Nerve Injury & Repair - Anatomy Under Attack
-
Nerve Sheaths
- Epineurium: Dense connective tissue covering the entire peripheral nerve.
- Perineurium: Surrounds nerve fascicles; forms the blood-nerve barrier.
- Endoneurium: Surrounds individual axons and their Schwann cells.
-
Seddon Classification of Nerve Injury
| Type | Myelin Damage | Axon Damage | Sheath Damage | Recovery |
|---|---|---|---|---|
| Neuropraxia | Yes | No | No | Complete |
| Axonotmesis | Yes | Yes | No (Endo intact) | Good |
| Neurotmesis | Yes | Yes | Yes | Poor/Incomplete |
- Wallerian Degeneration & Regeneration
⭐ Axonal regeneration in the PNS occurs at a rate of approximately 1 mm/day or 1 inch/month.
Guillain-Barré Syndrome - Ground-Up Invasion
- Acute, immune-mediated demyelinating polyneuropathy, often post-infection (Campylobacter jejuni, viruses).
- Pathogenesis involves molecular mimicry, targeting peripheral nerve myelin or axons.
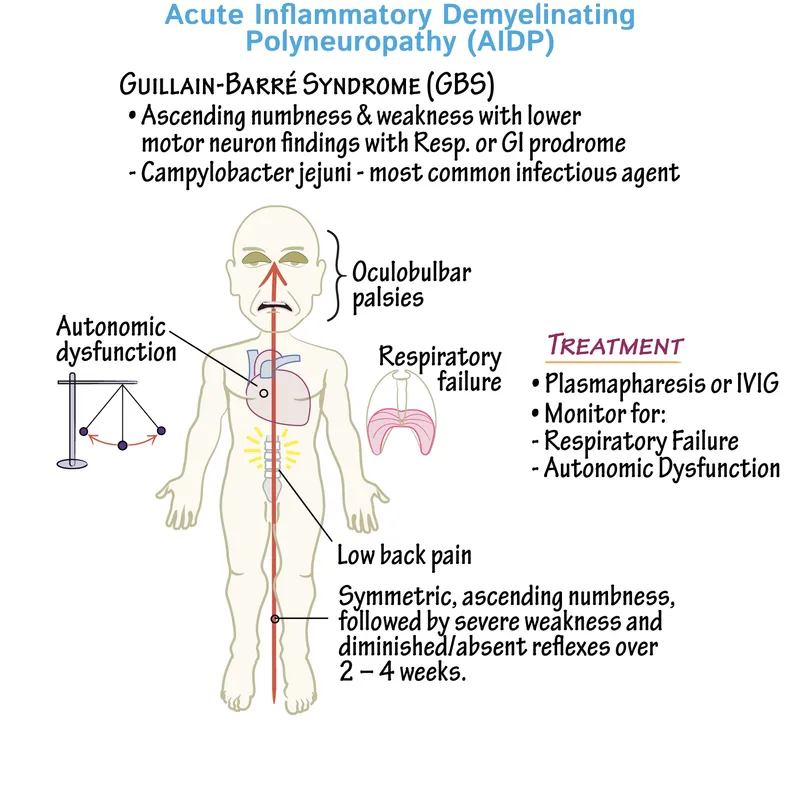
- Clinical: Rapidly progressive, symmetric ascending weakness (📌 "ground-to-brain").
- Starts in legs, ascends to arms, trunk, and face.
- ↓ or absent deep tendon reflexes.
- Autonomic dysfunction (tachycardia, BP changes) and respiratory failure are life-threatening complications.
- Diagnosis & Management:
- Nerve conduction studies show slowed velocity.
- Treatment: IV immunoglobulin (IVIG) or plasmapheresis.
⭐ Key finding is albuminocytologic dissociation in CSF: markedly ↑ protein with a normal cell count, typically seen after the first week.
Chronic Neuropathies - Slow Burn & Wreckage
-
Diabetic Neuropathy: Most common cause of peripheral neuropathy.
- Pathogenesis: Metabolic & vascular damage from chronic hyperglycemia. ↑Advanced glycation end products (AGEs) & sorbitol, ischemic injury to vasa nervorum.
- Clinical: Distal, symmetric sensory or sensorimotor "stocking-and-glove" pattern. Autonomic neuropathy (gastroparesis, orthostatic hypotension) is common.
- Morphology: Axonal degeneration. Hyalinization of endoneurial arterioles.
-
Charcot-Marie-Tooth (CMT) Disease: Most common hereditary peripheral neuropathy.
- Pathogenesis: Genetic defects in myelin- or axon-related proteins (e.g., PMP22 duplication in CMT1A).
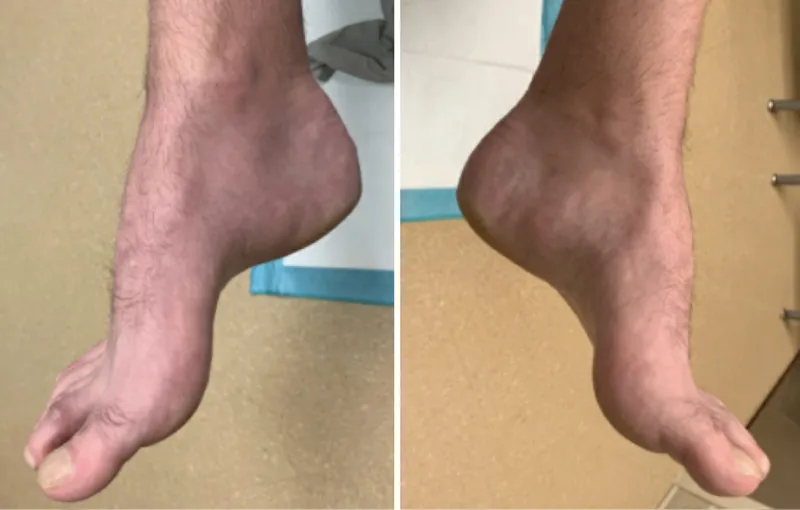
- Clinical: Distal muscle atrophy (e.g., peroneal), sensory loss, pes cavus ("stork leg" deformity).
- Morphology: Repetitive demyelination & remyelination forms concentric layers of Schwann cells.
⭐ Exam Favorite: The characteristic finding in demyelinating forms of CMT is "onion bulb" formation, visible on nerve biopsy, resulting from cycles of Schwann cell proliferation.
High‑Yield Points - ⚡ Biggest Takeaways
- Guillain-Barré syndrome is an acute, ascending paralysis, often post-Campylobacter infection, with albuminocytologic dissociation in CSF.
- Diabetic neuropathy, the most common type, manifests as a distal, symmetric "stocking-glove" sensory loss.
- Charcot-Marie-Tooth is a hereditary motor-sensory neuropathy causing pes cavus and distal muscle atrophy.
- Wallerian degeneration refers to axonal breakdown distal to injury, with debris cleared by macrophages.
- Segmental demyelination from Schwann cell damage slows nerve conduction velocity, a key feature in GBS.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

