Acute Inflammation - The First Responders
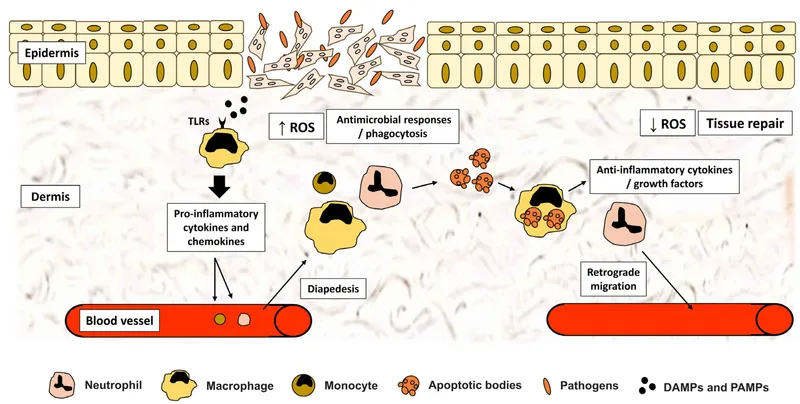
- Triggers: Microbial Pathogen-Associated Molecular Patterns (PAMPs) or host-derived Damage-Associated Molecular Patterns (DAMPs).
- Sensors: Sentinel cells like macrophages and mast cells use Pattern Recognition Receptors (e.g., Toll-like receptors - TLRs).
- Amplification: The inflammasome, a cytosolic complex, activates caspase-1, leading to the maturation and release of IL-1β.
⭐ The inflammasome-driven production of IL-1β is a critical step, making IL-1 a key therapeutic target in several autoinflammatory syndromes.
Vascular Changes - The Floodgates Open
- Vasodilation: Arterioles expand, causing ↑ blood flow.
- Mediators: Histamine, bradykinin, Nitric Oxide.
- Cardinal Signs: Rubor (redness) & Calor (heat).
- ↑ Vascular Permeability: Endothelial cell contraction opens gaps, allowing protein-rich exudate to leak into tissues.
- Result: Tumor (swelling/edema) & ↑ interstitial fluid.
- Dolor (pain) is mediated by bradykinin and prostaglandins.
Fluid movement is governed by Starling forces: $P_{net} = [(P_c - P_i) - \sigma(\pi_c - \pi_i)]$
⭐ Exudate (inflammatory) is protein-rich (sp. gr. > 1.020) and cellular, unlike transudate (hydrostatic), which is a protein-poor ultrafiltrate.

Cellular Events - Leukocyte Invasion
Leukocytes journey from the vessel lumen to the interstitial tissue in a defined sequence to fight infection and clear debris. This multi-step process is mediated by specific adhesion molecules and chemokines.
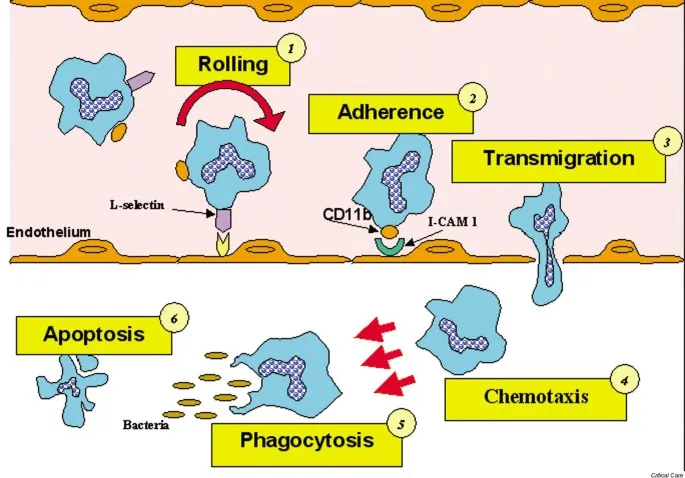
- Margination & Rolling: Slow blood flow pushes leukocytes to the periphery. Endothelial E/P-selectins loosely bind to leukocytes.
- Adhesion: Integrins on leukocytes bind firmly to endothelial ICAM-1. 📌 Mnemonic: Selectins for Slowing/rolling; Integrins for Immobile adhesion.
- Transmigration (Diapedesis): Leukocytes squeeze between endothelial cells, mediated by PECAM-1 (CD31).
- Chemotaxis: Cells migrate toward inflammatory stimuli like $C5a$, $LTB_4$, and IL-8.
⭐ In Leukocyte Adhesion Deficiency (LAD), defective integrins lead to recurrent bacterial infections without pus formation and delayed separation of the umbilical cord.
