Gestational Diabetes - Sweet Baby, Sour Mom
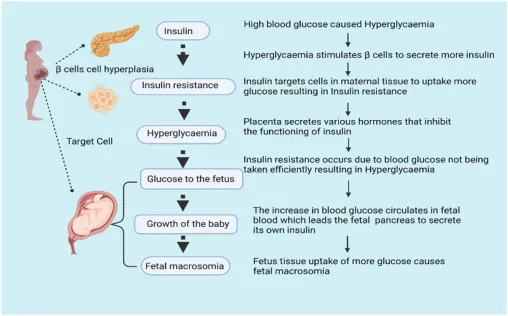
- Pathophysiology: Human placental lactogen (hPL) and other placental hormones ↑ insulin resistance in the mother.
- Screening & Diagnosis: Standard two-step approach.
- Maternal Risks: ↑ risk of preeclampsia, C-section, and future Type 2 DM.
- Fetal Risks: Macrosomia, neonatal hypoglycemia, polycythemia, respiratory distress.
⭐ High-Yield: Fetal macrosomia results from fetal hyperinsulinemia (insulin as a growth factor). After birth, persistent hyperinsulinemia with loss of maternal glucose supply causes profound neonatal hypoglycemia.
Thyroid Disorders - Bumps, Babies, & Butterflies
- Physiologic Changes: ↑ Estrogen → ↑ Thyroxine-binding globulin (TBG) → ↑ Total T4. hCG can weakly stimulate TSH receptors, causing transient hyperthyroidism.
- Maternal Hypothyroidism: Key risk is impaired fetal neurodevelopment (cretinism). Requires ↑ levothyroxine dose.
- Maternal Hyperthyroidism (Graves'):
- 📌 Propylthiouracil (PTU) for Primary (1st) trimester.
- Methimazole for 2nd/3rd trimesters to avoid PTU hepatotoxicity.
⭐ TSH-receptor antibodies (TSI) are IgG and can cross the placenta, causing fetal/neonatal thyrotoxicosis.
Preeclampsia & HELLP - When Pregnancy Gets Pressured
- Preeclampsia: New-onset hypertension (BP >140/90 mmHg) after 20 weeks gestation PLUS proteinuria or signs of end-organ damage.
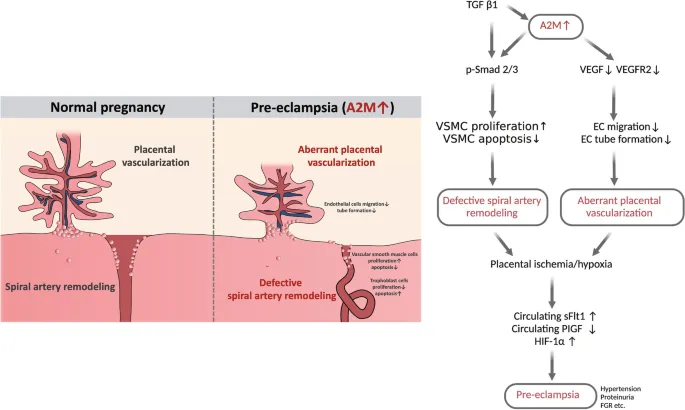
- Pathophysiology: Defective spiral artery remodeling → placental ischemia → release of anti-angiogenic factors (e.g., sFlt-1) → systemic endothelial dysfunction.
- HELLP Syndrome: A severe manifestation of preeclampsia.
- Hemolysis (schistocytes on smear, ↑LDH)
- Elevated Liver enzymes (AST, ALT)
- Low Platelets (<100,000/μL)
- Management:
- Definitive cure: Delivery of the placenta.
- Seizure prophylaxis: Magnesium sulfate (MgSO₄).
- BP control: Hydralazine, Labetalol, Nifedipine.
⭐ The definitive treatment for preeclampsia/HELLP syndrome is delivery of the fetus and placenta, which resolves the underlying pathology.
Pituitary & Adrenal Issues - The Other Endocrine Players
- Sheehan Syndrome: Postpartum pituitary necrosis due to severe hemorrhage & hypotension.
