FTT Definition - Sizing Up The Problem
- Definition: FTT is inadequate weight gain. Key indicators:
- Weight-for-age < 3rd or 5th percentile.
- Weight-for-length/height < 3rd or 5th percentile.
- Weight drop crossing two major centile lines (e.g., 90th → 50th).
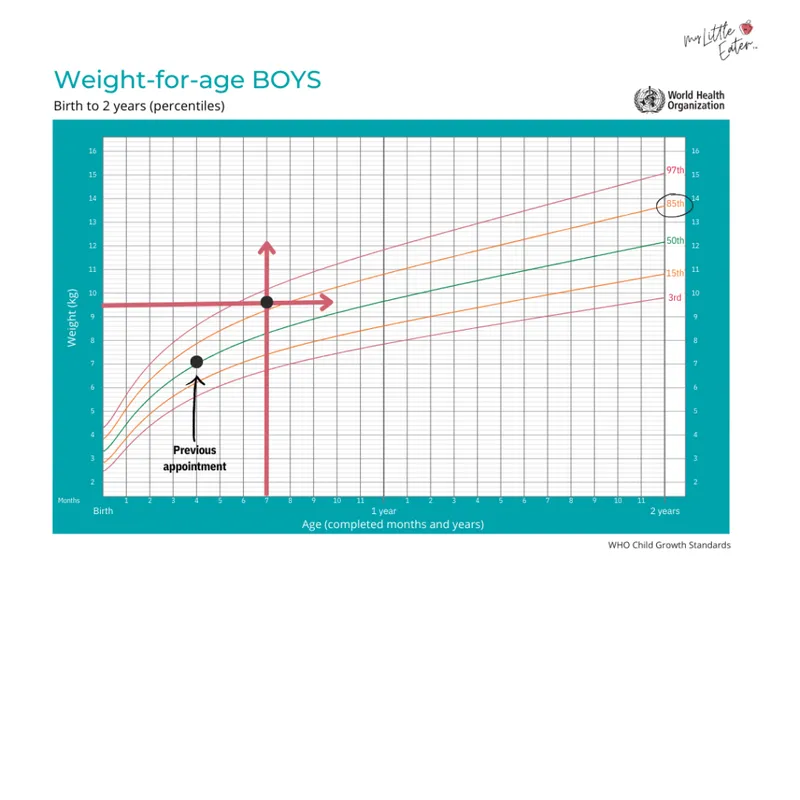
- Growth Charts:
- Use WHO charts for children < 2 years.
- Use IAP (Indian Academy of Pediatrics) charts for > 2 years.
⭐ Most FTT is non-organic, often due to inadequate caloric intake or psychosocial factors, rather than an underlying medical condition.
FTT Etiology - The 'Why' Behind It
- Primary Division: FTT is broadly classified into Organic (underlying medical condition) and Non-Organic (psychosocial) causes, often with significant overlap.
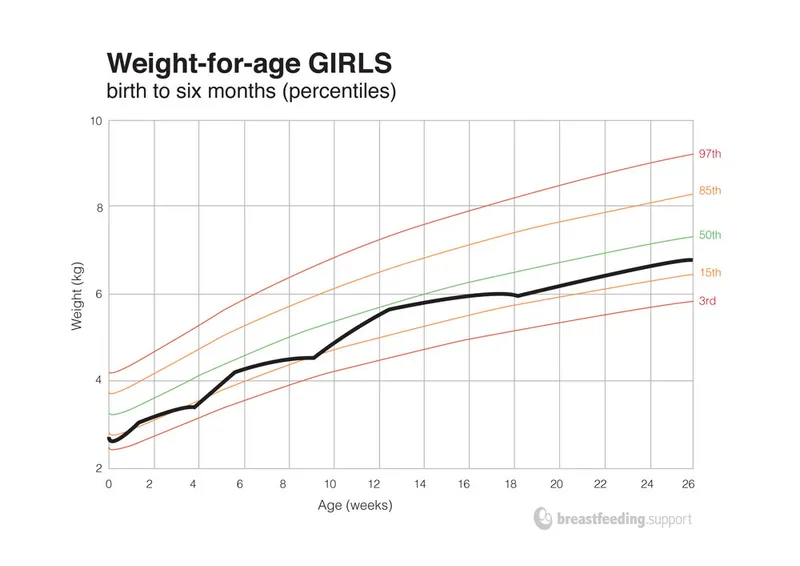
⭐ The most common cause of FTT is non-organic/psychosocial, accounting for over 75% of cases. It's often a diagnosis of exclusion after ruling out organic pathology.
Evaluation Pathway - The FTT Workup
- Initial Steps: Thorough history (including 72-hr diet recall), observed feeding, and meticulous growth chart plotting are paramount.
