Oral Pre-Malignant/Malignant - Risky Business
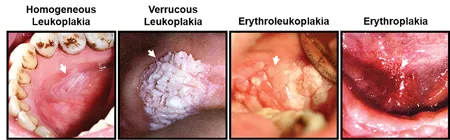
- Leukoplakia: White patch/plaque that cannot be scraped off. Represents epithelial hyperplasia/hyperkeratosis. Biopsy is crucial to rule out dysplasia or carcinoma.
- Erythroplakia: Red, velvety patch. Much higher risk of malignancy than leukoplakia; often represents severe dysplasia or carcinoma in situ.
- Squamous Cell Carcinoma (SCC): Most common oral malignancy (>90%).
- Risk Factors: Tobacco, alcohol (synergistic effect), HPV-16 (esp. oropharyngeal), betel nut chewing, chronic irritation.
⭐ The floor of the mouth is a high-risk site for malignant transformation of leukoplakia.
Salivary Gland Tumors - Glandular Goons
- General Rules: Most tumors in parotid (~80%), most parotid tumors benign. As gland size ↓ (submandibular, sublingual), malignancy risk ↑.
- Benign Tumors:
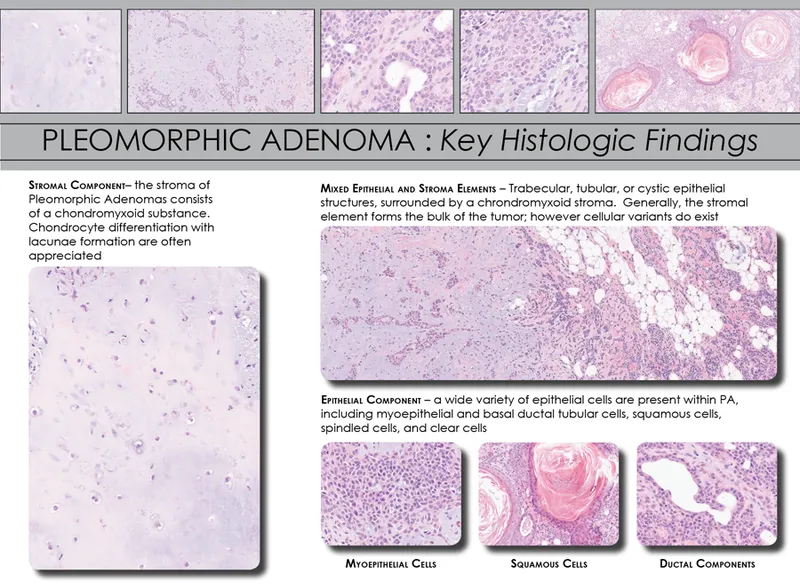
- Pleomorphic Adenoma (Mixed Tumor): Most common overall.
- Painless, mobile mass with chondromyxoid stroma & epithelium.
- High recurrence with incomplete excision.
- Warthin Tumor: Almost exclusive to parotid; strong link to smoking.
- Pleomorphic Adenoma (Mixed Tumor): Most common overall.
- Malignant Tumors:
- Mucoepidermoid Carcinoma: Most common malignant tumor.
- Adenoid Cystic Carcinoma: Cribriform ("Swiss cheese") pattern; perineural invasion causes pain.
⭐ Facial nerve (CN VII) palsy is a significant red flag, strongly suggesting a malignant parotid tumor due to nerve invasion.
Nasopharynx & Larynx - Airway Afflictions
- Nasopharyngeal Carcinoma: Strongly linked to EBV; common in Southern China/Africa. Presents with nasal obstruction, epistaxis, or a metastatic neck mass.
- Laryngeal Papilloma: Benign tumor of vocal cords caused by HPV 6 and 11.
- Single in adults, multiple (recurrent respiratory papillomatosis) in children. Presents with hoarseness.
- Laryngeal Carcinoma (SCC): Key risk factors are smoking and alcohol.
- Persistent hoarseness is a cardinal sign. Other symptoms include dysphagia and cough.
⭐ Undifferentiated nasopharyngeal carcinoma has the strongest association with EBV and often presents with a neck mass from nodal metastasis.
Odontogenic Lesions - Jaw-Dropping Growths
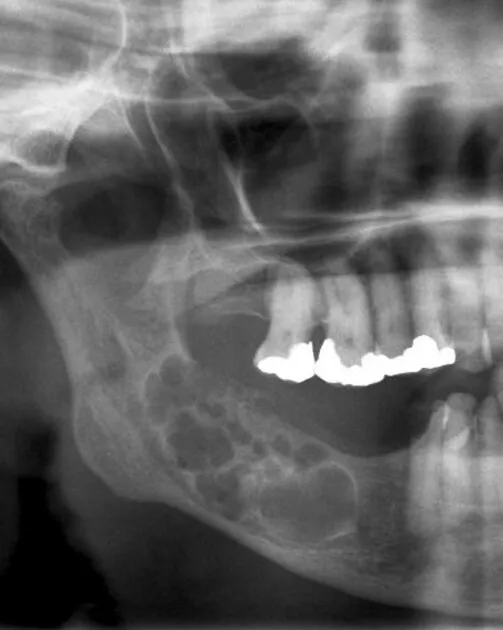
- Ameloblastoma: Benign but locally aggressive. Presents as a "soap bubble" or honeycomb multilocular radiolucency in the posterior mandible. High rate of recurrence if not completely excised.
- Keratocystic Odontogenic Tumor (KCOT): Aggressive cystic lesion known for high recurrence. Often seen in the posterior mandible. Multiple KCOTs are a key feature of Gorlin Syndrome (NBCCS).
- Odontoma: Most common odontogenic tumor; considered a hamartoma.
- Compound: Multiple small, tooth-like structures (denticles).
- Complex: Disorganized mass of dental tissue.
⭐ High-Yield: Ameloblastomas frequently harbor activating mutations in the BRAF V600E gene, a potential target for therapy.
High‑Yield Points - ⚡ Biggest Takeaways
- HPV-16 is a major driver of oropharyngeal SCC, especially in non-smokers, conferring a better prognosis.
- Nasopharyngeal carcinoma, particularly the undifferentiated type, is strongly associated with EBV infection.
- Pleomorphic adenoma is the most common benign tumor of the salivary glands, typically in the parotid.
- Mucoepidermoid carcinoma is the most common malignant salivary gland tumor.
- Branchial cleft cysts present as lateral neck masses, while thyroglossal duct cysts are midline.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