- Presents with failure to lactate (↓ prolactin), amenorrhea, adrenal insufficiency (↓ ACTH), and hypothyroidism (↓ TSH).
- Onset is often gradual.
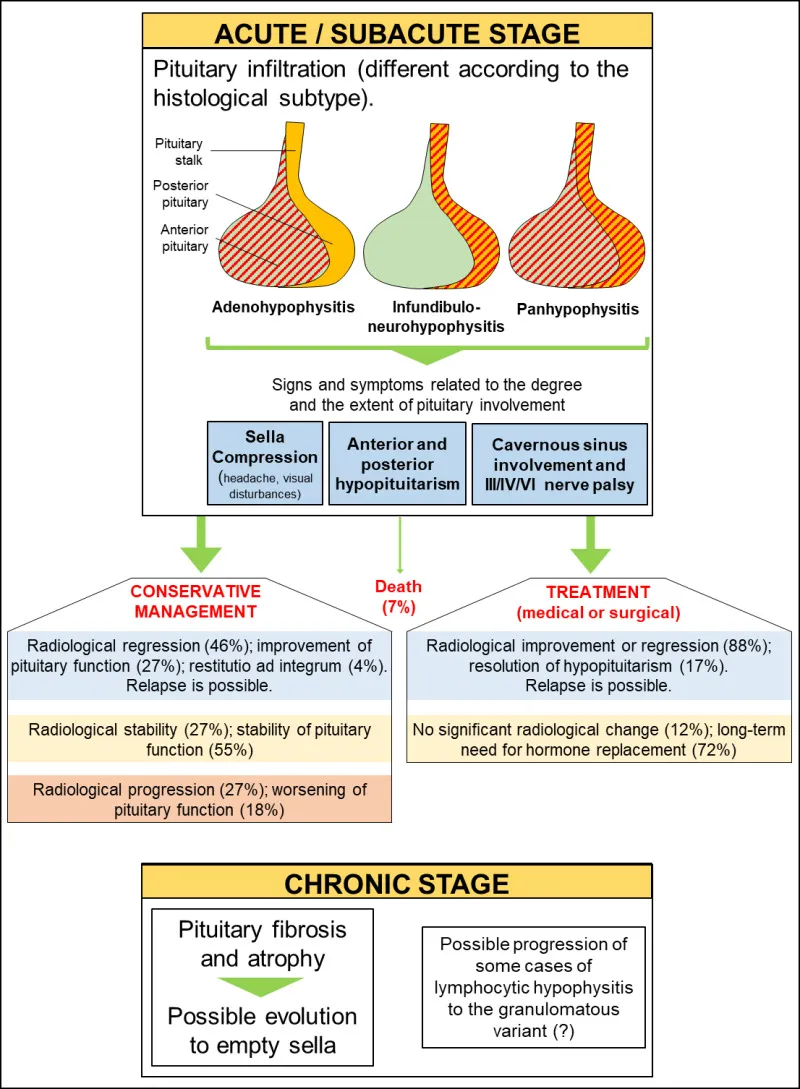
- Lymphocytic Hypophysitis: Autoimmune pituitary inflammation, usually in late pregnancy or postpartum.
- Can mimic a pituitary adenoma, causing headaches, visual defects, and hypopituitarism.
- Adrenal Insufficiency (Addison's): Requires increased glucocorticoid doses during pregnancy and stress-dose steroids for labor to prevent adrenal crisis.
⭐ Failure to lactate is the most common initial sign of Sheehan syndrome.
High‑Yield Points - ⚡ Biggest Takeaways
- Gestational diabetes is driven by hPL-induced insulin resistance; screen at 24-28 weeks.
- Maternal hyperglycemia → fetal hyperinsulinemia → macrosomia & neonatal hypoglycemia.
- hCG stimulates TSH receptors, raising total T4; free T4 and TSH levels remain normal.
- Graves' disease often improves during pregnancy; maternal anti-TSH receptor antibodies can cause fetal thyrotoxicosis.
- Postpartum thyroiditis presents as transient hyperthyroidism, often followed by a hypothyroid phase.
- Sheehan syndrome is postpartum pituitary necrosis causing failure to lactate and hypopituitarism.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

