Panniculitis - Fat Under Fire
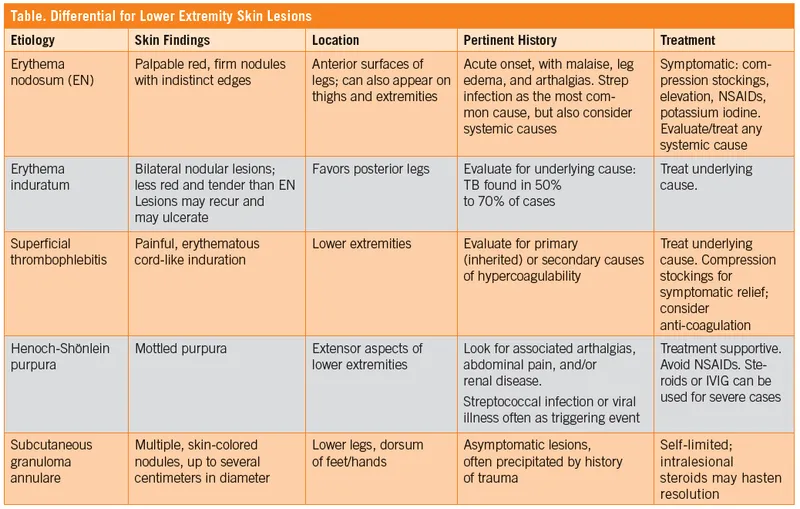
- Definition: Inflammation of subcutaneous fat (panniculus adiposus), presenting as deep, tender, erythematous nodules, typically on the lower extremities.
- Diagnosis: Requires a deep incisional or excisional biopsy for accurate histologic classification, which is crucial for determining the underlying cause and appropriate management.
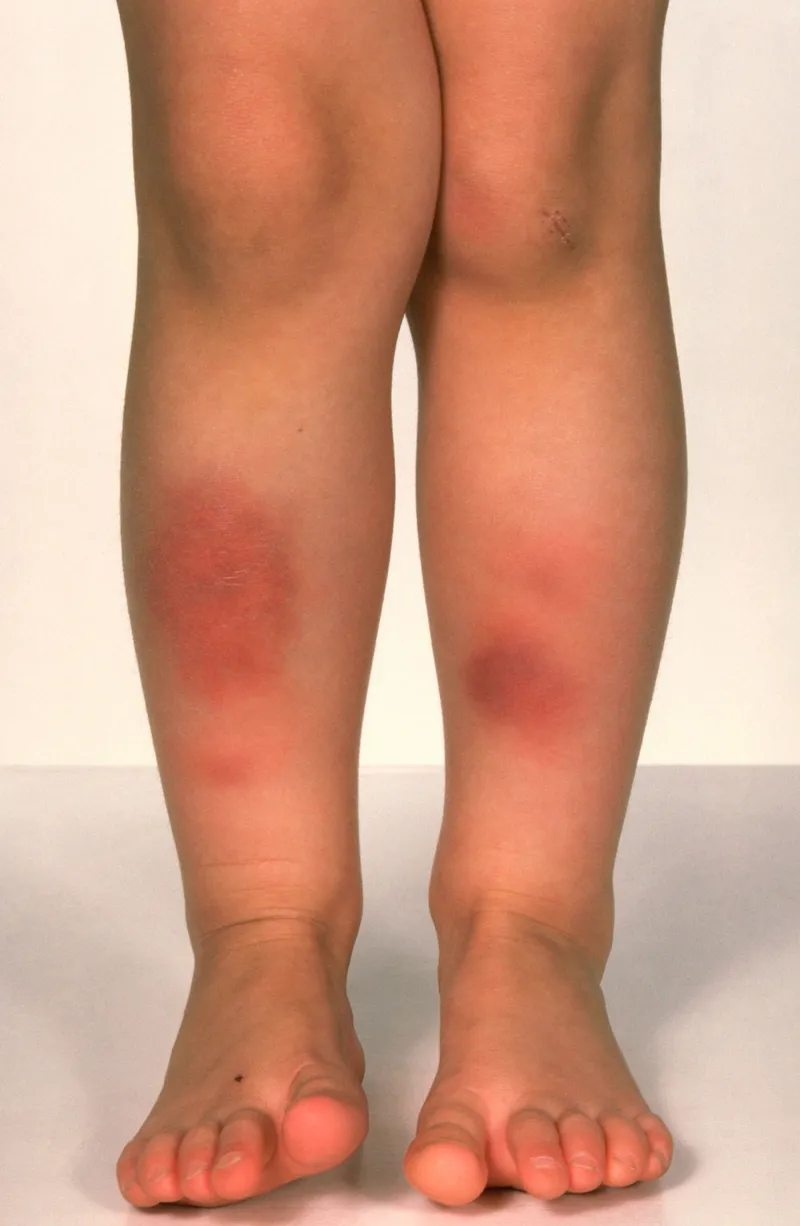
⭐ Erythema nodosum (septal, no vasculitis) is the most common form. It represents a delayed hypersensitivity reaction to various stimuli like infections (Strep), sarcoidosis, IBD, and drugs (OCPs).
