Thyroiditis Overview - The Gland on Fire
- Thyroiditis is inflammation of the thyroid gland, leading to transient or permanent dysfunction. It's classified by onset, duration, and the presence or absence of pain.
⭐ Subacute (de Quervain's) thyroiditis is the most common cause of a painful thyroid gland and often follows a viral upper respiratory infection.
Hashimoto's Thyroiditis - Autoimmune Attack
- Most common cause of hypothyroidism in iodine-sufficient areas.
- Pathogenesis: Autoimmune destruction of thyroid follicles.
- Genetic predisposition: HLA-DR3 & HLA-DR5.
- Key antibodies: Anti-thyroid peroxidase (anti-TPO) & anti-thyroglobulin (anti-Tg).
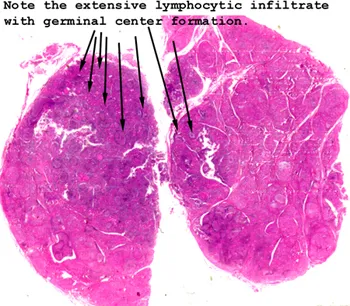
- Histology: Intense lymphoplasmacytic infiltrate with germinal centers, and Hurthle cells (enlarged eosinophilic follicular cells).
⭐ Increased risk of developing primary B-cell lymphoma of the thyroid.
- Clinical course: Initially may cause transient hyperthyroidism (hashitoxicosis) from follicle rupture, followed by progressive hypothyroidism.
Subacute Granulomatous Thyroiditis - de Quervain's Pain
- Often follows a viral upper respiratory infection.
- Primary Symptom: A very PAINFUL and tender thyroid gland; pain can radiate to the jaw or ear.
- Key Labs: Markedly ↑ ESR (often >100 mm/hr) and ↑ CRP.
- Clinical Course: Triphasic thyroid function:
- Transient hyperthyroidism (hormone release from damaged follicles).
- Followed by hypothyroidism.
- Spontaneous recovery to euthyroidism is common.
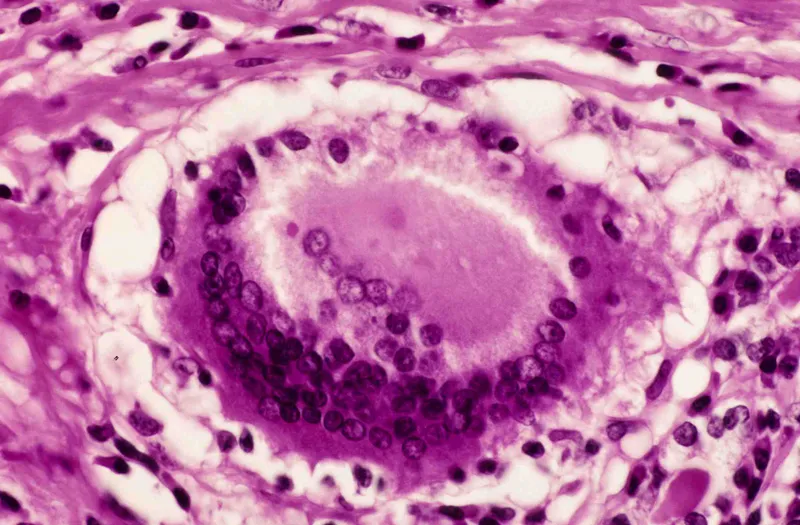
- Histology: Granulomatous inflammation with multinucleated giant cells.
⭐ Radioactive Iodine Uptake (RAIU) is dramatically decreased, typically <5%.
Rarer Forms - Rock-Hard & Silent
-
Riedel's Thyroiditis
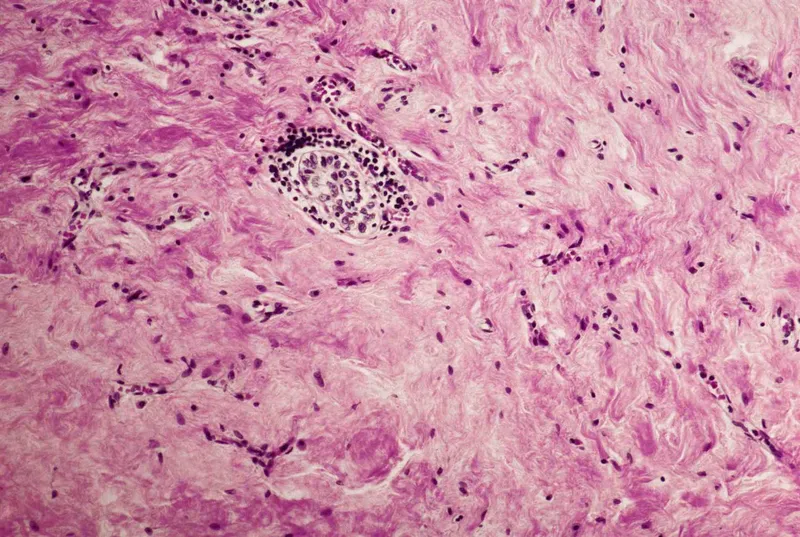
- An IgG4-related systemic disease causing intense fibrosis.
- Presents as a painless, "rock-hard," fixed goiter, mimicking malignancy.
- May compress local structures (e.g., trachea, esophagus).
- Patients are typically euthyroid.
-
Subacute Lymphocytic (Silent/Painless) Thyroiditis
- A self-limited variant of Hashimoto's, often occurring post-partum.
- Presents with a small, non-tender goiter.
- Brief hyperthyroid phase followed by hypothyroidism, then recovery.
⭐ Riedel's thyroiditis can be associated with IgG4-related fibrosis in other locations, such as retroperitoneal fibrosis.
Diagnostic Workup - Thyroid Detective
| Condition | Key Labs & Antibodies | RAIU Scan | Biopsy Buzzwords |
|---|---|---|---|
| Hashimoto's | ↑ TSH, ↓ T4 Anti-TPO, Anti-Tg Ab+ | Variable | Lymphocytic infiltrate, germinal centers, Hürthle cells |
| Subacute (de Quervain's) | ↓ TSH, ↑ T4 (early) ↑ ESR, CRP | ↓ (painful) | Granulomatous inflammation, multinucleated giant cells |
| Riedel's | Euthyroid/Hypo IgG4-related | ↓ ("cold") | Dense "rock-hard" fibrosis, fibrous tissue |
| Silent/Postpartum | Transient thyrotoxicosis then hypo | ↓ | Lymphocytic infiltrate (similar to Hashimoto's) |
⭐ Subacute (de Quervain's) thyroiditis is the most common cause of a painful thyroid gland.
High‑Yield Points - ⚡ Biggest Takeaways
- Hashimoto's thyroiditis: The most common cause of hypothyroidism in iodine-sufficient areas, marked by anti-TPO antibodies.
- Subacute (de Quervain) thyroiditis: Presents with a painful goiter, often following a viral infection.
- Riedel's thyroiditis: Characterized by a rock-hard, painless goiter from extensive fibrosis, mimicking malignancy.
- Postpartum thyroiditis: A self-limited condition occurring within 1 year of delivery.
- Subacute and postpartum types can cause transient hyperthyroidism followed by hypothyroidism.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

