Soft Tissue Tumors - The Body's Lumps
- Mesenchymal origin; classified by tissue type (fat, muscle, vascular).
- Benign Tumors: "-oma"
- Lipoma: Most common soft tissue tumor in adults. Mobile, soft, painless.
- Rhabdomyoma: Benign skeletal muscle tumor. Often in the heart (associated with Tuberous Sclerosis).
- Malignant Tumors: "-sarcoma"
- Liposarcoma: Malignant fat tumor; lipoblasts are key.
- Rhabdomyosarcoma: Most common soft tissue sarcoma in children.
⭐ Rhabdomyosarcoma often presents as a "grape-like" mass (sarcoma botryoides) in the vagina or bladder of young girls.
Benign Tumors - Mostly Harmless
Benign soft tissue tumors are common, slow-growing, well-differentiated masses with low metastatic potential. Management is typically surgical excision if symptomatic.
| Tumor | Tissue of Origin | Key Features |
|---|---|---|
| Lipoma | Adipose Tissue | Most common soft tissue tumor in adults. Soft, mobile, painless. |
| Fibroma | Fibroblastic | Firm mass. Ovarian fibromas can cause Meigs syndrome. |
| Leiomyoma | Smooth Muscle | Most common in the uterus ("fibroids"). Whorled pattern of smooth muscle. |
| Rhabdomyoma | Skeletal Muscle | Rare. Cardiac type associated with Tuberous Sclerosis. |
| Hemangioma | Blood Vessels | Common in infancy (strawberry hemangioma); often regress spontaneously. |
Malignant Sarcomas - The Real Villains
- General Features: Deep-seated, large (>5 cm), aggressive tumors. Tend to spread hematogenously (lungs are a common site of metastasis).
- Liposarcoma:
- Most common sarcoma in adults (40-60 years).
- Key feature: Lipoblasts (cells with vacuolated, lipid-rich cytoplasm and a scalloped nucleus).
- Well-differentiated type is associated with MDM2 amplification.
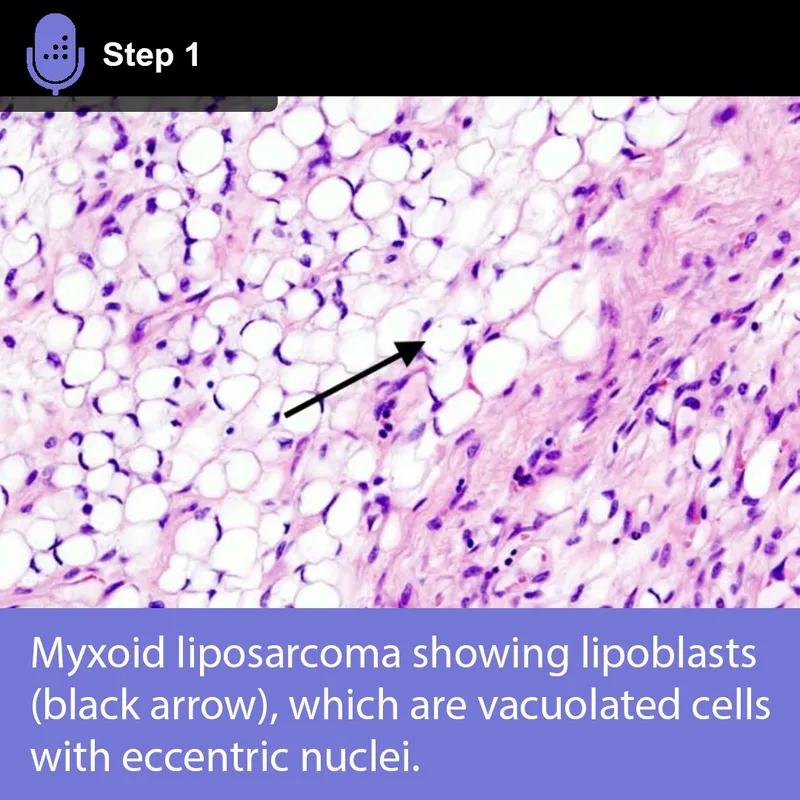
- Rhabdomyosarcoma:
- Most common soft tissue sarcoma in children (<15 years).
- Key cell: Rhabdomyoblast (tadpole or strap cells; may show cross-striations). Stains for desmin, myogenin.
- Embryonal subtype is most common; Alveolar subtype has t(2;13) or t(1;13) translocations and a worse prognosis.
- Synovial Sarcoma:
- Typically affects adolescents and young adults (15-40 years), often near large joints (e.g., knee).
-
⭐ Pathognomonic finding: t(X;18) translocation, resulting in an SS18-SSX fusion protein.
Diagnosis & Genetics - Cracking the Code
- Initial Dx: H&P, imaging (MRI is key).
- Tissue is the Issue: Biopsy (core needle > incisional/excisional) is mandatory before treatment.
- Microscopy: Spindle cells, pleomorphism, mitotic activity.
- Immunohistochemistry (IHC): Crucial for lineage.
- Desmin: Muscle (rhabdomyo-)
- S100: Neural (MPNST)
- CD34: Vascular (angiosarcoma), GIST
⭐ Synovial Sarcoma: Characterized by the t(X;18) translocation, creating an SS18-SSX fusion gene.
- Lipoma is the most common benign soft tissue tumor in adults; liposarcoma is the most common malignant, linked to MDM2 amplification.
- Rhabdomyosarcoma is the most frequent soft tissue sarcoma in children, typically the embryonal type in the head, neck, or genitourinary tract.
- Nodular fasciitis mimics sarcoma with its rapid growth and high cellularity but is a benign, self-limiting process.
- Synovial sarcoma, despite its name, is unrelated to synovium and shows a characteristic t(X;18) translocation.
- Desmoid fibromatosis is locally aggressive but non-metastatic, often associated with APC/β-catenin pathway mutations.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

