Obstructive Lung Disease - The Air-Trapping Intro
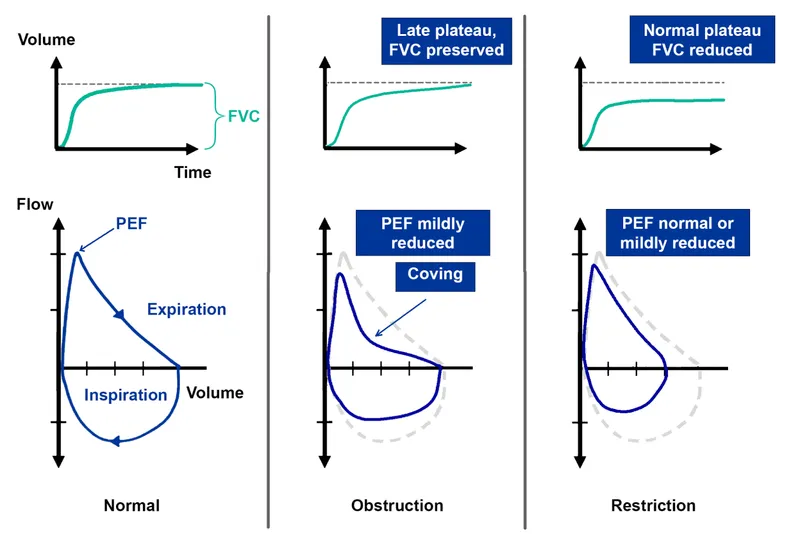
- Defined by airway obstruction causing difficulty with expiration, leading to air trapping.
- Hallmark on spirometry is a decreased FEV₁/FVC ratio ($< \textbf{0.7}$).
- Forced Expiratory Volume in 1 sec (FEV₁) is disproportionately ↓.
- Forced Vital Capacity (FVC) can be normal or ↓.
- Leads to hyperinflation with ↑ lung volumes:
- ↑ Total Lung Capacity (TLC)
- ↑ Functional Residual Capacity (FRC)
- ↑ Residual Volume (RV)
⭐ While the FEV₁/FVC ratio defines obstruction, the absolute FEV₁ value determines its severity (e.g., GOLD stages for COPD).
Chronic Bronchitis - The Blue Bloater
- Clinical Dx: Productive cough for >3 months in >2 consecutive years.
- Pathophysiology: Hypertrophy and hyperplasia of bronchial mucous glands in response to irritants (e.g., smoke).
- Site: Large airways (bronchi).
- ↑ Reid index > 0.5 (ratio of gland depth to bronchial wall thickness).
- Presentation: "Blue Bloater"
- Early-onset hypoxemia (cyanosis) due to shunting.
- Hypercapnia, respiratory acidosis.
- Leads to pulmonary hypertension & cor pulmonale (right heart failure).
⭐ The primary pathology is in the large airways (bronchi), unlike emphysema, which affects the acinus.
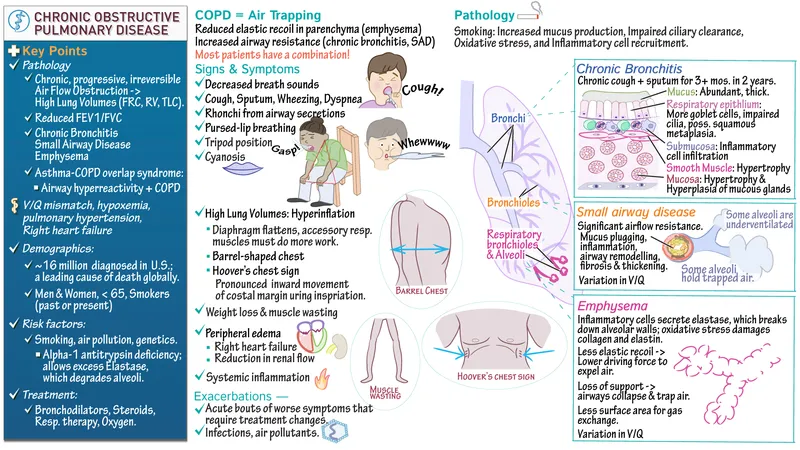
Emphysema - The Pink Puffer
- Pathogenesis: Permanent enlargement of airspaces distal to terminal bronchioles due to alveolar wall destruction. Caused by ↑ elastase activity.
- Centriacinar: Smoking-related (most common).
- Panacinar: α1-antitrypsin (AAT) deficiency.
- Clinical: "Pink Puffer" → pursed-lip breathing, barrel chest (↑ AP diameter), dyspnea, minimal cyanosis.
- Diagnosis: PFTs show obstructive pattern: ↓ FEV₁, ↓ FVC, so ↓ $FEV₁/FVC$ ratio (< 0.7). ↑ TLC, ↑ RV. Markedly ↓ DLCO.
⭐ Look for liver cirrhosis in a young, non-smoking patient with emphysema; it suggests AAT deficiency.
