Pathophysiology - The Growth Thief
- Nutritional Deficit: The core issue. Results from ↓intake (anorexia), malabsorption, or ↑metabolic demand, diverting calories from growth.
- Inflammatory Cytokine Storm:
- Key mediators: TNF-α, IL-1, IL-6.
- Effects: Induce anorexia, ↑catabolism, and cause Growth Hormone (GH) resistance.
- Hormonal Dysregulation:
- GH-IGF-1 Axis Disruption: ↓IGF-1 (the "workhorse" of growth) despite normal/↑GH.
- Glucocorticoid Excess: Directly inhibits cartilage growth in the epiphyseal plate.
- Hypogonadism: Delays pubertal growth spurt.
- Direct Tissue Insults:
- Chronic acidosis (e.g., RTA) and hypoxia (e.g., cyanotic heart disease) impair cellular growth processes.
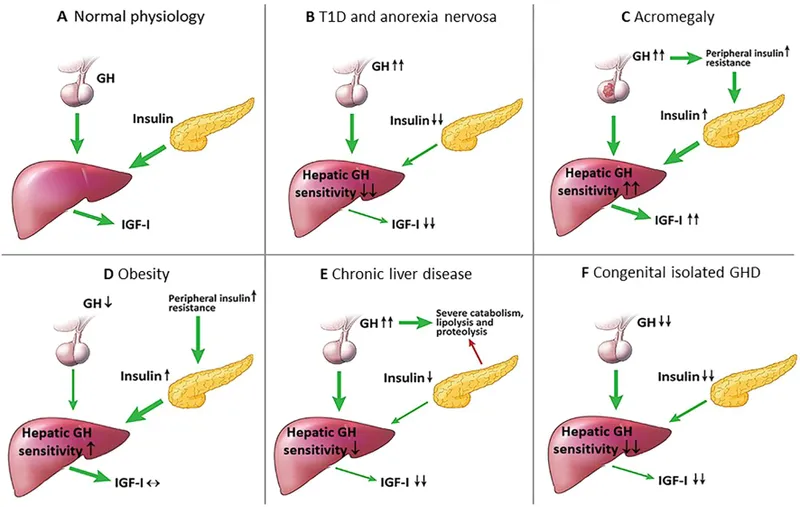
⭐ The key hormonal finding in growth failure of chronic disease is GH resistance: characterized by normal or ↑GH levels with paradoxically ↓IGF-1 levels.
System-Specific Impacts - Disease Deep Dive
- Congenital Heart Disease (CHD):
- Cyanotic CHD > Acyanotic CHD for growth impact.
- Mechanisms: Chronic hypoxia, increased caloric needs, feeding difficulties.
- Chronic Kidney Disease (CKD):
- Key factors: Metabolic acidosis, renal osteodystrophy, anemia, and growth hormone (GH) resistance.
- Uremic toxins disrupt the GH-IGF-1 axis.
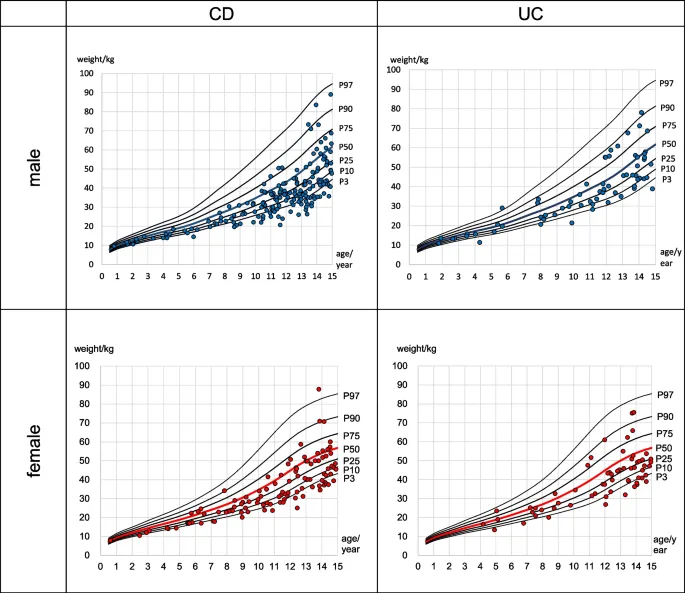
- Gastrointestinal (IBD - Crohn's):
- Mechanisms: Malabsorption, systemic inflammation (↑ TNF-α, IL-6), and poor appetite.
- Weight is affected more than height initially.
⭐ In Crohn's disease, growth failure can be the sole presenting feature, preceding GI symptoms by years.
Assessment - Growth Detective Work
- History is Key: Detailed 3-day dietary recall, systemic symptoms (fever, diarrhea, pain), birth history, and developmental milestones.
- Clinical Clues:
- Weight-for-height (Wasting): Indicates acute malnutrition.
- Height-for-age (Stunting): Indicates chronic malnutrition.
- Look for specific signs: pallor, edema, clubbing, organomegaly.
- Core Investigations:
- Bone Age X-ray (left hand & wrist): Crucial; often delayed more than chronological age.
- Screening Labs: CBC, ESR, CRP, Urinalysis, Stool exam, LFT, KFT.
⭐ In nutritional growth failure, the sequence of impact is always: Weight → Height → Head Circumference.
Management - The Growth Boosters
-
Nutritional Rehabilitation: Cornerstone of management.
- High-calorie diets: ↑ intake by 25-50% over RDA.
- Enteral feeds (NG/gastrostomy) if oral intake is inadequate.
- Micronutrient supplementation (Iron, Zinc, Vit D).
-
Disease-Specific Therapy: Treat the underlying condition aggressively.
- e.g., Anti-TNF agents in Crohn's disease, gluten-free diet in Celiac disease.
-
Hormonal Therapy: For persistent growth failure despite other measures.
- Recombinant Human Growth Hormone (rhGH).
- Indications: Chronic Renal Insufficiency (CRI), Turner Syndrome, SGA.
- Dose for CRI: 0.045-0.050 mg/kg/day.
⭐ In Chronic Renal Insufficiency, rhGH therapy is approved for pre-dialysis patients to promote catch-up growth before transplantation.
High‑Yield Points - ⚡ Biggest Takeaways
- Chronic disease first impacts weight, then height, and lastly head circumference.
- The most common mechanism is inadequate caloric intake due to anorexia or malabsorption.
- Catch-up growth is a key feature and occurs once the underlying disease is controlled.
- Bone age is a more reliable indicator of growth potential than chronological age and is usually delayed.
- Growth failure is most severe during infancy and puberty.
- Consider endocrinopathies (hypothyroidism) and renal disease as non-nutritional causes.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

