Hypertensive Nephropathy - Pressure Cooker Kidneys
- Pathophysiology: Chronic hypertension → pressure-induced injury to renal arterioles, leading to luminal narrowing and ischemia.
- Benign Nephrosclerosis (Chronic HTN):
- Gross: Symmetrically atrophic kidneys with a fine, granular cortical surface.
- Micro: Hyaline arteriolosclerosis (glassy, pink thickening of arteriole walls), leading to glomerulosclerosis, tubular atrophy, and interstitial fibrosis.
- Malignant (Accelerated) Hypertension:
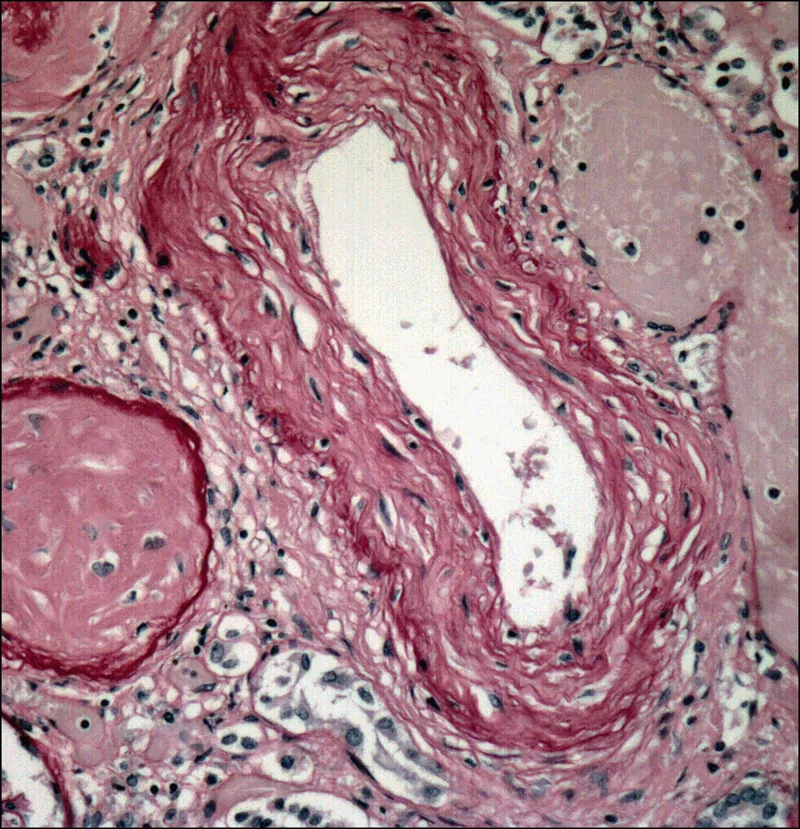
- Micro: Fibrinoid necrosis and hyperplastic arteriolosclerosis ("onion-skinning").
- Gross: "Flea-bitten" appearance from petechial hemorrhages.
⭐ Exam Favorite: The pathognomonic finding for malignant hypertension is hyperplastic arteriolosclerosis, described as "onion-skinning" of arterioles due to concentric smooth muscle proliferation.
Renal Artery Stenosis - The Clogged Pipe
- Etiology: Narrowing of one or both renal arteries, most commonly due to:
- Atherosclerosis (~90%): Elderly males; involves renal artery ostium.
- Fibromuscular Dysplasia (FMD): Younger females; classic "string of beads" appearance on angiography.
- Pathophysiology: Reduced renal blood flow triggers the Renin-Angiotensin-Aldosterone System (RAAS), leading to severe secondary hypertension.