Erythema Nodosum - Shins on Fire
- Pathophysiology: A delayed-type (Type IV) hypersensitivity reaction affecting the septa of subcutaneous fat.
- Clinical: Presents as tender, erythematous, non-ulcerated nodules, classically on the anterior shins. Fever and arthralgias are common.
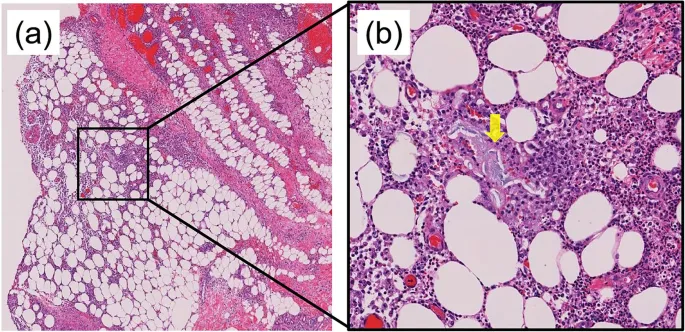
- Histology: Septal panniculitis without primary vasculitis. Early lesions show edema, hemorrhage, and neutrophils; later lesions have lymphocytes, histiocytes, and giant cells, including characteristic Miescher's radial granulomas.
- Associations:
- 📌 Mnemonic: ENjoys SODA
- Sarcoidosis / Streptococcal infection
- OCPs
- Drugs (sulfonamides)
- Autoimmune (e.g., IBD)
- 📌 Mnemonic: ENjoys SODA
⭐ In children, streptococcal infection is the most common trigger, whereas in adults, it's often idiopathic or linked to sarcoidosis.
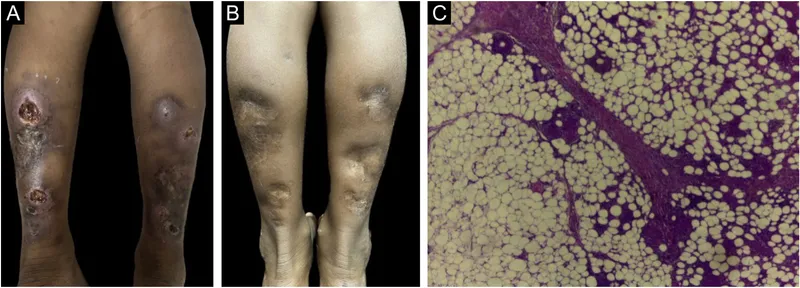
Erythema Induratum - Calf Ulcer Attack
- Pathophysiology: A mostly lobular panniculitis involving a T-cell mediated hypersensitivity reaction, often with vasculitis.
- Clinical Presentation:
- Tender, erythematous nodules primarily on the posterior calves.
- Characteristically ulcerate, drain, and heal with scarring, distinguishing it from erythema nodosum.
- Histology:
- Lobular or mixed septal-lobular panniculitis.
- Necrotizing vasculitis of small to medium-sized vessels within the fat lobules.
- Associations:
- Strongly associated with Mycobacterium tuberculosis (scrofuloderma).
- Also linked to other infections like Nocardia and hepatitis C.
⭐ When linked to tuberculosis, it's termed Bazin's disease. A positive PPD test or IGRA is a key diagnostic clue.
Other Types - The Unusual Suspects
- Alpha-1-Antitrypsin Deficiency: A lobular panniculitis with liquefactive necrosis, leading to oily discharge and ulceration. Diagnosis requires checking A1AT levels.
- Factitial Panniculitis: Self-induced by injecting foreign substances (e.g., oils, milk). Presents with bizarre, angular lesions. Histology reveals foreign material.
- Pancreatic Panniculitis: Lobular type associated with pancreatitis or pancreatic cancer.
⭐ Histology classically shows "ghost cells"-anucleated adipocytes with calcified walls from saponification.
High‑Yield Points - ⚡ Biggest Takeaways
- Erythema nodosum, the most common form, is a septal panniculitis without vasculitis, typically on the anterior shins.
- Erythema induratum is a lobular panniculitis with vasculitis, strongly associated with tuberculosis.
- Pancreatic panniculitis shows ghost-like fat cells from enzymatic fat necrosis due to pancreatitis or carcinoma.
- Alpha-1 antitrypsin deficiency can cause a neutrophilic lobular panniculitis.
- Diagnosis requires a deep excisional biopsy to adequately sample the subcutaneous fat.
- The key histologic distinction is septal versus lobular inflammation.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

