Leukemia Basics - Blood Cell Rebellion
- Most common childhood malignancy (~33%).
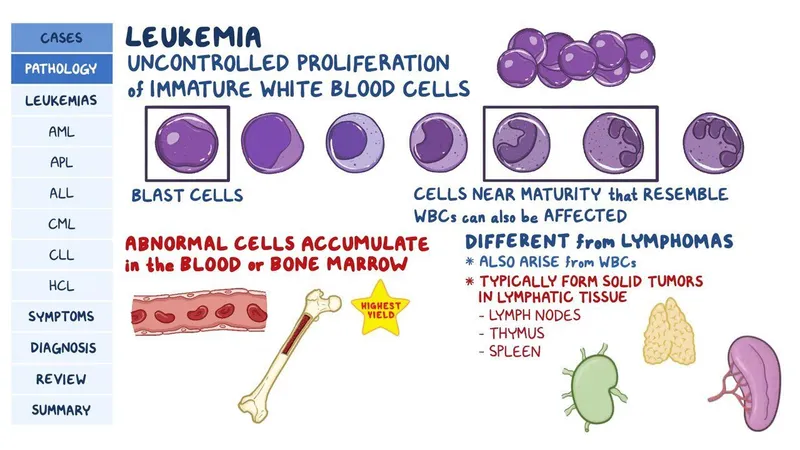
- Uncontrolled clonal proliferation of immature hematopoietic cells (blasts) in the bone marrow.
- This "rebellion" leads to bone marrow failure:
- ↓ RBCs → Anemia (pallor, fatigue)
- ↓ Platelets → Thrombocytopenia (petechiae, bleeding)
- ↓ Neutrophils → Neutropenia (recurrent infections)
- Blasts can infiltrate extramedullary sites: liver, spleen, lymph nodes (LNs), CNS, and testes.
⭐ Children with Down syndrome (Trisomy 21) have a 10-20x increased risk of developing acute leukemia, particularly ALL.
Acute Lymphoblastic Leukemia (ALL) - The Lympho-Blast Off
- Most common childhood cancer; peak incidence at 2-5 years.
- Presentation: Abrupt onset of bone marrow failure symptoms (anemia, infection, bleeding), bone pain, and lymphadenopathy.
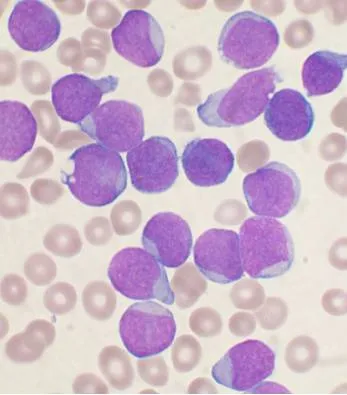
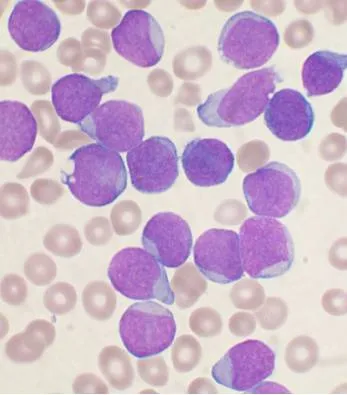
- Diagnosis: Requires >25% lymphoblasts in bone marrow.
- B-ALL (85%): CD10, CD19, CD22, TdT+. Good prognosis.
- T-ALL (15%): CD2, CD3, CD5, CD7, TdT+. Often presents with a mediastinal mass.
⭐ CNS Prophylaxis: All ALL patients receive intrathecal chemotherapy (e.g., Methotrexate) as the CNS is a pharmacological sanctuary site.
Acute Myeloid Leukemia (AML) - Myeloid Mayhem
- Accounts for 15-20% of childhood leukemias; less common than ALL.
- Key Associations: Down syndrome (especially < 4 years), Fanconi anemia, neurofibromatosis type 1.
- Clinical Hallmarks: Besides pancytopenia symptoms (fatigue, fever, bleeding), look for:
- Gingival hypertrophy (common in M4/M5 subtypes)
- Leukemia cutis (nodular skin infiltrates)
- Myeloid sarcoma (Chloroma): extramedullary solid tumor of blasts.
- Diagnosis: Bone marrow aspirate showing ≥20% myeloblasts.
- Auer rods: Pathognomonic eosinophilic, needle-like cytoplasmic inclusions.
- Cytochemistry: Blasts are Myeloperoxidase (MPO) and Sudan Black B (SBB) positive.
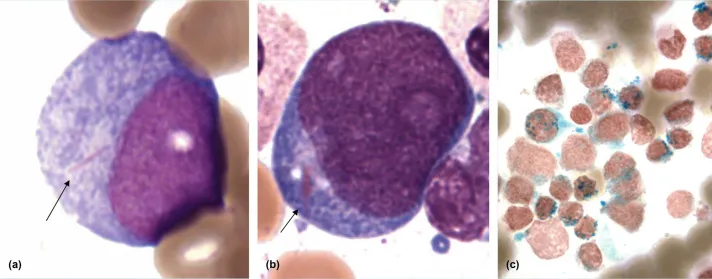
⭐ AML M7 (Acute Megakaryoblastic Leukemia) is strongly associated with Down syndrome, particularly in children < 4 years of age.
Diagnosis & Management - The Cancer Crackdown
- Initial Workup: Complete Blood Count (CBC) with Peripheral Smear (PS) showing ↑ blasts, pancytopenia.
- Confirmatory Test: Bone Marrow Aspiration & Biopsy is gold standard. Diagnosis requires >20% blasts.
- Lineage & Risk: Flow cytometry (differentiates ALL/AML), cytogenetics, and molecular studies (e.g., t(9;22) Philadelphia) for risk stratification.
- Management: Multi-agent chemotherapy is the mainstay.
- Phases (ALL): Induction → Consolidation → Interim Maintenance → Delayed Intensification → Maintenance.
- CNS Prophylaxis: Intrathecal Methotrexate is crucial to prevent CNS relapse.
- Supportive Care: Blood product transfusions, managing infections (neutropenic fever).
⭐ Auer rods (needle-like cytoplasmic inclusions) seen on peripheral smear are pathognomonic for Acute Myeloid Leukemia (AML).
- Acute Lymphoblastic Leukemia (ALL) is the most common pediatric malignancy, with a peak incidence at 2-5 years.
- Favorable prognosis in ALL is associated with hyperdiploidy and the t(12;21) translocation.
- Poor prognostic markers include age <1 year or >10 years, WBC >50,000/μL, and the t(9;22) Philadelphia chromosome.
- AML is less common and often presents with Auer rods in myeloblasts.
- CNS prophylaxis is a mandatory component of ALL treatment to prevent relapse.
- Be vigilant for Tumor Lysis Syndrome, an oncologic emergency.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