Phagocytosis - The Clean-Up Crew
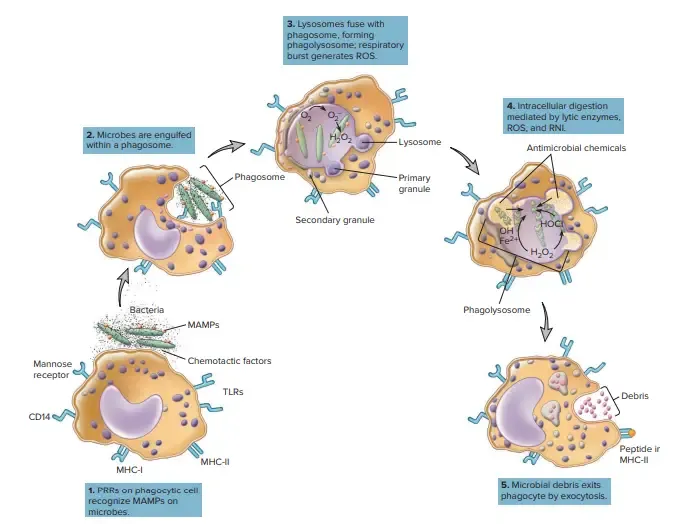
- Opsonization: Pathogens are tagged for destruction by opsonins, primarily IgG and C3b.
- Engulfment & Destruction: Phagocytes engulf tagged pathogens into a phagosome. This fuses with a lysosome to form a phagolysosome, where destruction occurs.
- Killing Mechanisms:
- Respiratory Burst: The primary method. Utilizes oxygen to create reactive oxygen species. $O_2 \xrightarrow{NADPH \text{ oxidase}} O_2^{\cdot-} \xrightarrow{SOD} H_2O_2 \xrightarrow{MPO} HOCl$ (bleach)
- NETs: Neutrophil Extracellular Traps are webs of DNA and proteins released to trap and kill pathogens.
⭐ Chronic Granulomatous Disease (CGD) results from a defective NADPH oxidase, leading to recurrent infections by catalase-positive organisms.
Chemical Mediators - The Conductors
Orchestrate inflammation from two sources:
-
Cell-Derived (Ready or made on demand):
- Histamine: Vasodilation, ↑ vascular permeability.
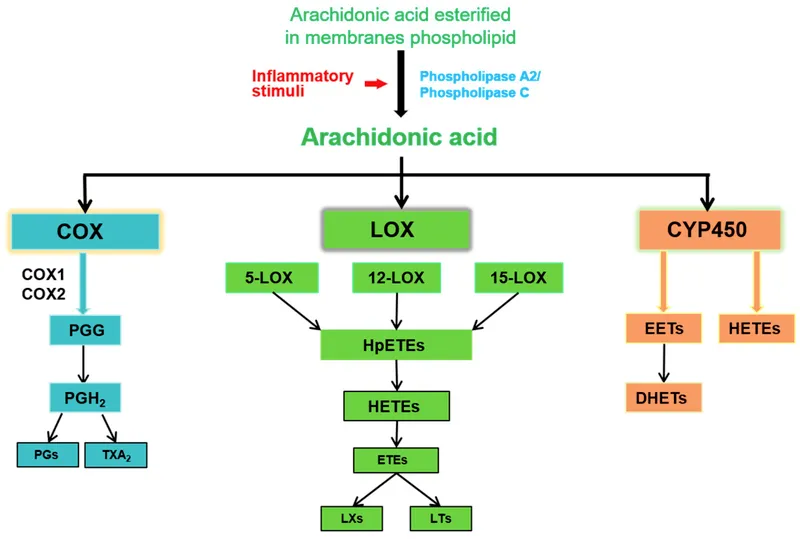
- Arachidonic Acid Metabolites:
- Prostaglandins (via COX): Pain, fever.
- Leukotrienes (via Lipoxygenase): Chemotaxis, bronchospasm.
- Cytokines: TNF, IL-1, IL-6 drive systemic effects (fever).
-
Plasma-Derived (From liver):
- Complement: C3a/C5a (inflammation), C3b (opsonization).
- Kinin System: Bradykinin (pain, vasodilation).
⭐ The cytokine triad of TNF, IL-1, and IL-6 drives the systemic acute-phase response, causing fever and hepatic synthesis of proteins like C-reactive protein (CRP).
High‑Yield Points - ⚡ Biggest Takeaways
- Key vascular changes are vasodilation (redness, heat) and increased permeability (swelling), driven by histamine and bradykinin.
- Neutrophil extravasation is a cascade: rolling (selectins), adhesion (integrins), and transmigration (PECAM-1).
- Chemotaxis is crucial for recruitment, guided by potent chemoattractants like C5a, LTB4, and IL-8.
- Pain is mediated by bradykinin and PGE₂; fever is driven by cytokines like TNF and IL-1.
- Phagocytosis relies on opsonization by IgG and C3b to clear pathogens and debris effectively.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

