Neurodegeneration - Protein Power Down
- Core Mechanism: Misfolded proteins lose normal function & gain toxic properties, resisting degradation and aggregating.
- Key Proteinopathies:
- Alzheimer: Aβ plaques, Tau tangles
- Parkinson/LBD: α-synuclein (Lewy bodies)
- Huntington: Huntingtin (HTT)
- Prion Disease (CJD): Prion protein (PrPSc)
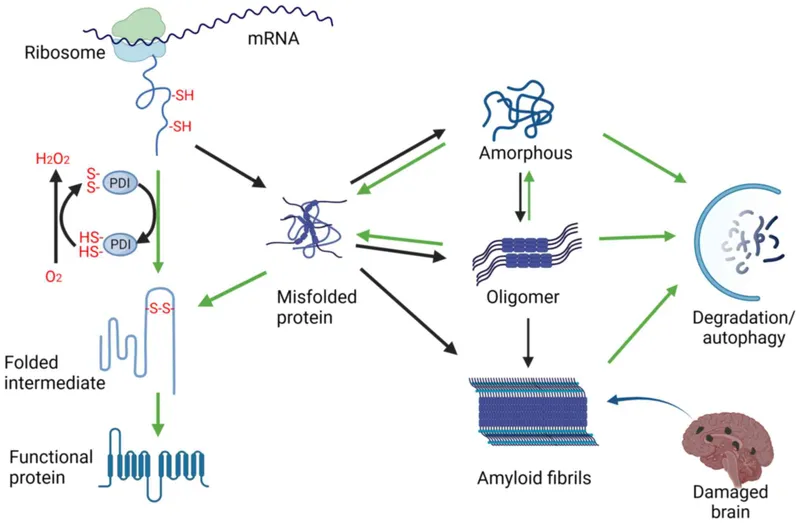
⭐ Prion-like Spread: Misfolded proteins like α-synuclein and tau can propagate from cell to cell, seeding aggregation in a chain reaction.
Alzheimer Disease - Plaque & Tangle Tussle
- Pathology: Extracellular senile plaques (β-amyloid) & intracellular neurofibrillary tangles (hyperphosphorylated tau protein).
- Clinical: Most common cause of dementia. Insidious onset with progressive memory loss (initially short-term), visuospatial deficits, and executive dysfunction.
- Genetics:
- Sporadic (late-onset, >95%): Apolipoprotein E4 (ApoE4) is the major risk factor.
- Familial (early-onset): Mutations in APP (Chr 21), PSEN1 (Chr 14), PSEN2 (Chr 1).
- Gross: Diffuse cortical atrophy, especially hippocampus → hydrocephalus ex vacuo.
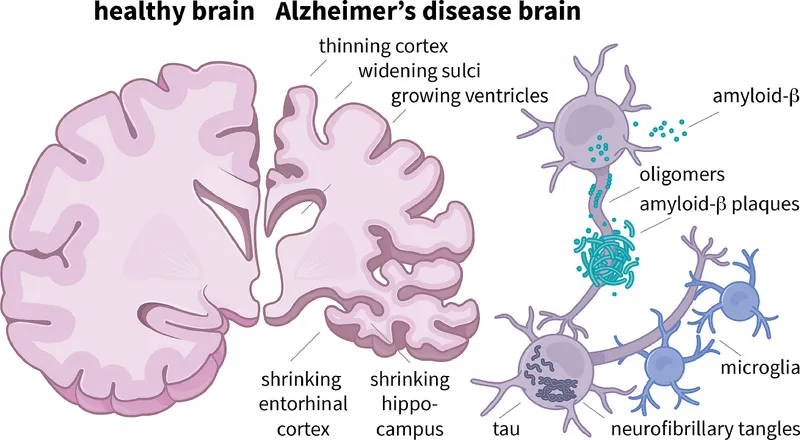
⭐ Patients with Down Syndrome (Trisomy 21) have an extra copy of the APP gene, leading to a significantly increased risk of early-onset Alzheimer's disease.
Synucleinopathies - The Shakes & Slips
-
Parkinson's Disease (PD): Core motor symptoms 📌 TRAP: Tremor (pill-rolling, at rest), Rigidity (cogwheel), Akinesia/bradykinesia, Postural instability.
