Skeletal Dysplasias: Overview - Blueprint for Bones
- Heterogeneous group of disorders causing abnormal bone & cartilage growth, leading to disproportionate short stature.
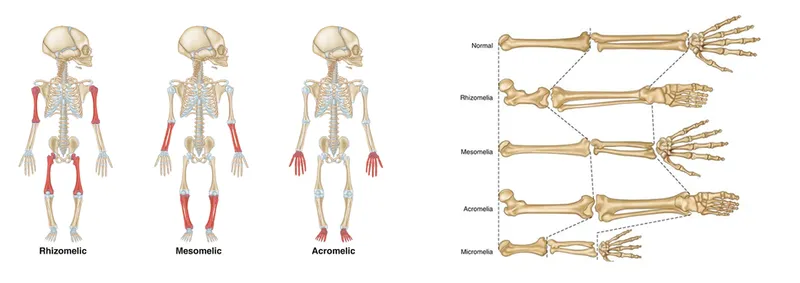
- Classified by affected limb segment:
- Rhizomelic: Proximal (humerus, femur)
- Mesomelic: Middle (radius/ulna, tibia/fibula)
- Acromelic: Distal (hands, feet)
- Micromelic: Entire limb is shortened
- Key genetic culprits: Collagen (COL1A1) & FGFR3 gene mutations.
⭐ Thanatophoric dysplasia, the most common lethal skeletal dysplasia, is linked to FGFR3 gene mutations.
Achondroplasia - The King of Dwarfs
- Genetics & Patho: Most common non-lethal skeletal dysplasia. Autosomal Dominant, but >80% of cases are de novo mutations (advanced paternal age is a risk factor).
- Cause: Gain-of-function mutation in the FGFR3 gene on chromosome 4p16.3.
- Effect: Inhibits chondrocyte proliferation in epiphyseal growth plates, impairing endochondral ossification.
- Clinical Features:
- Limbs: Rhizomelic (proximal) shortening. Genu varum (bow-legs). Trident hand (persistent space between 3rd & 4th digits).
- Craniofacial: Macrocephaly with frontal bossing & midface hypoplasia.
- Spine: Thoracolumbar kyphosis, exaggerated lumbar lordosis.
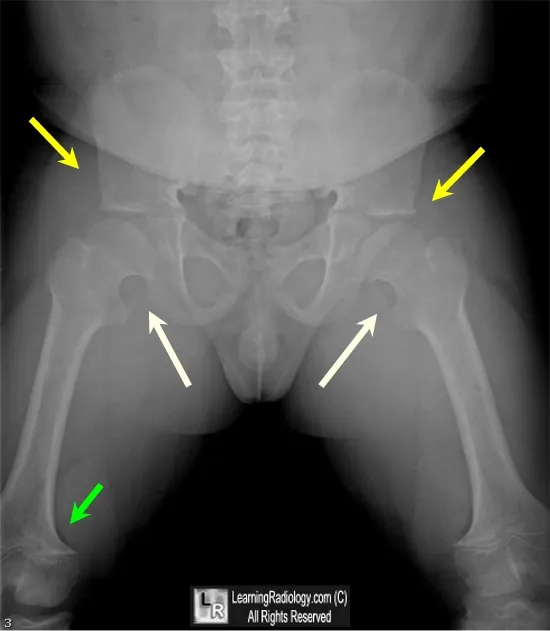
- Radiology:
- Spine: Caudal narrowing of interpedicular distance.
- Pelvis: "Champagne-glass" pelvic inlet.
⭐ Foramen magnum stenosis is the most serious complication in infancy, potentially causing hydrocephalus, sleep apnea, or sudden infant death.
Osteogenesis Imperfecta - Brittle Bone Blues
- Patho: Autosomal Dominant defect in Type I collagen (COL1A1/A2 genes).
- Classic Triad:
- Multiple recurrent fractures with minimal trauma.
- Blue sclerae.
- Hearing loss (conductive/mixed).
- Other signs: Dentinogenesis imperfecta (opalescent teeth), joint hypermobility, short stature.
- 📌 Mnemonic (BITE): Bones (fractures), I (Eyes - blue sclera), Teeth (dentinogenesis imperfecta), Ear (hearing loss).
- Types (Sillence):
- Type I: Mildest, most common.
- Type II: Lethal perinatal.
- Type III: Progressive deforming.
- Rx: Bisphosphonates (Pamidronate), physiotherapy.
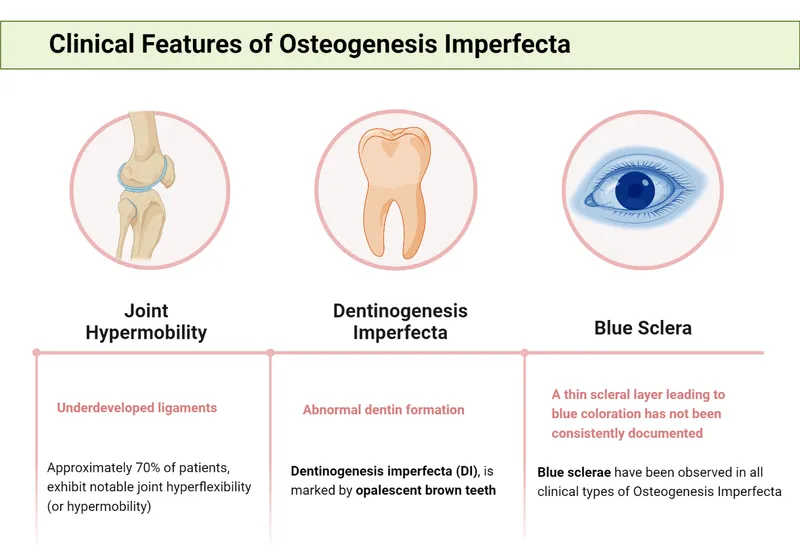
⭐ Exam Pearl: The characteristic blue sclera is due to the translucency of the thin scleral collagen, revealing the color of the underlying choroidal veins.
Other Key Dysplasias - Rogues' Gallery of Bones
-
Cleidocranial Dysostosis
- Gene: RUNX2 (AD)
- Features: Aplastic/hypoplastic clavicles (patient can appose shoulders), delayed fontanelle closure, wormian bones, supernumerary teeth.
- 📌 Mnemonic: CCD → Clavicles, Cranium, Dentition.
-
Diastrophic Dysplasia
- Gene: SLC26A2 (AR)
- Features: "Hitchhiker thumb" (abducted thumb), cauliflower ear, severe clubfoot, kyphoscoliosis.
-
Spondyloepiphyseal Dysplasia (SED)
- Gene: COL2A1 (Type II Collagen)
- Features: Affects spine & epiphyses → platyspondyly (flat vertebrae), short trunk dwarfism. Often associated with myopia & retinal detachment.
⭐ Diastrophic Dysplasia is often called "hitchhiker's dysplasia" due to the characteristic abducted, retroflexible thumb, a key diagnostic clue.
High-Yield Points - ⚡ Biggest Takeaways
- Achondroplasia, the most common non-lethal dysplasia, is due to an FGFR3 gene mutation, presenting with trident hands.
- Thanatophoric dysplasia, the most common lethal form, is also an FGFR3 mutation, often showing a cloverleaf skull.
- Osteogenesis Imperfecta is a Type I collagen defect, leading to blue sclera, fractures, and hearing loss.
- Osteopetrosis (“marble bone disease”) involves defective osteoclast function, causing dense, brittle bones and pancytopenia.
- Look for hitchhiker thumb in Diastrophic Dysplasia.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

