Advance Directives - The Master Plan
- Advance Directive: A legal document outlining a patient's wishes for future medical care should they become unable to make decisions. Rooted in the Patient Self-Determination Act (1990).
- Key Types:
- Living Will: Specifies desired treatments (e.g., no mechanical ventilation) if terminally ill or in a persistent vegetative state.
- DPOA-HC (Healthcare Proxy): Designates a person to make healthcare decisions upon incapacitation.
- DNR/DNI: Specific medical orders to withhold CPR or intubation.
- POLST: Converts patient wishes into actionable medical orders for the seriously ill.
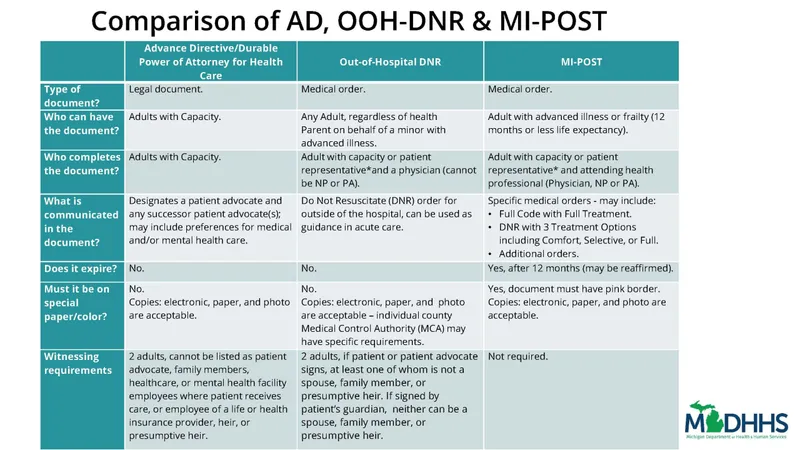
⭐ If a patient has both a living will and a healthcare proxy (DPOA-HC), the proxy's decisions generally take precedence, as they can interpret the patient's wishes in the current specific clinical context.
Will vs. Proxy - Paper Power
Advance directives are legal documents for when a patient loses decision-making capacity-a clinical determination distinct from legal competence.
| Feature | Living Will (Instructional Directive) | DPOA-HC (Proxy Directive) |
|---|---|---|
| What it is | Specifies desired or refused treatments (e.g., mechanical ventilation, tube feeding). | Appoints a surrogate decision-maker (health care proxy) to act for the patient. |
| Activation | Upon loss of capacity AND presence of a qualifying condition (e.g., terminal illness). | Activates simply when the patient loses decision-making capacity. |
| Flexibility | Inflexible; only applies to situations explicitly written and can be difficult to interpret. | Highly flexible; the proxy can interpret the patient's wishes for unforeseen circumstances. |
⭐ In the absence of an advance directive, states provide a legal hierarchy for the next of kin to act as a surrogate, typically: spouse → adult children → parents.
Medical Orders - The Action Plan
-
Code Status Orders: Specific medical directives for immediate, life-sustaining interventions.
- DNR (Do Not Resuscitate): Prohibits cardiopulmonary resuscitation (CPR) if a patient's heart or breathing stops.
- DNI (Do Not Intubate): Prohibits the insertion of an endotracheal tube.
-
POLST (Physician Orders for Life-Sustaining Treatment): A portable medical order for patients who are seriously ill or frail. It translates a patient's end-of-life wishes into actionable medical commands.
- Portability: Valid and honored across different healthcare settings (e.g., home, nursing facility, hospital).
- Actionable: Unlike a traditional advance directive, a POLST is a direct medical order.
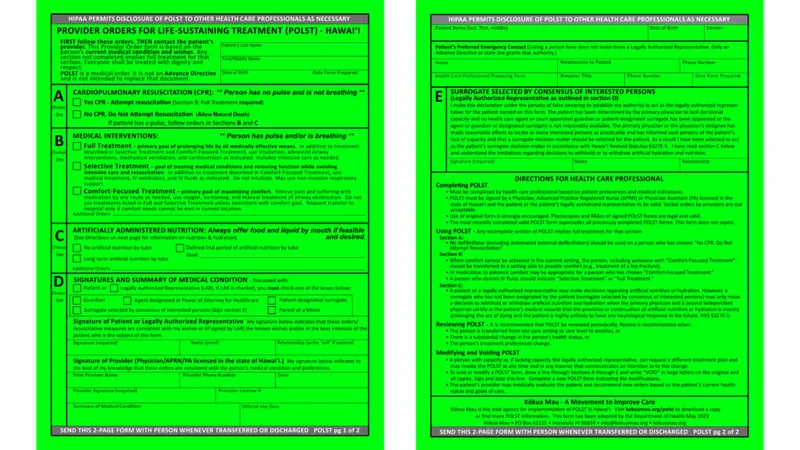

⭐ A POLST is for current treatment plans for seriously ill patients, whereas a living will is for future, hypothetical scenarios and is not a medical order.
Capacity & Surrogates - Who Decides?
-
Decision-Making Capacity: A clinical determination required for informed consent. It is task-specific and can fluctuate. Assessed using:
- 📌 Mnemonic: CURVES
- Communicate a choice
- Understand relevant information
- Reason about treatment options
- Value the consequences
- Emergency (not) - capacity is assumed unless challenged.
- 📌 Mnemonic: CURVES
-
Surrogate Hierarchy: If no DPOA-HC is designated, the following are approached in order:
-
- Spouse
-
- Adult Child (majority consensus)
-
- Parent
-
- Adult Sibling
-
⭐ High-Yield: Capacity is a clinical finding assessed by a physician, while competence is a legal state determined by a judge. A patient can lack capacity for one decision without being legally incompetent overall.
High‑Yield Points - ⚡ Biggest Takeaways
- Advance directives are legal documents guiding future medical care if a patient loses decision-making capacity.
- A living will outlines specific treatment preferences, while a healthcare proxy (or durable power of attorney) designates a surrogate decision-maker.
- Directives must be created when the patient is competent.
- A competent patient can revoke or change a directive at any time.
- The Patient Self-Determination Act requires institutions to inquire about and uphold advance directives.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

