UTI Basics - The Bladder Blues
- Cystitis (lower UTI/bladder) vs. Pyelonephritis (upper UTI/kidney). Most ascend from the urethra.
- Pathogens: >80% E. coli. Others: Staphylococcus saprophyticus (young, sexually active women), Klebsiella pneumoniae, Proteus mirabilis (alkaline urine, struvite stones).
- Risk Factors: Female sex, sexual intercourse, catheterization, urinary stasis (BPH, stones), vesicoureteral reflux.
- Clinical: Dysuria, frequency, urgency, suprapubic pain. Absence of vaginal discharge helps differentiate from vaginitis.
⭐ Positive nitrites on urinalysis are highly specific for gram-negative bacteria (Enterobacteriaceae), which convert nitrates to nitrites.
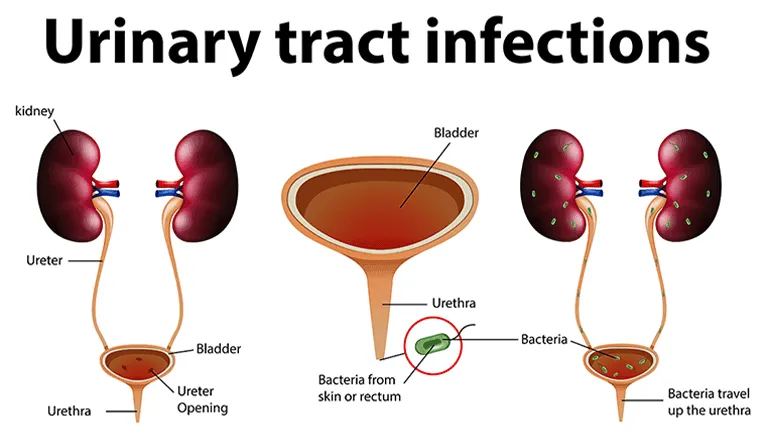
Pathophysiology - The Upstream Battle
- Ascending Infection: The dominant pathway (>95%). Gut flora colonizes the urethra, ascends to the bladder (cystitis), and then travels up the ureters to the kidney parenchyma.
- Key Bacterial Factor: P-fimbriae on uropathogenic E. coli (UPEC) are crucial for adhering to urothelial cells, preventing washout.
- Host Risk Factors:
- Vesicoureteral Reflux (VUR): Retrograde urine flow.
- Obstruction: BPH, calculi, or tumors leading to urine stasis.
- Hematogenous Spread: Less common; typically from S. aureus bacteremia (e.g., endocarditis).
⭐ E. coli is the culprit in >80% of uncomplicated UTIs, using its P-fimbriae for adhesion.
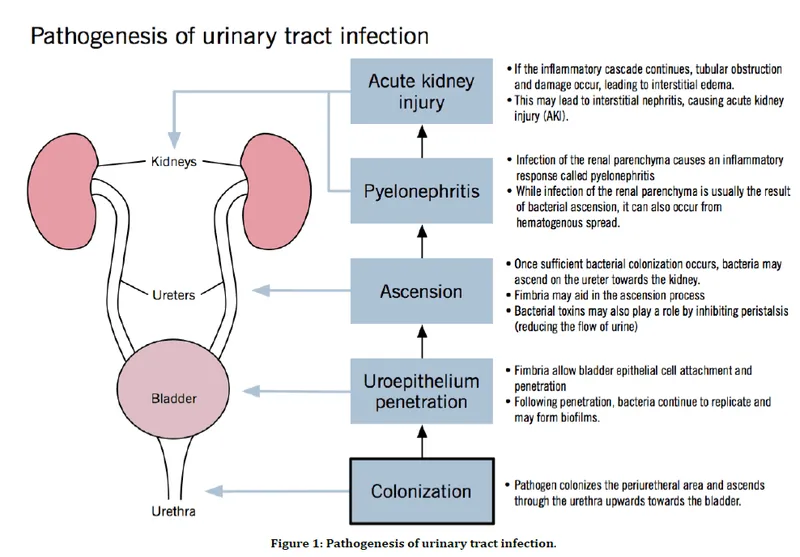
Acute Pyelonephritis - Kidney Under Siege
- Bacterial infection of the kidney parenchyma and renal pelvis, typically from an ascending lower UTI.
- Etiology: Most commonly E. coli. Other causes include Klebsiella, Proteus, and Enterococcus.
- Risk Factors: Vesicoureteral reflux (VUR) in children, urinary tract obstruction (e.g., BPH, stones), catheterization, female sex, pregnancy.
- Clinical Triad: Fever, costovertebral angle (CVA) tenderness, and nausea/vomiting.
