Normal Wound Healing - The Repair Blueprint
- A sequential, four-phase process to restore tissue integrity. Key for tissue repair but can result in fibrosis.
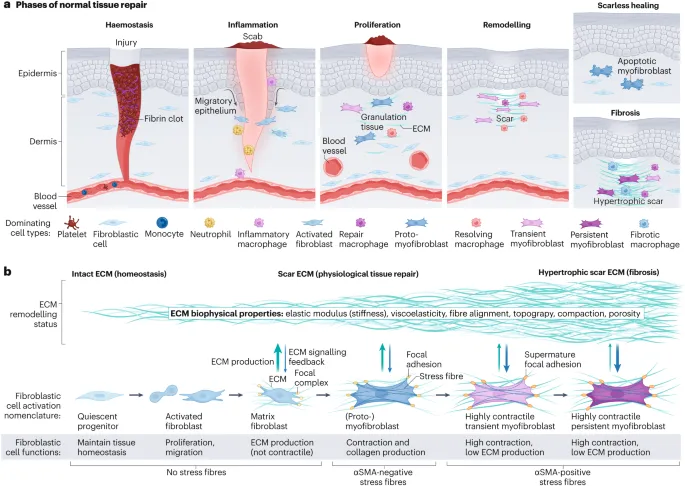
⭐ The switch from Type III collagen (early, weak) to Type I collagen (late, strong) is critical for increasing tensile strength. Wound strength reaches ~80% of original tissue by 3 months but never fully recovers.
Deficient Healing - When Things Fall Apart
- Wound Dehiscence: Rupture of a wound, most often along a surgical incision. A serious complication that can lead to evisceration.
- Ulceration: Formation of a local defect on the surface of an organ or tissue due to inadequate vascularization during healing. Common in patients with peripheral vascular disease, neuropathy (e.g., diabetic foot ulcers), or prolonged pressure.
Key Impairing Factors:
- Systemic Factors:
- Nutrition: ↓ Protein, ↓ Vitamin C (scurvy), or ↓ Zinc impairs collagen synthesis.
- Metabolic: Diabetes mellitus.
- Circulatory: Poor perfusion (arterial or venous disease).
- Hormonal: ↑ Glucocorticoids.
- Local Factors:
- Infection: The single most common cause of delayed healing.
- Mechanical: Early motion, local pressure.
- Foreign bodies.
⭐ Vitamin C is an essential co-factor for lysyl hydroxylase, an enzyme crucial for collagen cross-linking. Deficiency results in unstable collagen and weak scar tissue.

Excessive Scarring - Too Much Good Stuff
- Over-healing due to excess collagen deposition or granulation tissue. Two main types: Keloids and Hypertrophic Scars.
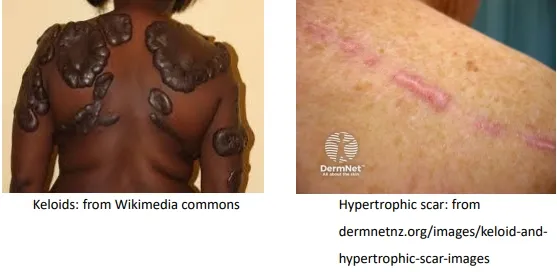
| Feature | Keloid | Hypertrophic Scar |
|---|---|---|
| Borders | Extends beyond original wound | Confined to original wound |
| Collagen | Disorganized Type I & III | Primarily Type III, parallel |
| Genetics | ↑ incidence in African ethnicity | No major genetic link |
| Recurrence | Frequent after resection | Infrequent |
- Excess granulation tissue protrudes above the wound, blocking re-epithelialization.
- Requires cautery or surgical removal.
⭐ Keloids are a classic example of a fibroproliferative disorder with a very high recurrence rate post-excision, unlike hypertrophic scars. This is a key management challenge.
Wound Contracture - A Tight Squeeze
- An exaggeration of normal wound contraction, a key phase in healing by secondary intention.
- Pathophysiology: Driven by the excessive action of myofibroblasts, which contract and pull wound edges together, leading to tissue deformity.
- Clinical Impact: Causes significant cosmetic and functional impairment, particularly over joints (e.g., axilla, fingers) and on palms or soles.
- Commonly develops after severe burns.
⭐ High-Yield: Myofibroblasts are the primary cells responsible for wound contraction. Their overactivity leads to pathologic contracture, causing significant functional deficits.
High‑Yield Points - ⚡ Biggest Takeaways
- Keloids grow beyond original wound margins due to excess Type III collagen; hypertrophic scars stay within.
- Wound dehiscence is the premature opening of a wound, often due to infection or increased pressure.
- Contractures are an exaggerated healing process, common after burns, leading to deformity and limited mobility.
- Ulceration occurs from inadequate vascularization or innervation, preventing complete healing.
- Vitamin C and copper deficiency impair collagen synthesis; zinc deficiency impairs collagenase.
- Glucocorticoids inhibit inflammation, leading to decreased wound strength.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

