Ischemic Stroke - The Brain's Plumbing Problem
Brain injury from ↓ blood flow, creating a core infarct surrounded by a salvageable ischemic penumbra. Time is brain; intervention aims to save the penumbra.

- Etiologies:
- Thrombotic: Atherosclerotic plaque rupture in cerebral arteries.
- Embolic: Clot from heart (AFib) or large arteries travels to the brain.
- Systemic Hypoperfusion: "Watershed" infarcts from shock/hypotension.
⭐ Histological "red neurons" (eosinophilic cytoplasm, pyknotic nuclei) are the first microscopic sign, visible at 12-24 hours post-infarct.
Vascular Territories - Stroke's GPS

-
Anterior Cerebral Artery (ACA)
- Supplies: Medial surface of the brain (1° motor/sensory cortex for leg-foot).
- Deficits: Contralateral paralysis and sensory loss in the lower limb.
-
Middle Cerebral Artery (MCA)
- Supplies: Lateral convexity of the brain, including speech areas.
- Deficits: Contralateral face/arm paralysis & sensory loss, aphasia (dominant hemisphere), or hemineglect (non-dominant).
⭐ The MCA is the most frequently affected vessel in ischemic stroke.
-
Posterior Cerebral Artery (PCA)
- Supplies: Occipital lobe.
- Deficits: Contralateral homonymous hemianopia with macular sparing.
-
Lenticulostriate Arteries
- Branches of MCA supplying deep structures (basal ganglia, internal capsule).
- Occlusion causes pure motor or pure sensory lacunar strokes.
Hemorrhagic Stroke - When Pipes Burst
- Pathophysiology: Bleeding into brain parenchyma (intracerebral) or subarachnoid space.
- Intracerebral Hemorrhage (ICH):
- Causes: Chronic hypertension (basal ganglia), cerebral amyloid angiopathy (lobar, elderly), AVMs, tumors.
- Mechanism: Rupture of Charcot-Bouchard microaneurysms.
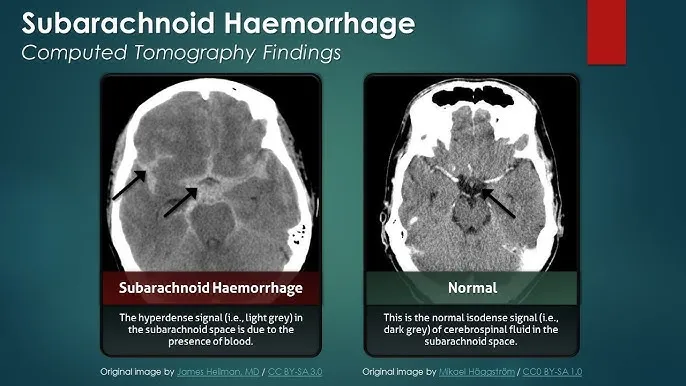
- Subarachnoid Hemorrhage (SAH):
- Presentation: Sudden "worst headache of my life," nuchal rigidity.
- Causes: Ruptured saccular (berry) aneurysm (85%), trauma, AVM.
- Diagnosis: Non-contrast CT. Lumbar puncture shows xanthochromia.
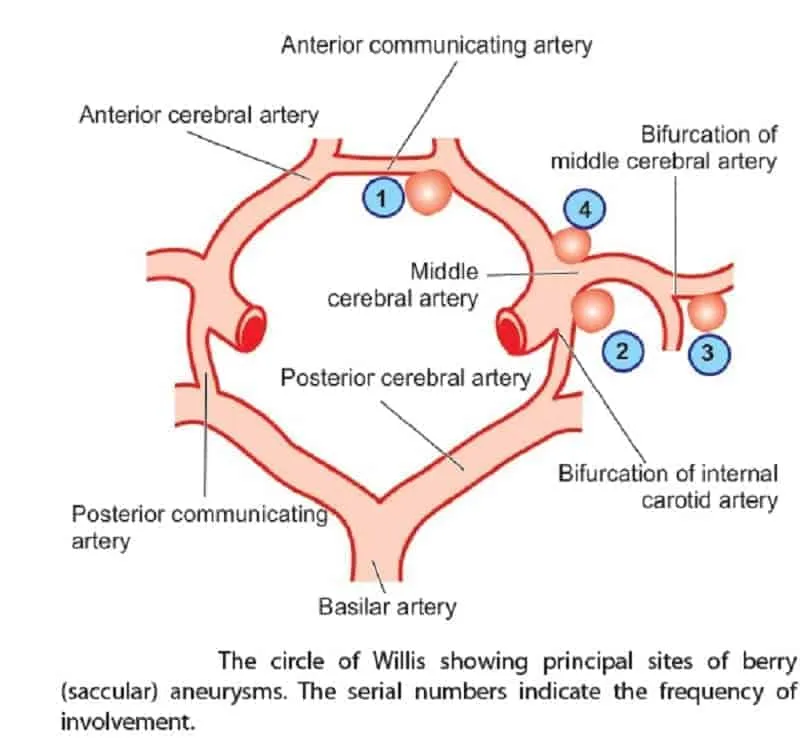
⭐ Berry aneurysms are common at Circle of Willis branch points (esp. AComA) and are associated with ADPKD and Ehlers-Danlos syndrome.
Aneurysms & Malformations - Ticking Time Bombs
- Saccular (Berry) Aneurysm: Most common cause of non-traumatic subarachnoid hemorrhage (SAH). Thin-walled outpouching, lacks media layer. Associated with ADPKD, Ehlers-Danlos syndrome.
- Location: Anterior Communicating Artery (ACoA).
- Charcot-Bouchard Microaneurysm: Affects small vessels (<300 μm) from chronic hypertension; may rupture, causing intracerebral hemorrhage (e.g., basal ganglia).
- Arteriovenous Malformation (AVM): Congenital tangle of arteries & veins.
⭐ Ruptured saccular aneurysm → SAH → classic complaint of "worst headache of my life."
High‑Yield Points - ⚡ Biggest Takeaways
- Ischemic strokes (~85%) are most common, typically from atherosclerosis or cardioembolism (e.g., atrial fibrillation).
- The Middle Cerebral Artery (MCA) is the most frequently involved vessel in ischemic stroke.
- Hypertension is the main risk factor for deep intraparenchymal hemorrhages (Charcot-Bouchard microaneurysms) and lacunar infarcts.
- Subarachnoid hemorrhage classically presents as a "thunderclap headache" from a ruptured berry aneurysm.
- Watershed infarcts affect border zones between arterial territories, often due to severe systemic hypotension.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

