Esophagus & Diaphragm - Upper Tract Troubles
-
Tracheoesophageal Fistula (TEF)
- Most common: Type C (85%), with esophageal atresia & distal fistula.
- Antenatal: Polyhydramnios (impaired fetal swallowing).
- Postnatal: Frothing/drooling, choking on feeds, respiratory distress.
- Diagnosis: Coiled nasogastric tube in upper esophagus on X-ray.
- 📌 VACTERL association: Vertebral, Anal, Cardiac, TEF, Renal, Limb defects.
-
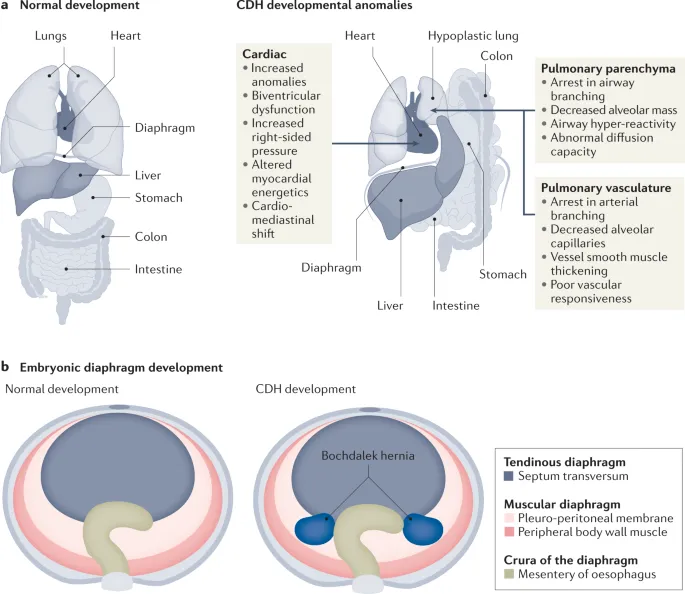
Congenital Diaphragmatic Hernia (CDH)
- Most common: Bochdalek hernia (left posterolateral).
- Signs: Severe respiratory distress at birth, scaphoid abdomen, bowel sounds in chest.
- Management: Immediate intubation; avoid bag-mask ventilation.
⭐ CDH Prognosis: The Lung-to-Head Ratio (LHR) on fetal ultrasound is the best predictor of outcome.
Gut Obstructions - The Vomiting Babies
- Presents with non-bilious or bilious vomiting, depending on obstruction level relative to the ampulla of Vater.
- Key diagnostic: Abdominal X-ray to identify characteristic gas patterns.
| Feature | Hypertrophic Pyloric Stenosis (HPS) | Duodenal Atresia | Jejunal/Ileal Atresia |
|---|---|---|---|
| Vomiting | Non-bilious, projectile (2-8 wks) | Bilious (hours post-birth) | Bilious (24-48 hrs) |
| Palpation | Olive-shaped mass in RUQ | Scaphoid abdomen | Abdominal distension |
| X-ray Sign | Single bubble (dilated stomach) | Double bubble | Triple bubble / multiple levels |
| Cause | Pylorus muscle hypertrophy | Failure to recanalize | In utero vascular accident |
⭐ Double Bubble Sign: The pathognomonic "double bubble" on an AXR for duodenal atresia is caused by gas in the stomach and the proximal duodenum. It is strongly associated with Trisomy 21.
Twists & Nerves - Gut's Wrong Turn
-
Malrotation: Abnormal intestinal rotation during fetal life, creating a narrow mesenteric base prone to twisting (volvulus).
- Presentation: Sudden onset of bilious vomiting in a neonate is the cardinal sign.
- Diagnosis: Upper GI contrast series is the gold standard, showing a "corkscrew" sign. USG may show a "whirlpool sign".
- Management: Emergency surgery (Ladd's Procedure).
-
Hirschsprung's Disease: Aganglionosis of the distal bowel due to failed neural crest cell migration.