- Pathophysiology: Loss of dopaminergic neurons in substantia nigra pars compacta. Intraneuronal Lewy bodies (α-synuclein aggregates).
-
Lewy Body Dementia (LBD): Features parkinsonism plus early cognitive decline (dementia < 1 year of motor symptoms), fluctuating cognition, and vivid visual hallucinations.
-
Multiple System Atrophy (MSA): Parkinsonism combined with prominent, early autonomic failure (e.g., orthostatic hypotension) or cerebellar signs.
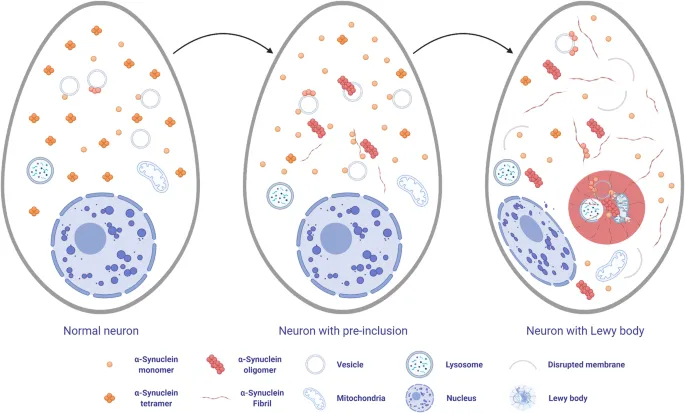
⭐ In LBD, cognitive symptoms appear before or within 1 year of motor symptoms. In PD, dementia is a late complication.
Diverse Pathologies - FTD, HD, ALS & Prions
-
Frontotemporal Dementia (FTD)
- Degeneration of frontal and/or temporal lobes, leading to behavioral or language deficits.
- Pathology: Round tau inclusions (Pick bodies) or TDP-43 inclusions.
-
Huntington's Disease (HD)
- Autosomal dominant; ↑CAG repeats in the HTT gene (anticipation).
- Marked atrophy of the caudate and putamen.
- Loss of GABAergic medium spiny neurons.
- 📌 Choria, Aggressiveness, Grimacing = CAG.
-
Amyotrophic Lateral Sclerosis (ALS)
- Combined Upper (UMN) & Lower (LMN) motor neuron death.
- Pathology: TDP-43 inclusions in motor neurons; Bunina bodies (remains of autophagic vacuoles).
-
Prion Disease (e.g., CJD)
- Pathogenic PrPSc induces misfolding of normal PrPC.
- Causes spongiform encephalopathy (vacuolization).
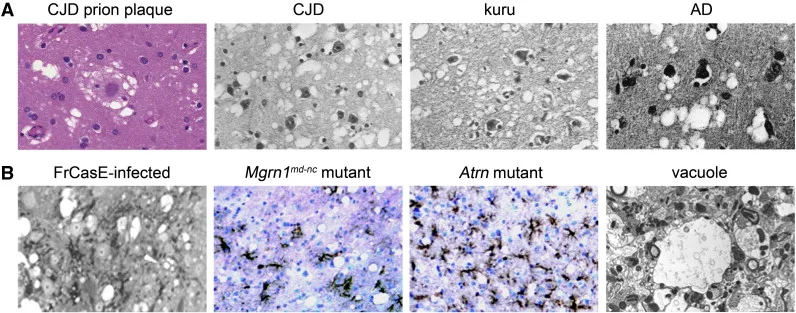
⭐ Creutzfeldt-Jakob Disease (CJD) classically presents as a rapidly progressive dementia with myoclonus and characteristic periodic sharp wave complexes on EEG.
High‑Yield Points - ⚡ Biggest Takeaways
- Alzheimer's disease is defined by extracellular amyloid-β plaques and intracellular neurofibrillary tangles (hyperphosphorylated tau).
- Parkinson's disease features Lewy bodies (α-synuclein) and loss of dopaminergic neurons in the substantia nigra.
- Huntington's disease results from a CAG repeat expansion, leading to caudate and putamen atrophy.
- ALS combines upper and lower motor neuron signs; look for TDP-43 inclusions.
- Creutzfeldt-Jakob disease causes rapidly progressive dementia via spongiform encephalopathy.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