- Screening Labs (Tier 1): If no cause is evident after initial assessment and dietary counseling:
- Complete Blood Count (CBC)
- Urinalysis & culture
- Basic Metabolic Panel (BMP)
- Stool for occult blood, pH, reducing substances
⭐ In >85% of cases, a cause for FTT is found through a detailed history and physical exam alone, making extensive, unfocused lab testing low-yield.
Management Strategy - The Recovery Plan
- Nutritional Rehabilitation: The cornerstone of management.
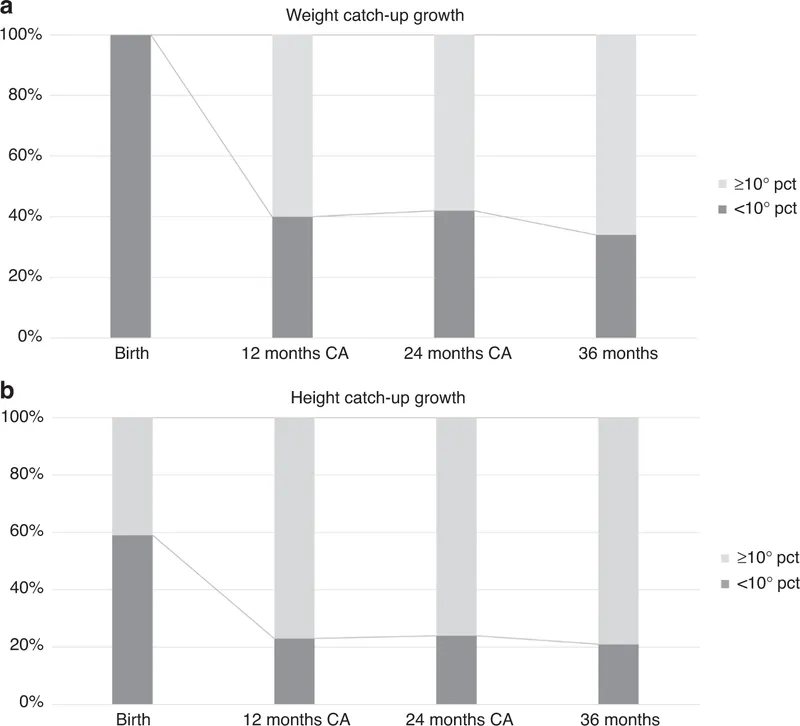
- Goal: Achieve catch-up growth with high-calorie diet (1.5-2x RDA).
- Caloric Requirement Calculation:
- $Required,Kcal/kg = \frac{Ideal,weight,for,height \times 120}{Actual,weight}$
- Use high-density feeds (e.g., 1 kcal/mL).
- Multidisciplinary Team: Involve pediatrician, dietitian, social worker, and psychologist for comprehensive care.
- Monitoring:
- Initial daily weight checks.
- Weekly length and head circumference measurements.
⭐ High-Yield: Expect a weight gain of >20-30 g/day in a hospitalized child during initial recovery.
High‑Yield Points - ⚡ Biggest Takeaways
- Most common cause of FTT is non-organic (e.g., psychosocial deprivation).
- Weight is the first parameter to fall, followed by height, and lastly head circumference.
- Wasting (↓ weight-for-height) indicates acute malnutrition; Stunting (↓ height-for-age) suggests chronic malnutrition.
- A detailed dietary history and observation of feeding are the most crucial diagnostic tools.
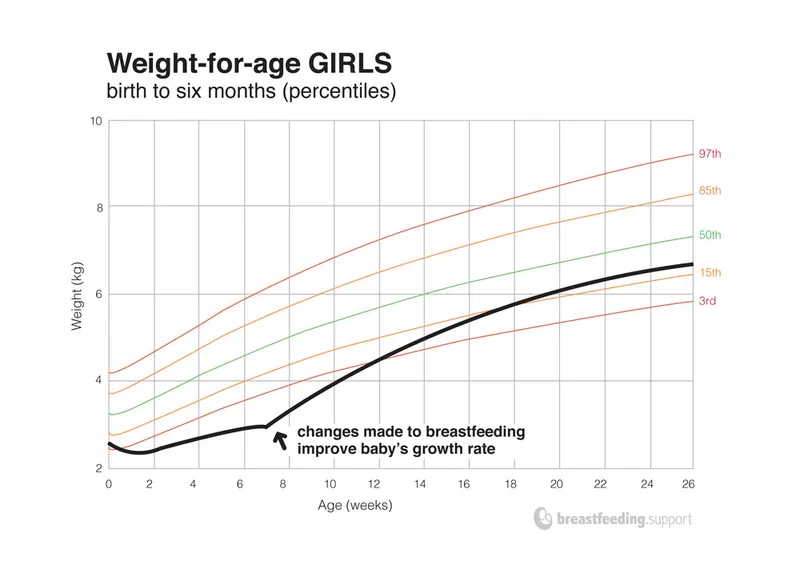
- Hospitalization showing catch-up growth strongly suggests a non-organic cause.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