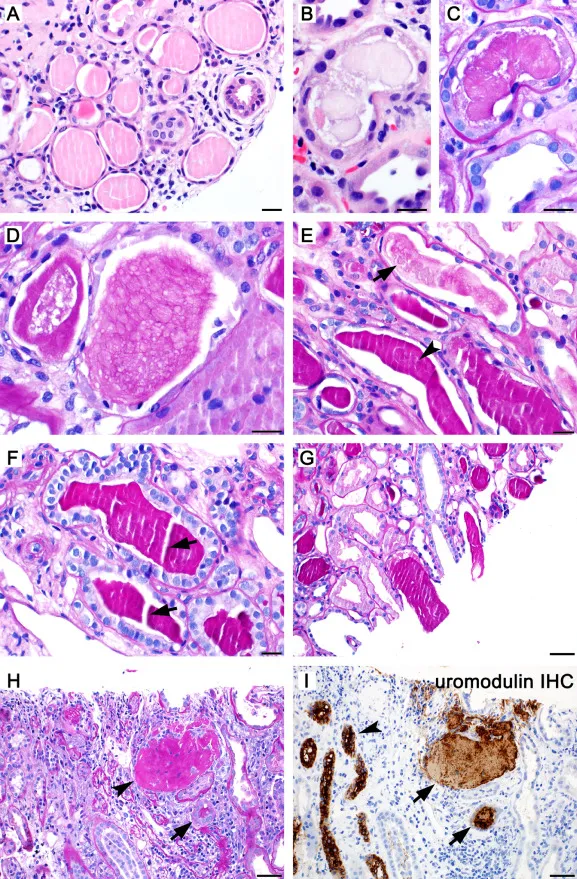
- Pathology: Patchy interstitial inflammation with neutrophils. Neutrophils in tubules form pathognomonic white blood cell (WBC) casts.
⭐ High-Yield: WBC casts are pathognomonic for pyelonephritis or interstitial nephritis, indicating the infection involves the kidney itself, not just the lower urinary tract.
- Complications: Perinephric abscess, pyonephrosis, urosepsis, and renal papillary necrosis.
Chronic Pyelonephritis - The Aftermath & Scars
- Etiology: Typically results from recurrent acute pyelonephritis, often due to vesicoureteral reflux (VUR) in children or chronic obstruction in adults.
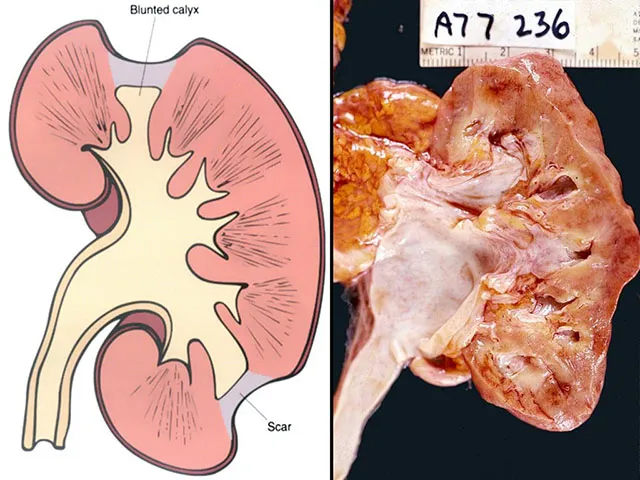
- Gross Pathology: Asymmetrically scarred, contracted kidneys with blunted calyces.
- Microscopic Hallmark:
- Chronic interstitial inflammation (lymphocytes, plasma cells).
- Atrophic tubules containing eosinophilic proteinaceous casts, resembling thyroid follicles (thyroidization).
⭐ High-Yield: Look for coarse, discrete corticomedullary scars overlying dilated, blunted, or deformed calyces on imaging or gross examination.
Complications - When Things Go Wrong
- Renal Papillary Necrosis: Coagulative necrosis of renal papillae. Risk factors: 📌 POSTCARDS (Pyelonephritis, Obstruction, Sickle cell, Tuberculosis, Cirrhosis, Analgesics, Renal vein thrombosis, Diabetes, Systemic vasculitis).
- Perinephric Abscess: Pus collection in the space around the kidney.
- Pyonephrosis: Pus accumulation in an obstructed, infected urinary system; a urologic emergency.
- Urosepsis: Systemic inflammatory response to UTI.
⭐ Emphysematous Pyelonephritis: A severe, necrotizing infection with gas formation in/around the kidney, most common in diabetics. High mortality.
High‑Yield Points - ⚡ Biggest Takeaways
- E. coli is the most common cause, typically via ascending infection.
- Classic presentation includes fever, flank pain (CVA tenderness), and nausea/vomiting.
- WBC casts in urine are pathognomonic for pyelonephritis, distinguishing it from lower UTIs.
- Urinalysis typically shows positive leukocyte esterase and nitrites.
- Serious complications include urosepsis, perinephric abscess, and chronic pyelonephritis.
- Chronic pyelonephritis leads to cortical scarring and histologic thyroidization of tubules.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

