Intro to Neuropathies - Nerve Network Nonsense
- Peripheral Neuropathy: A result of damage to nerves outside the brain and spinal cord, leading to sensory, motor, or autonomic dysfunction.
- Key Patterns:
- Mononeuropathy: Single nerve (e.g., Carpal Tunnel).
- Mononeuritis Multiplex: Multiple, non-contiguous nerves (e.g., vasculitis).
- Polyneuropathy: Symmetrical, distal "stocking-glove" pattern.
- Primary Pathologic Processes:
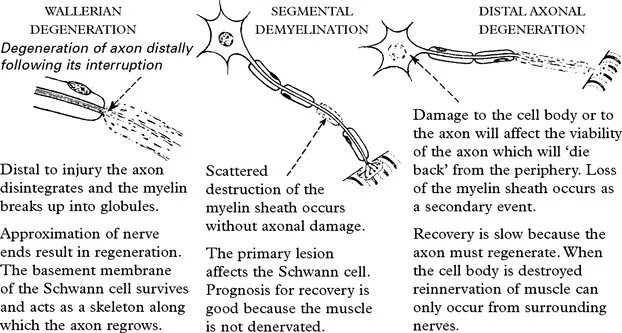
- Axonal Degeneration: "Dying back" process from metabolic/toxic injury; reduces signal amplitude.
- Segmental Demyelination: Schwann cell/myelin damage from immune/hereditary causes; reduces conduction velocity.
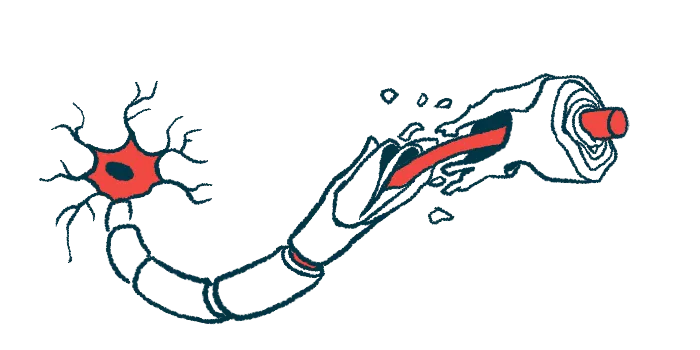
⭐ Wallerian Degeneration: Anterograde degeneration of the axon and myelin sheath distal to a point of injury, like transection.
Guillain-Barré Syndrome - Ascending Paralysis Panic
- Patho: Acute, immune-mediated demyelinating polyneuropathy. Triggered by infections (e.g., Campylobacter jejuni, CMV) via molecular mimicry.
- Clinical: Rapidly progressive, symmetric ascending weakness/paralysis. "Ground-to-Brain."
- ↓ or absent deep tendon reflexes (LMN sign).
- Autonomic dysfunction & respiratory failure are major risks.
- Diagnosis:
- CSF: ↑ protein with normal cell count (albuminocytologic dissociation).
- Nerve conduction studies confirm demyelination.
- Treatment: IVIG or plasmapheresis. Corticosteroids are not effective.
⭐ Exam Favorite: The classic CSF finding is albuminocytologic dissociation, with protein levels typically rising after the first week of symptoms.
📌 Mnemonic: Ground-to-Brain Syndrome.
Diabetic Neuropathy - Sweet & Sour Signals
-
Pathogenesis: Hyperglycemia → ↑intracellular glucose in nerves/Schwann cells.
- Polyol Pathway: Glucose → sorbitol (via aldose reductase) → ↑osmotic stress, ↓Na+/K+ ATPase activity.
- Non-enzymatic Glycation: Forms advanced glycation end-products (AGEs) → inflammation & microvascular damage.
-
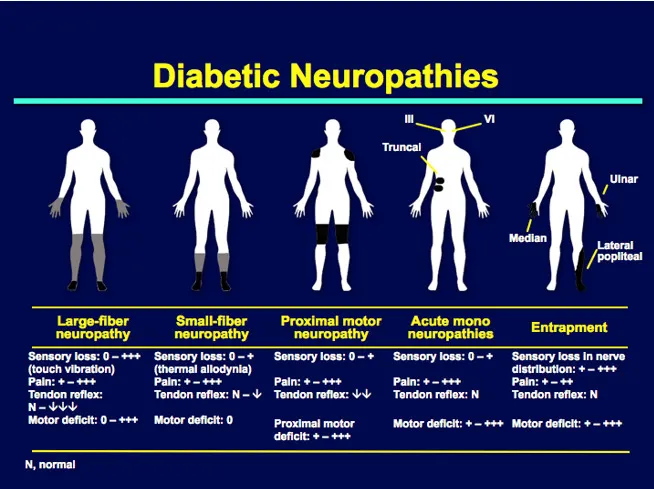
Clinical Types:
- Distal Symmetrical Polyneuropathy (DSPN): Most common. "Stocking-glove" sensory loss (numbness, paresthesias).
- Autonomic Neuropathy: Gastroparesis, orthostatic hypotension, neurogenic bladder, erectile dysfunction.
- Mononeuropathy: Focal nerve damage. 📌 Cranial Nerves III, IV, VI, VII are commonly affected.
⭐ Exam Favorite: Diabetic CN III palsy classically presents with ptosis and a "down and out" eye but spares the pupil. This is because the ischemic damage affects the central somatic fibers while sparing the peripheral parasympathetic fibers.
Hereditary & Traumatic - Genes, Jeans & Jams
-
Charcot-Marie-Tooth (CMT): Most common inherited neuropathy.
- CMT1A (demyelinating): PMP22 gene duplication.
- CMT2 (axonal): Various gene mutations (e.g., MFN2).
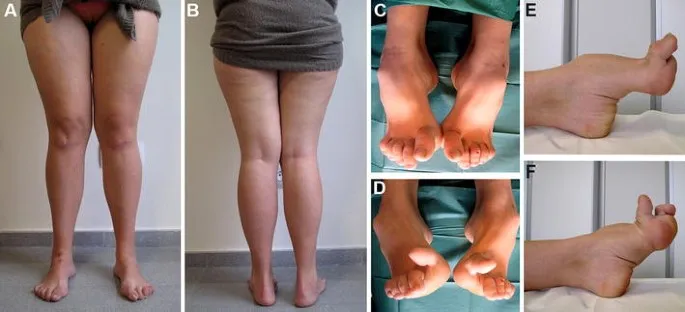
- Classic signs: Distal muscle atrophy (stork legs), pes cavus, foot drop, palpable nerves.
-
Traumatic Injury:
- Wallerian Degeneration: Anterograde degeneration of axon & myelin distal to injury.
- Traumatic Neuroma: Painful, non-neoplastic mass from haphazard nerve regeneration after transection.
⭐ Repetitive demyelination & remyelination (as in CMT1) creates concentric Schwann cell layers visible as "onion bulbs" on histology.
High‑Yield Points - ⚡ Biggest Takeaways
- Guillain-Barré syndrome presents as an acute, ascending paralysis with albuminocytologic dissociation in the CSF, often post-Campylobacter infection.
- Diabetic neuropathy, the most common type, manifests as a "stocking-glove" sensory loss due to non-enzymatic glycosylation and osmotic damage.
- Charcot-Marie-Tooth disease is a hereditary motor-sensory neuropathy causing pes cavus, foot drop, and palpably thickened nerves.
- Wallerian degeneration is axonal breakdown distal to injury, while segmental demyelination from Schwann cell damage slows conduction velocity.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

