Pathophysiology - Leaky Lungs 101
Fluid balance is governed by Starling's equation: $J_v = K_f [ (P_c - P_i) - \sigma (\pi_c - \pi_i) ]$.
- Cardiogenic: ↑ Hydrostatic pressure ($P_c$) from LV failure or volume overload. Forces protein-poor transudate into interstitium & alveoli.
- Non-Cardiogenic (ARDS): ↑ Permeability ($K_f$) from capillary injury (e.g., sepsis, pneumonia). Leaks protein-rich exudate.
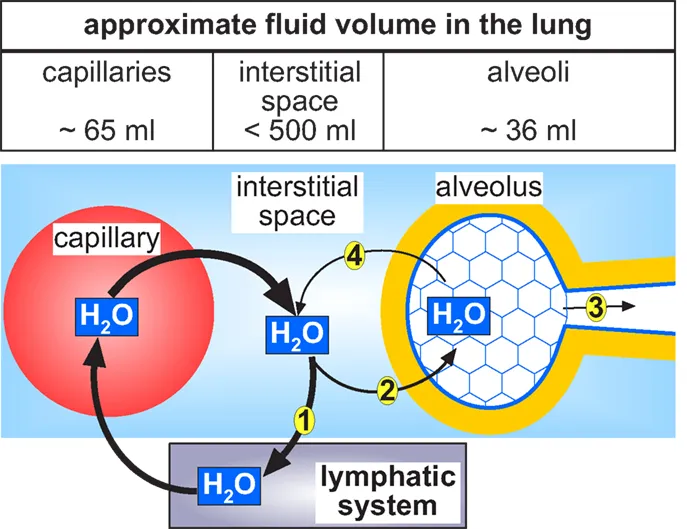
⭐ Edema fluid protein differentiates the cause: it is low in cardiogenic edema (transudate) but high in ARDS (exudate), reflecting the integrity of the capillary barrier.
Etiology - When Lungs Flood
Pulmonary edema results from excess fluid shifting into the pulmonary interstitium and alveoli, driven by an imbalance in Starling forces.
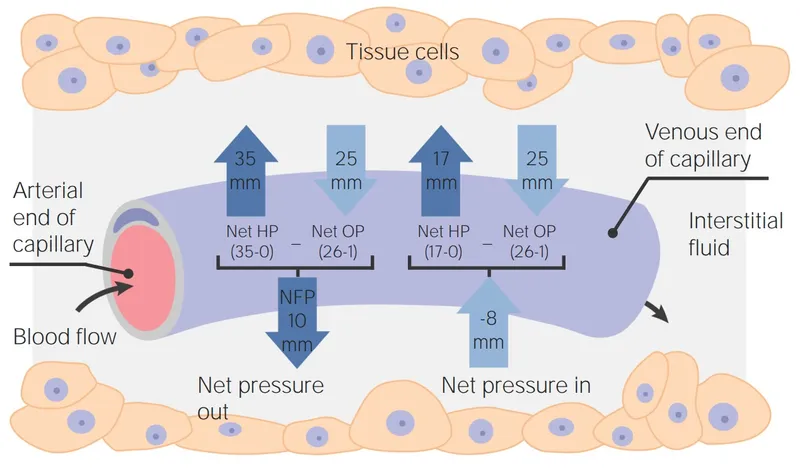
-
Cardiogenic (↑ Hydrostatic Pressure): Most common cause.
- Left ventricular failure (e.g., post-MI)
- Severe hypertension
- Volume overload (e.g., renal failure)
- Mitral or aortic valve disease
-
Non-Cardiogenic (↑ Permeability) / ARDS: Alveolar-capillary membrane damage.
- Sepsis (most common cause of ARDS)
- Pneumonia & Aspiration
- Trauma, pancreatitis, transfusions (TRALI)
- 📌 Mnemonic (ARDS Causes): SPARTAS (Sepsis, Pancreatitis/Pneumonia, Aspiration, uRemia, Trauma, Amniotic fluid embolism, Shock)
⭐ In cardiogenic edema, Pulmonary Capillary Wedge Pressure (PCWP) is >18 mmHg, while in ARDS, PCWP is typically normal (<18 mmHg).
Diagnosis - Crackles, CXR & Catheters
- Auscultation: Bibasilar fine crackles (rales) are characteristic as fluid fills alveoli.
- Chest X-ray (CXR): Key diagnostic tool showing progressive changes.
- Stage 1 (Cephalization): ↑ pressure forces blood to upper lobe vessels.
- Stage 2 (Interstitial Edema):
- Kerley B lines: Short, horizontal lines at lung peripheries.
- Peribronchial cuffing.
- Stage 3 (Alveolar Edema):
- Diffuse, bilateral "batwing" or "butterfly" opacities.
- Pleural effusions, often bilateral.
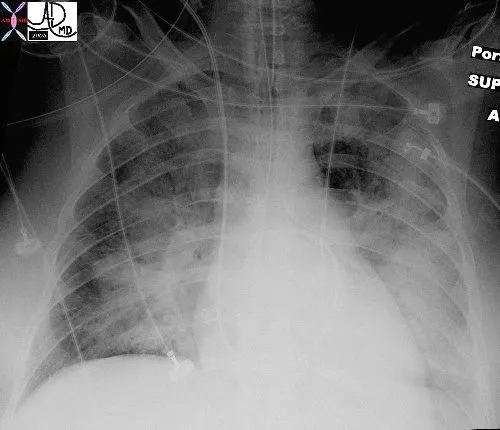
- Pulmonary Artery Catheter (Swan-Ganz): Differentiates cause.
- Measures Pulmonary Capillary Wedge Pressure (PCWP).
- Cardiogenic: PCWP > 18 mmHg.
- Non-cardiogenic (ARDS): PCWP < 18 mmHg.
⭐ High-Yield: Brain Natriuretic Peptide (BNP) is a crucial lab test. A level > 500 pg/mL is highly specific for acute heart failure as the cause of dyspnea and edema.
Management - LMNOP to the Rescue
Initial steps involve sitting the patient upright to decrease venous return and providing supplemental oxygen to correct hypoxemia. The core management follows the 📌 LMNOP mnemonic.
- Lasix (Furosemide): Diuresis to ↓ preload. 40-80 mg IV.
- Morphine: Venodilator ↓ preload; also reduces anxiety & sympathetic drive.
- Nitroglycerin: Potent venodilator ↓ preload. Sublingual or IV.
- Oxygen: Titrate to maintain SpO₂ > 90%.
- Position: Sit patient upright, legs dangling.
⭐ Non-invasive ventilation (BiPAP/CPAP) is a crucial early intervention. It increases intrathoracic pressure, decreasing preload and afterload, and helps recruit alveoli.
High‑Yield Points - ⚡ Biggest Takeaways
- Pulmonary edema is excess fluid in the lung interstitium and alveoli, driven by either ↑ hydrostatic pressure (cardiogenic) or ↑ capillary permeability (non-cardiogenic).
- The most common cause is left-sided heart failure; other key causes include ARDS and nephrotic syndrome.
- Histology reveals engorged capillaries and a characteristic pink, acellular, intra-alveolar transudate.
- Hemosiderin-laden macrophages (“heart failure cells”) are hallmarks of chronic pulmonary congestion.
- Classic clinical signs include dyspnea, orthopnea, PND, and crackles (rales) on auscultation.
- Chest X-ray findings include Kerley B lines, cephalization of pulmonary vessels, and a “batwing” appearance.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

