Demyelination - Myelin Under Attack
- Autoimmune-mediated destruction of the myelin sheath, which slows or blocks nerve impulse conduction.
- Central (CNS): Oligodendrocytes are the primary target. Key diseases include Multiple Sclerosis (MS) and Progressive Multifocal Leukoencephalopathy (PML).
- Peripheral (PNS): Schwann cells are attacked. The classic example is Guillain-Barré Syndrome (GBS).
⭐ In MS, MRI reveals characteristic demyelinating plaques, often in a periventricular distribution.
Multiple Sclerosis - Plaques on the Brain
Grossly visible, demyelinated lesions in the CNS white matter. They represent the focal endpoint of the inflammatory cascade in MS.

- Key Features & Evolution:
- Acute (Active) Plaques: Pink, edematous, ill-defined. Contain perivascular lymphocytes and lipid-laden macrophages (myelin breakdown).
- Chronic (Inactive) Plaques: Gray/tan, firm, sharply demarcated (sclerotic). Characterized by astrocytic proliferation (gliosis) and an absence of myelin.
- Classic Locations:
- Periventricular white matter (Dawson's fingers)
- Juxtacortical
- Infratentorial (brainstem, cerebellum)
- Spinal cord
⭐ High-Yield: Plaques often have a characteristic ovoid shape and are oriented perpendicular to the lateral ventricles, following the path of deep medullary veins. This is the basis for the classic "Dawson's fingers" sign on sagittal MRI.
MS Differentials - Mimics & Variants
- Inflammatory/Post-infectious
- ADEM (Acute Disseminated Encephalomyelitis): Monophasic, post-infectious/vaccination, affects children.
- NMOSD (Neuromyelitis Optica): Relapsing; targets optic nerves & spinal cord. AQP4-IgG positive.
- Neurosarcoidosis: Granulomatous inflammation; cranial neuropathies, leptomeningeal enhancement.
- Infectious
- PML (Progressive Multifocal Leukoencephalopathy): JC virus in immunosuppressed (HIV, natalizumab).
- Lyme Neuroborreliosis: Borrelia burgdorferi; facial palsy, radiculoneuritis.
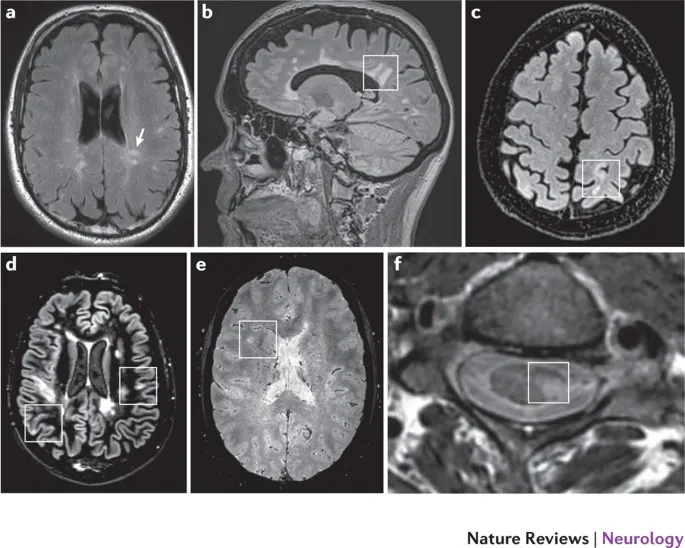
⭐ NMO Spectrum Disorder (NMOSD) is distinguished from MS by the presence of Aquaporin-4 antibodies (AQP4-IgG), which are highly specific and target astrocytic foot processes.
- MS Variants (Fulminant)
- Marburg Type: Acute, monophasic, severe course with large lesions.
- Balo's Concentric Sclerosis: Lamellar, onion-like rings of demyelination.
