Malabsorption - Gut Feeling Gone Wrong
- Pathophysiology: Impaired intestinal absorption of nutrients, leading to steatorrhea, weight loss, and vitamin deficiencies.
- Classification:
- Pancreatic Insufficiency: ↓ Lipase (e.g., Chronic Pancreatitis, Cystic Fibrosis).
- Bile Salt Deficiency: ↓ Micelle formation (e.g., Cholestasis, Bacterial Overgrowth).
- Mucosal Defects: ↓ Surface area (e.g., Celiac Disease, Whipple Disease).
⭐ The D-xylose test distinguishes mucosal from pancreatic causes. Low urinary/serum D-xylose suggests a mucosal defect as its absorption is independent of pancreatic enzymes.
Celiac Disease - Gluten's Arch Nemesis
- Autoimmune-mediated intolerance to gliadin (a gluten protein) found in wheat, barley, and rye.
- Strongly associated with HLA-DQ2 and HLA-DQ8.
- Clinical Features: Chronic diarrhea/steatorrhea, bloating, weight loss, and nutritional deficiencies (e.g., iron deficiency anemia).
- Diagnosis:
- Initial test: IgA anti-tissue transglutaminase (tTG) antibodies.
- Gold standard: Small bowel biopsy showing histologic changes.
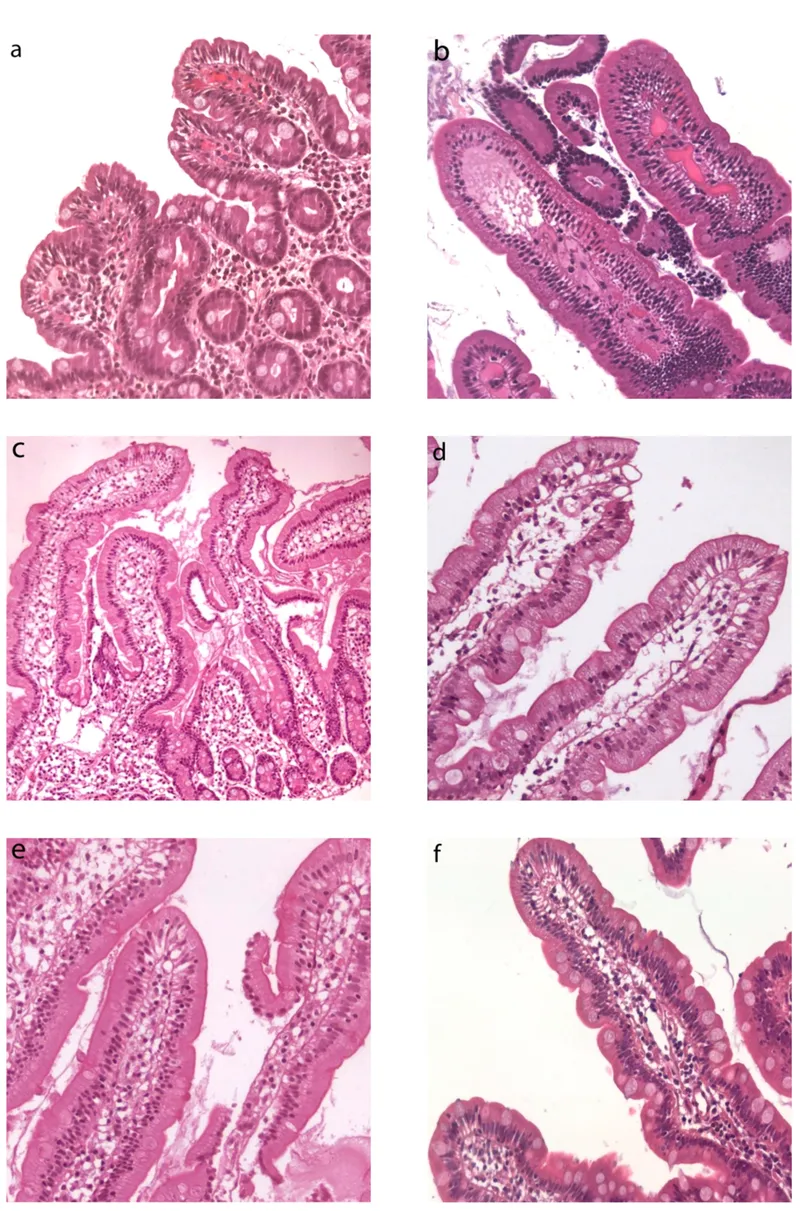
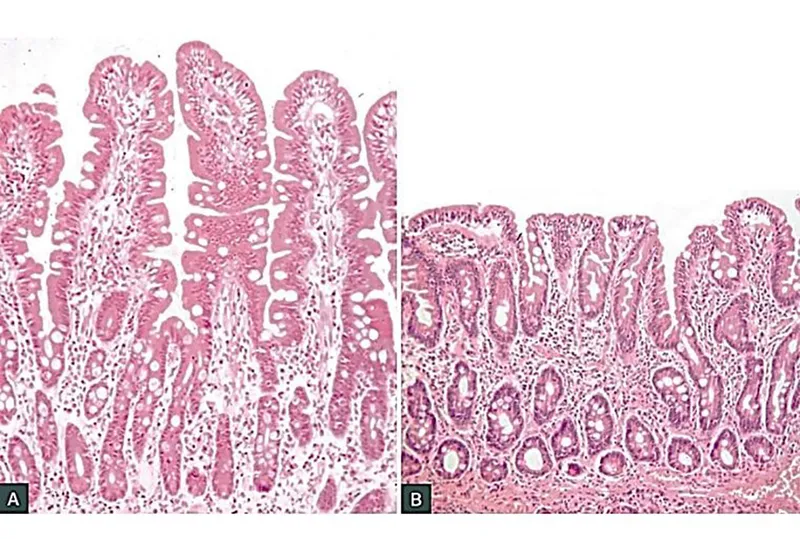
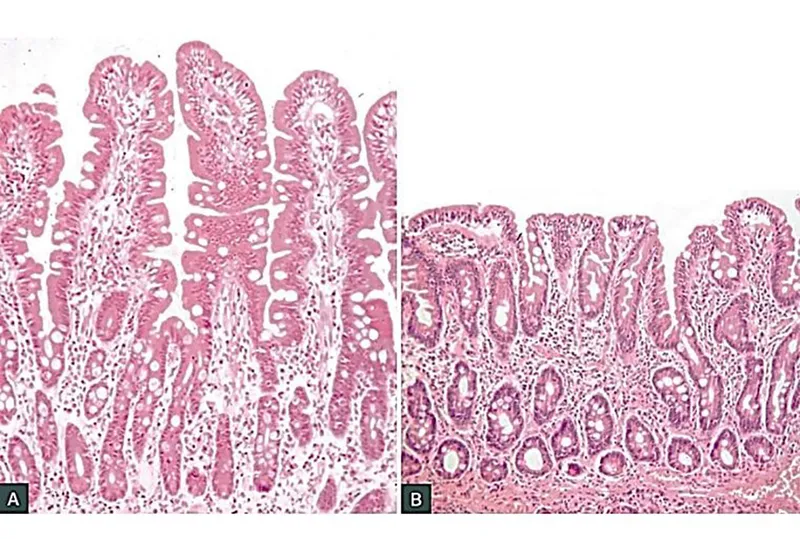
- Histopathology: Villous atrophy, crypt hyperplasia, and increased intraepithelial lymphocytes.
⭐ Dermatitis herpetiformis (a pruritic papulovesicular rash on extensor surfaces) is a specific skin manifestation.
- Treatment: Lifelong, strict gluten-free diet.
Key Syndromes - The Usual Suspects
-
Celiac Disease
- Autoimmune reaction to gluten (gliadin) in genetically susceptible individuals (HLA-DQ2/DQ8).
- Location: Primarily affects duodenum & proximal jejunum.
- Histology: Blunting/atrophy of villi, crypt hyperplasia, ↑ intraepithelial lymphocytes.
