Empiric therapy failure is common.
- Carbapenems (Meropenem, Imipenem) often required.
- Colistin as a last resort for pan-drug resistance (PDR).
- Community-Acquired Pneumonia (CAP): Penicillin-resistant S. pneumoniae (PRSP).
- Resistance via altered Penicillin-Binding Proteins (PBPs).
- Higher doses of Amoxicillin (90 mg/kg/day) can overcome resistance.
- Ceftriaxone/Cefotaxime for non-responders.
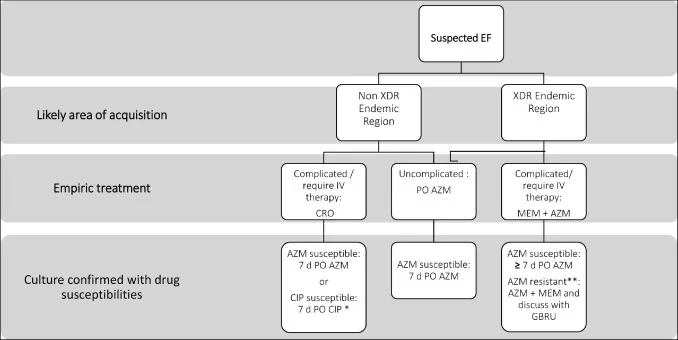
- Enteric Fever (Typhoid): Multidrug-resistant (MDR) and extensively drug-resistant (XDR) Salmonella Typhi is rampant.
- MDR: Resistant to Ampicillin, Chloramphenicol, Co-trimoxazole.
- XDR: MDR + Fluoroquinolone + 3rd Gen Cephalosporin resistance.
⭐ Azithromycin is the preferred oral agent for uncomplicated MDR Typhoid fever. For XDR Typhoid, Meropenem is often the treatment of choice, sometimes combined with Azithromycin.
Antimicrobial Stewardship - The Good Fight
- Goal: Optimize clinical outcomes while minimizing unintended consequences of antimicrobial use, primarily resistance.
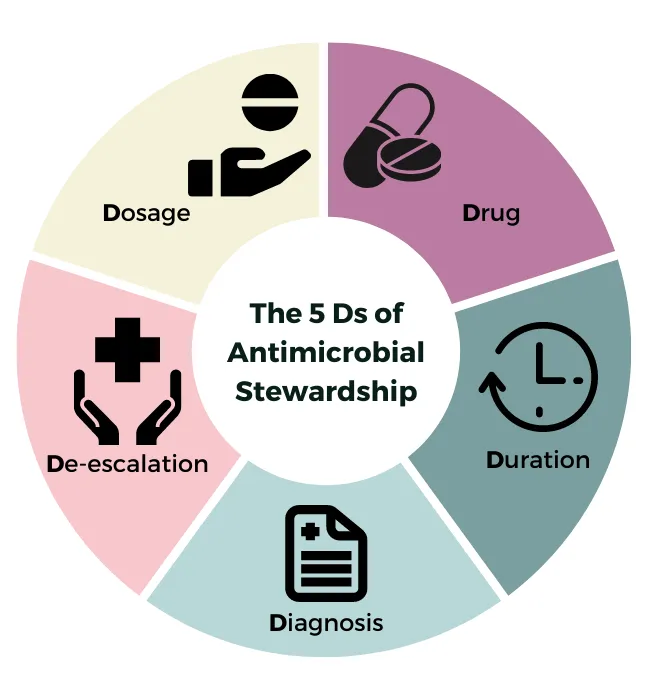
- The 5 Ds of AMS:
- Diagnosis: Accurate and timely.
- Drug: Correct choice, narrowest spectrum.
- Dose: Optimized based on weight and renal function.
- Duration: Shortest effective duration.
- De-escalation: Switch to targeted therapy post-sensitivity results.
⭐ WHO AWaRe Classification: A key stewardship tool categorizing antibiotics into Access, Watch, and Reserve groups to combat resistance.
High‑Yield Points - ⚡ Biggest Takeaways
- Inappropriate antibiotic use, especially for viral infections, is the primary driver of resistance.
- Key resistant pathogens include MRSA, ESBL-producers (E. coli, Klebsiella), and Penicillin-Resistant S. pneumoniae (PRSP).
- For Enteric Fever, widespread fluoroquinolone resistance necessitates using azithromycin or ceftriaxone.
- MDR-TB in children is a growing threat requiring specialized drug regimens and contact tracing.
- Management hinges on antibiotic stewardship and strict adherence to culture sensitivity data.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