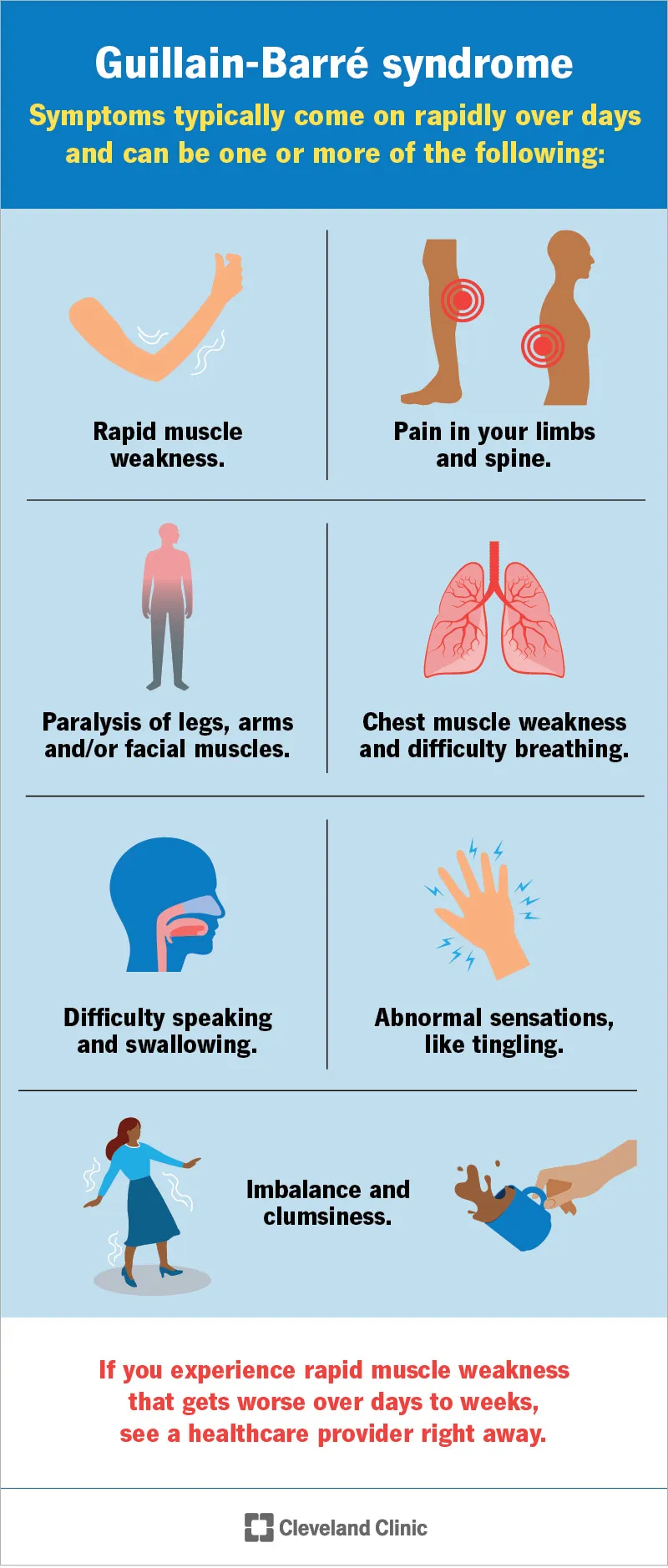
Guillain-Barré Syndrome - Crawling Paralysis
- Pathogenesis: Acute, immune-mediated inflammatory polyneuropathy causing demyelination of peripheral nerves. Frequently triggered by infections (Campylobacter jejuni, CMV) through molecular mimicry.
- Clinical: Classic presentation is a rapidly ascending, symmetric paralysis.
- Starts in lower extremities, progressing upwards over days to weeks.
- Key sign: Areflexia or marked hyporeflexia.
- May involve cranial nerves and respiratory muscles.
- Autonomic dysfunction (tachycardia, BP instability) is common.
- Diagnosis:
- CSF: Albuminocytologic dissociation (↑↑ protein, normal WBC count).
- EMG/NCS: Markedly slowed nerve conduction velocity.
- Treatment: IV immunoglobulins (IVIG) or plasmapheresis.
⭐ Exam Favorite: The most life-threatening complication is respiratory failure from paralysis of the diaphragm and intercostal muscles.
📌 Mnemonic: Ground-to-Brain Syndrome.
High‑Yield Points - ⚡ Biggest Takeaways
- Multiple Sclerosis (MS) is an autoimmune CNS disease with periventricular plaques and oligoclonal bands in the CSF.
- Guillain-Barré Syndrome (GBS) is a PNS condition, often post-infectious, causing ascending paralysis with albuminocytologic dissociation in CSF.
- Progressive Multifocal Leukoencephalopathy (PML) results from JC virus in the immunosuppressed, leading to widespread CNS demyelination.
- Charcot-Marie-Tooth is a hereditary PNS neuropathy causing distal muscle weakness and high-arched feet.
- Acute Disseminated Encephalomyelitis (ADEM) is a post-infectious CNS demyelination, primarily in children.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