- Presentation: Failure to pass meconium in the first 24-48 hours, abdominal distension, and bilious emesis.
- Diagnosis: Rectal suction biopsy is the definitive diagnostic test.
⭐ In Hirschsprung's disease, the transition zone is most commonly found in the recto-sigmoid segment (~80%).
Anorectal Malformations - The Final Exit
- Spectrum of hindgut termination anomalies, often part of the VACTERL association (Vertebral, Anal, Cardiac, Tracheal, Esophageal, Renal, Limb).
- Classification: High vs. Low, based on the relation of the rectal pouch to the pubococcygeal (PC) line.
- Diagnosis: Clinical exam + Invertogram (Wangesteen-Rice) to assess pouch height. A gas-to-skin distance > 2 cm indicates a high lesion.
⭐ In males, the most common fistula is rectourethral (bulbar). In females, it's rectovestibular.
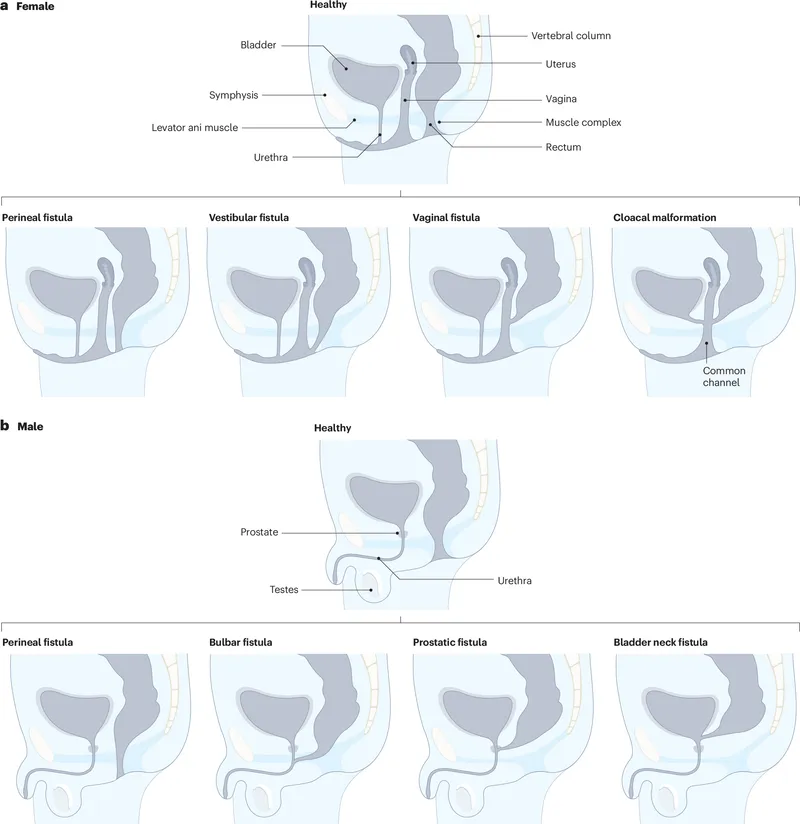
- Management: Low lesions are treated with perineal anoplasty. High lesions require a staged approach: initial colostomy, followed by Posterior Sagittal Anorectoplasty (PSARP).
High‑Yield Points - ⚡ Biggest Takeaways
- Tracheoesophageal fistula is most commonly Type C; presents with coiling of the nasogastric tube.
- Duodenal atresia shows a "double-bubble" sign on X-ray and is strongly associated with Down syndrome.
- Jejunal and ileal atresia are due to an in-utero vascular accident.
- Hypertrophic pyloric stenosis presents with non-bilious projectile vomiting and a palpable "olive-like" mass.
- Hirschsprung's disease results from failed neural crest cell migration; diagnosis is confirmed by rectal biopsy.
- Meckel's diverticulum is diagnosed using a Technetium-99m scan for ectopic gastric mucosa.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