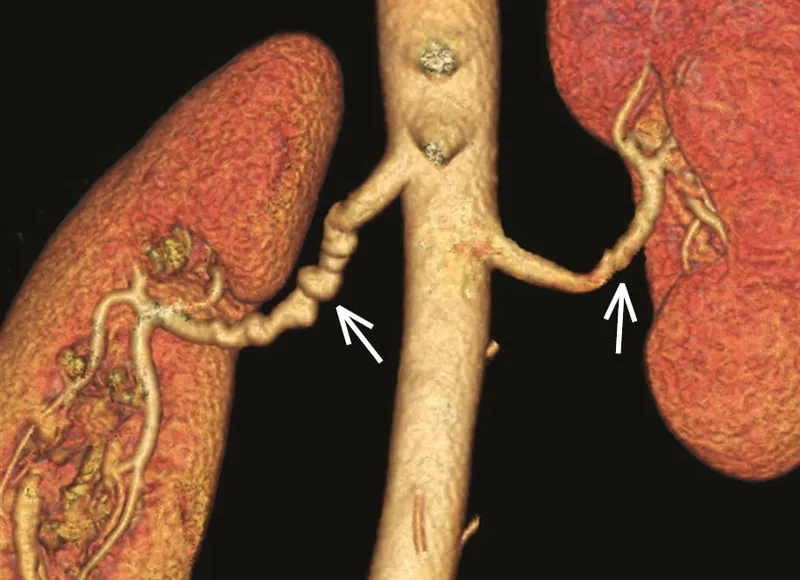
- Clinical Clues:
- Resistant hypertension, especially in patients <30 or >55 years.
- Audible abdominal bruit.
- Recurrent "flash" pulmonary edema.
- Acute kidney injury (↑ Cr >30%) after starting an ACE inhibitor or ARB.
⭐ Unilateral stenosis leads to hypertension; bilateral stenosis can cause both hypertension and renal failure, especially with ACE inhibitor use which preferentially dilates the efferent arteriole, dropping GFR.
Thrombotic Microangiopathies - Tiny Clot Chaos
- Pathophysiology: Endothelial injury triggers widespread platelet activation and microthrombi formation in small vessels.
- Clinical Triad: Microangiopathic hemolytic anemia (MAHA), thrombocytopenia, and organ injury (especially kidney and CNS).
- Thrombotic Thrombocytopenic Purpura (TTP):
- Cause: ↓ ADAMTS13 activity (autoimmune Ab or genetic). Leads to large vWF multimers that trap platelets.
- 📌 FAT RN Pentad: Fever, Anemia, Thrombocytopenia, Renal failure, Neurologic signs.
- Hemolytic Uremic Syndrome (HUS):
- Typical (D+ HUS): Shiga-like toxin (E. coli O157:H7) injures endothelium. Often follows dysentery.
- Atypical (aHUS): Dysregulated complement activation.
- Presents with more prominent acute kidney injury.
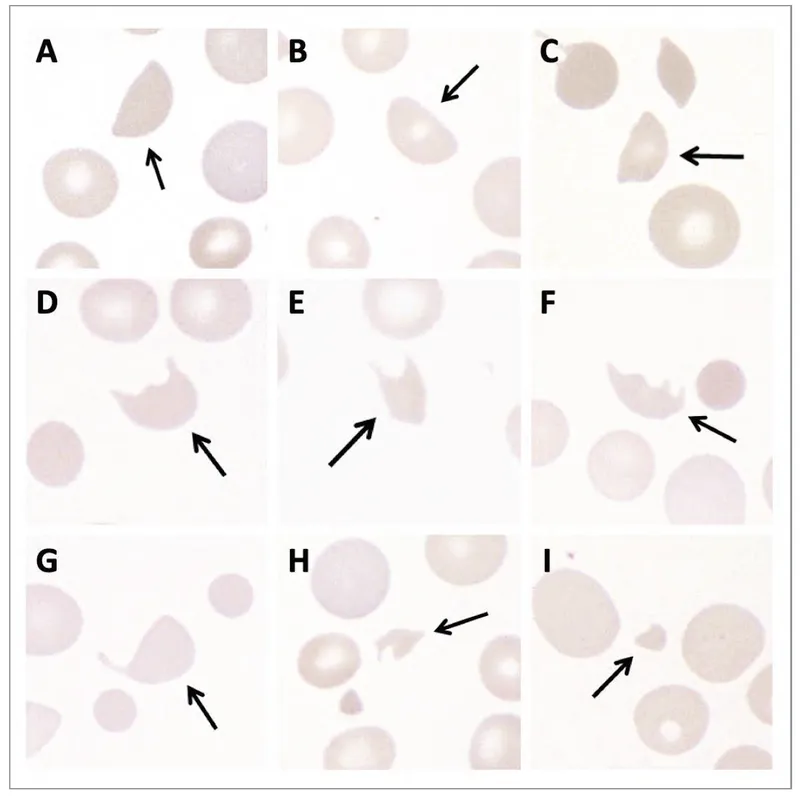
⭐ Key diagnostic clue: Peripheral smear shows schistocytes. Unlike in DIC, coagulation studies (PT/PTT) are characteristically normal.