- Labs: ↑ IgA anti-tissue transglutaminase (tTG), anti-endomysial antibodies.
⭐ Associated with dermatitis herpetiformis, an intensely pruritic papulovesicular rash on extensor surfaces.
-
Tropical Sprue
- Occurs in residents of or visitors to tropical regions; likely infectious etiology.
- Affects entire small bowel; jejunum & ileum involvement leads to folate & B12 deficiency.
- Responds to antibiotics (e.g., tetracycline) and folate supplementation.
-
Whipple Disease
- Systemic infection with Tropheryma whipplei.
- Histology: Lamina propria filled with PAS-positive foamy macrophages.
- 📌 Mnemonic: Foamy Whipped cream in a CAN (Cardiac, Arthralgias, Neurologic symptoms).
Clinical Workup - Cracking the Code
- Initial Tests: Sudan stain or quantitative fecal fat (>7 g/day) to confirm steatorrhea.
- D-xylose Test: Differentiates pancreatic vs. mucosal causes.
⭐ Low urinary D-xylose points to a mucosal defect (e.g., celiac disease), as the intestine itself cannot absorb the monosaccharide. Normal levels suggest a pancreatic enzyme deficiency is the likely culprit.
High‑Yield Points - ⚡ Biggest Takeaways
- Celiac disease: Autoimmune, HLA-DQ2/DQ8-associated reaction to gluten causing villous atrophy.
- Whipple disease: Systemic infection (T. whipplei) with PAS-positive macrophages in lamina propria.
- Tropical sprue: Affects the entire small bowel (jejunum/ileum) and responds to antibiotics.
- Lactase deficiency: Results in osmotic diarrhea; diagnosed via hydrogen breath test.
- Pancreatic insufficiency: Causes steatorrhea and fat-soluble vitamin (A, D, E, K) deficiency.
- D-xylose test: Distinguishes mucosal damage (impaired absorption) from enzyme deficiency (normal absorption).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