COPD Face-Off - Puffer vs. Bloater
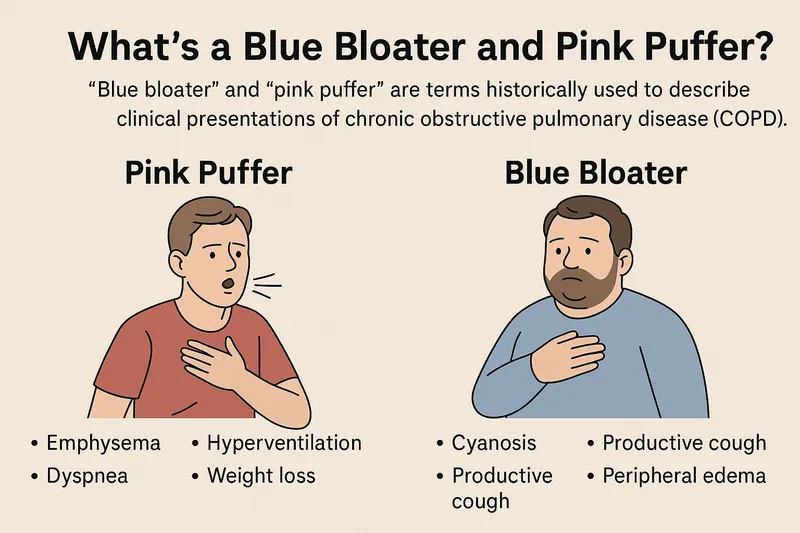
| Feature | Emphysema ("Pink Puffer") | Chronic Bronchitis ("Blue Bloater") |
|---|---|---|
| Pathology | Alveolar wall destruction (↑ elastase). | Mucous gland hypertrophy (Reid Index > 0.5). |
| Appearance | Thin, barrel chest, accessory muscle use. | Cyanotic, edematous (cor pulmonale). |
| Breathing | Pursed-lip breathing, severe dyspnea. | Productive cough (>3 mo/yr for >2 yr). |
| Blood Gas | PaO₂ ↓, PaCO₂ normal/↓. | PaO₂ ↓↓, PaCO₂ ↑↑. |
| DLCO | ↓ (↓ surface area). | Normal. |
| %%{init: {'flowchart': {'htmlLabels': true}}}%% | ||
| flowchart TD |
subgraph Bronchitis [Chronic Bronchitis]
B1["<b>🧬 Gland Change</b><br><span style='display:block; text-align:left; color:#555'>• Mucous gland growth</span><span style='display:block; text-align:left; color:#555'>• Wall thickening</span>"]
B2["<b>💧 Excess Mucus</b><br><span style='display:block; text-align:left; color:#555'>• ⬆️ Sputum production</span><span style='display:block; text-align:left; color:#555'>• Chronic cough</span>"]
B3["<b>🚫 Obstruction</b><br><span style='display:block; text-align:left; color:#555'>• Airway inflammation</span><span style='display:block; text-align:left; color:#555'>• Narrowed lumen</span>"]
B1 --> B2
B2 --> B3
end
subgraph Emphysema [Emphysema]
E1["<b>🔬 Alveolar Damage</b><br><span style='display:block; text-align:left; color:#555'>• Septal destruction</span><span style='display:block; text-align:left; color:#555'>• Large air spaces</span>"]
E2["<b>🩹 Loss of Recoil</b><br><span style='display:block; text-align:left; color:#555'>• Elastin breakdown</span><span style='display:block; text-align:left; color:#555'>• Floppy airways</span>"]
E3["<b>🎈 Hyperinflation</b><br><span style='display:block; text-align:left; color:#555'>• ⬆️ Compliance</span><span style='display:block; text-align:left; color:#555'>• Severe air trapping</span>"]
E1 --> E2
E2 --> E3
end
style B1 fill:#F7F5FD,stroke:#F0EDFA,stroke-width:1.5px,rx:12,ry:12,color:#6B21A8
style B2 fill:#F7F5FD,stroke:#F0EDFA,stroke-width:1.5px,rx:12,ry:12,color:#6B21A8
style B3 fill:#FDF4F3,stroke:#FCE6E4,stroke-width:1.5px,rx:12,ry:12,color:#B91C1C
style E1 fill:#F7F5FD,stroke:#F0EDFA,stroke-width:1.5px,rx:12,ry:12,color:#6B21A8
style E2 fill:#F7F5FD,stroke:#F0EDFA,stroke-width:1.5px,rx:12,ry:12,color:#6B21A8
style E3 fill:#FDF4F3,stroke:#FCE6E4,stroke-width:1.5px,rx:12,ry:12,color:#B91C1C
> ⭐ The diffusing capacity for carbon monoxide (DLCO) is the key differentiating PFT finding. It is **decreased** in emphysema due to destruction of the alveolar-capillary membrane but remains normal in chronic bronchitis.
## High‑Yield Points - ⚡ Biggest Takeaways
> * **COPD** presents with **irreversible airflow obstruction**, primarily from **smoking** or **α1-antitrypsin deficiency**.
> * **Emphysema** ("**Pink Puffer**") features **alveolar destruction**, **↓ elastic recoil**, and a **barrel chest**.
> * **Chronic Bronchitis** ("**Blue Bloater**") is a clinical diagnosis: **productive cough** for **>3 months** over **2 years**.
> * Bronchitis pathology shows **submucosal gland hypertrophy**, with an increased **Reid index > 0.4**.
> * The key diagnostic finding is a **decreased FEV1/FVC ratio (< 0.7)** on spirometry.
> * Both can lead to **pulmonary hypertension** and **cor pulmonale**.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