Embolic & Infarctive Disease - Sudden Blockade
- Etiology: Thromboembolism from the left heart is the most common cause, often secondary to atrial fibrillation or mural thrombi post-myocardial infarction.
- Other sources include septic emboli (endocarditis) and cholesterol emboli (atheroembolism).
- Pathology: Results in wedge-shaped, pale (anemic) infarcts with a base on the cortex and apex pointing to the medulla.
- A thin subcapsular rim of cortex is often spared due to dual blood supply from capsular vessels.
- Microscopy shows coagulative necrosis.
- Clinical: Sudden onset of flank pain, hematuria, and fever.
- Labs: Markedly elevated serum lactate dehydrogenase (LDH) is a classic finding.
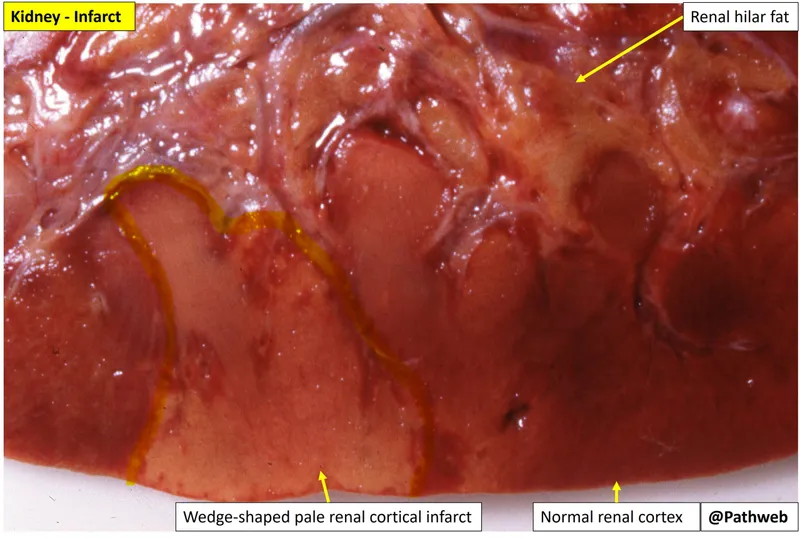
⭐ Renal infarcts are pale (anemic) because the renal arteries are end-arteries with no significant collateral flow. Occlusion leads to ischemic coagulative necrosis without hemorrhage, unlike organs with dual circulation (e.g., lung, liver).
- Renal Artery Stenosis is a key cause of secondary hypertension, driven by atherosclerosis in older men or fibromuscular dysplasia in young women.
- Malignant hypertension shows fibrinoid necrosis and hyperplastic "onion-skin" arteriolosclerosis, creating a "flea-bitten" kidney appearance.
- Thrombotic microangiopathies (TTP/HUS) feature platelet-rich thrombi in glomeruli, causing MAHA and acute kidney injury.
- Atheroembolic disease follows vascular procedures, with cholesterol crystal emboli, livedo reticularis, and eosinophilia.
- Renal vein thrombosis is a major complication of nephrotic syndrome (especially membranous nephropathy).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

