Basal Cell Carcinoma - The Pearly Peril
- Most common skin cancer. Locally invasive, very low metastatic potential.
- Risk Factors: Chronic sun exposure (UVB), fair skin, immunosuppression, xeroderma pigmentosum.
- Subtypes:
- Nodular: Most common. Pearly papule with telangiectasias.
- Superficial: Pink/red patch with fine scale.
- Morpheaform: Scar-like, indistinct borders, aggressive.
- Histology: Nests of basaloid cells in the dermis with peripheral palisading nuclei and stromal retraction.
⭐ Classic "rodent ulcer" describes central ulceration within a pearly, rolled border.
- Treatment: Mohs surgery for high-risk/facial lesions. Standard excision, curettage, or topical therapies for others.
Squamous Cell Carcinoma - Keratin's Rebellion
- Pathogenesis: Malignant proliferation of epidermal keratinocytes, invading the dermis. Often arises from a precursor lesion, actinic keratosis.
- Risk Factors: Chronic UVB exposure, immunosuppression (e.g., transplant recipients), chronic inflammation (e.g., burn scars, Marjolin's ulcer), arsenic, HPV.
- Clinical: Firm, scaling, erythematous papule or plaque; may ulcerate or bleed. Typically on sun-exposed areas like the face, lower lip, ears, and hands.
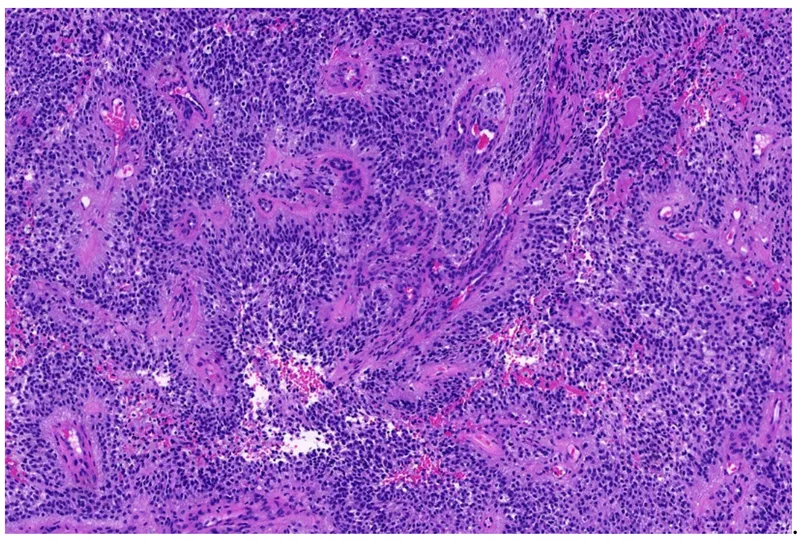
- Histology: Invasive cords/nests of atypical squamous cells with eosinophilic cytoplasm, large pleomorphic nuclei, and characteristic keratin pearls.
- Bowen's Disease: SCC in situ (full-thickness epidermal atypia).
⭐ SCC arising in non-sun-exposed sites, such as chronic wounds or burn scars (Marjolin's ulcer), has a higher metastatic potential.

Precursors & Mimics - The Warning Signs
-
Actinic Keratosis (AK)
- Premalignant lesion for SCC; rough, "sandpaper" feel.
- Found on sun-exposed skin (face, scalp, arms).
- Progression risk to SCC is low per lesion (<1%/year) but high per patient.

-
Bowen's Disease (SCC in situ)
- Full-thickness epidermal atypia without dermal invasion.
- Well-demarcated, scaly, erythematous patch or plaque.
-
Keratoacanthoma (KA)
- Rapidly growing "volcano-like" nodule with a central keratin plug.
- Often spontaneously involutes; treated as well-differentiated SCC.
⭐ Leser-Trélat Sign: Sudden eruption of multiple seborrheic keratoses can be a sign of underlying internal malignancy, most commonly gastric adenocarcinoma.
Rarer Tumors - The Odd Ones Out
- Merkel Cell Carcinoma: Aggressive neuroendocrine tumor, often on sun-exposed skin. Associated with Merkel cell polyomavirus. Histology shows small blue cells; stains for synaptophysin & CK-20.
- Dermatofibrosarcoma Protuberans (DFSP): Locally aggressive, slow-growing spindle cell tumor. Histology: storiform (pinwheel) pattern, CD34 positive.
- Sebaceous Carcinoma: Arises from sebaceous glands, typically on the eyelid. Associated with Muir-Torre syndrome (Lynch syndrome variant).
⭐ Merkel cell carcinoma presents as a rapidly growing, painless, red-to-violaceous nodule (AEIOU mnemonic: Asymptomatic, Expanding rapidly, Immunosuppression, Older age, UV-exposed site).
High‑Yield Points - ⚡ Biggest Takeaways
- Basal Cell Carcinoma (BCC) is the most common skin cancer, presenting as a pearly papule with telangiectasias and showing peripheral palisading on histology.
- Squamous Cell Carcinoma (SCC) is linked to UV exposure and immunosuppression; histology reveals characteristic keratin pearls.
- Actinic keratosis is the most common premalignant lesion for SCC.
- Keratoacanthoma is a rapidly growing, volcano-like SCC variant that can spontaneously regress.
- Marjolin's ulcer is an aggressive SCC arising in chronic wounds or burn scars.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

