Definition & Thresholds - The Late Bloomers
Delayed puberty is the absence of initial signs of sexual maturation at an age that is 2-2.5 standard deviations above the population mean.
- Girls: No thelarche (breast development, Tanner stage 2) by age 13.
- Boys: No testicular enlargement (≥4 mL volume or ≥2.5 cm length) by age 14.
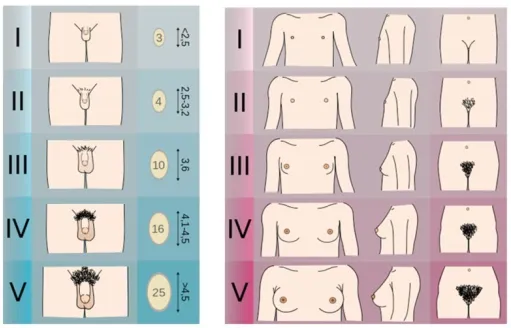
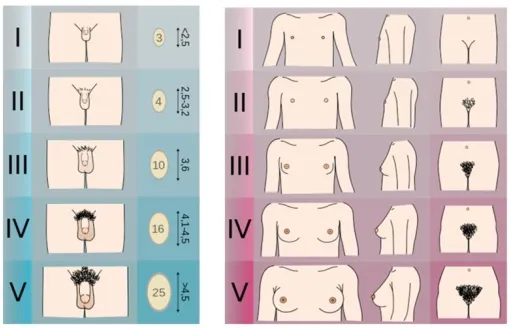
Assessment relies on Tanner staging to classify physical development.
⭐ Constitutional Delay of Growth and Puberty (CDGP) is the most common cause, representing a normal variant of development.
Etiology - Central vs. Peripheral
Delayed puberty results from low sex steroids. The primary defect can be central (hypothalamus/pituitary) or peripheral (gonadal failure).
| Hypogonadotropic Hypogonadism (Central) | Hypergonadotropic Hypogonadism (Peripheral) |
|---|---|
| Defect in GnRH/FSH/LH secretion | Primary gonadal failure |
| ↓ FSH/LH → ↓ Estrogen/Testosterone | ↑ FSH/LH → ↓ Estrogen/Testosterone |
| - Constitutional Delay: Most common overall. | - Turner Syndrome: (45,XO); webbed neck, shield chest. |
| - Kallmann Syndrome: Defective GnRH neuron migration; associated with anosmia. | - Klinefelter Syndrome: (47,XXY); gynecomastia, tall stature. |
| - CNS Tumors: e.g., Craniopharyngioma. | - Gonadal Damage: Chemotherapy, radiation. |
| - Chronic Illness/Malnutrition. |
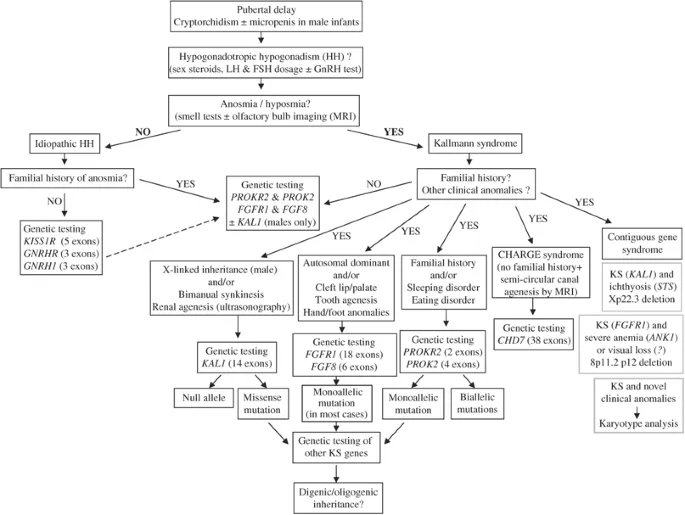
Clinical Approach - The Puberty Detective
Initial workup is key. A systematic approach differentiates central from peripheral causes.
-
Step 1: Foundation
- Detailed History: Inquire about chronic illness, nutrition, and anosmia (smell deficit).
- Physical Exam: Tanner staging, height/weight percentiles, dysmorphic features.
- Bone Age X-ray (non-dominant wrist): Crucial first step. Is bone age delayed compared to chronological age?
-
Step 2: Hormonal Axis
- Measure basal FSH & LH levels.
⭐ In a patient with delayed puberty and anosmia or hyposmia, always suspect Kallmann Syndrome, a form of central hypogonadotropic hypogonadism due to failed GnRH neuron migration.
Management - Kickstarting the Clock
-
Constitutional Delay (CDGP):
- Mainstay: Reassurance and observation.
- For psychosocial distress: Short course (4-6 months) of low-dose sex steroids.
- Boys: Testosterone IM (50-100 mg/month) or oral.
- Girls: Ethinyl estradiol (2.5-5 mcg/day).
-
Gonadal Failure (Hypergonadotropic):
- Hormone Replacement Therapy (HRT) to induce and maintain secondary sexual characteristics.
- Girls (Turner’s): Estrogen therapy; progesterone is added later to induce withdrawal bleeding.
- Boys (Klinefelter’s): Testosterone replacement.
-
Central Causes (Hypogonadotropic):
- Address the underlying pathology (e.g., tumor).
- Fertility induction: Pulsatile GnRH or gonadotropins (hCG, hMG).
⭐ In Turner Syndrome, estrogen is initiated at a low dose around age 11-12 to mimic natural puberty, maximizing adult height potential by delaying epiphyseal fusion.
High‑Yield Points - ⚡ Biggest Takeaways
- Delayed puberty is the absence of secondary sexual characteristics by age 13 in girls or 14 in boys.
- The most common cause is Constitutional Delay of Growth and Puberty (CDGP), a diagnosis of exclusion.
- The first investigation is a bone age X-ray, which is characteristically delayed in CDGP.
- Hypogonadotropic hypogonadism (↓FSH/LH) suggests a central cause like Kallmann syndrome (often with anosmia).
- Hypergonadotropic hypogonadism (↑FSH/LH) indicates primary gonadal failure (e.g., Turner or Klinefelter syndrome).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

