Keratoses - Stuck-On Old Warts
- Seborrheic Keratosis (SK): Common, benign epidermal tumors in older adults.
- Clinical: "Stuck-on," waxy, well-demarcated papules/plaques; color varies (tan to black).
- Histology: Exophytic proliferation of basaloid cells, keratin-filled invaginations (horn cysts), and pseudohorn cysts.
- Variants:
- Dermatosis Papulosa Nigra (DPN): Multiple small, hyperpigmented papules on the face/neck of darker-skinned individuals (e.g., Fitz IV-VI).
- Stucco Keratosis: Small, white-gray papules on lower extremities; "stuck-on" dry appearance.
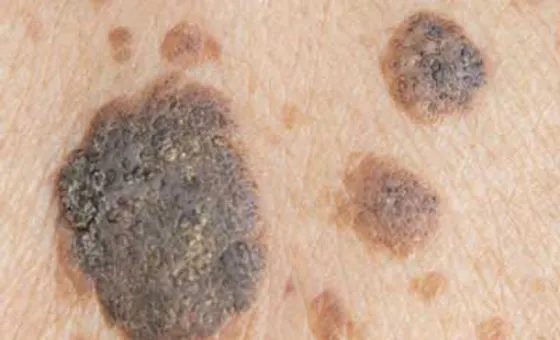
⭐ The sudden eruptive appearance of multiple seborrheic keratoses, known as the sign of Leser-Trélat, can be a cutaneous marker for internal malignancy (e.g., gastric adenocarcinoma).
Acanthosis Nigricans - Velvet Clues Within
- Pathophysiology: A disorder of keratinocyte proliferation, often driven by ↑ insulin levels or fibroblast growth factor receptor 3 (FGFR3) activation. Insulin binds to IGF-1 receptors on keratinocytes, stimulating their growth.
- Presentation: Symmetric, velvety, hyperpigmented plaques.
- Locations: Commonly found in flexural areas like the axillae, groin, and posterior neck.

- Types:
- Benign: Associated with obesity, insulin resistance, and endocrine disorders (e.g., PCOS, diabetes).
- Malignant: A paraneoplastic sign, often linked to underlying GI malignancies (especially gastric adenocarcinoma).
⭐ High-Yield: Sudden, explosive onset of acanthosis nigricans in an older, non-obese patient is a red flag for an internal malignancy.
Keratinocyte Tumors - Sun's Angry Children
- Sun-induced epithelial lesions with malignant potential, often on sun-exposed skin (face, hands). 📌 Mnemonic: Actinic Keratosis for Atypical Keratinocytes.
| Feature | Actinic Keratosis (AK) | Keratoacanthoma (KA) |
|---|---|---|
| Clinical | Sandpaper-like, erythematous patch/papule | Rapidly growing, dome-shaped nodule with central keratin plug |
| Progression | Premalignant; <1%/year risk of SCC | Often regresses; variant of well-differentiated SCC |
| Histology | Basal cell atypia, parakeratosis, solar elastosis | Symmetrical, crateriform; glassy eosinophilic keratinocytes |
⭐ Keratoacanthoma's classic presentation is a rapidly growing "volcano-like" nodule with a central keratin-filled crater, which may spontaneously involute.
Adnexal Neoplasms - Sweat & Hair Glitches
Benign tumors from sweat glands or hair follicles, often presenting as skin-colored papules.
| Tumor | Origin | Clinical Presentation | Histology |
|---|---|---|---|
| Syringoma | Eccrine | Multiple, small periorbital papules | Ducts with "tadpole" or comma shapes |
| Cylindroma | Apocrine | Scalp/forehead nodules ("Turban tumor") | "Jigsaw puzzle" pattern of basaloid islands |
| Trichoepithelioma | Follicular | Flesh-colored facial papules | Basaloid islands, abortive follicles, horn cysts |
⭐ Brooke-Spiegler syndrome is an autosomal dominant condition featuring multiple cylindromas and trichoepitheliomas, caused by a CYLD gene mutation.
High‑Yield Points - ⚡ Biggest Takeaways
- Seborrheic keratosis presents as waxy, "stuck-on" papules; the Leser-Trélat sign (sudden eruptive onset) suggests underlying GI adenocarcinoma.
- Acanthosis nigricans manifests as velvety, hyperpigmented plaques in flexural areas, strongly associated with insulin resistance or malignancy.
- Keratoacanthoma is a rapidly growing, dome-shaped nodule with a central keratin-filled crater that may spontaneously resolve.
- Epidermal inclusion cysts are common subcutaneous nodules with a central punctum, containing degenerating keratin.
- Cylindromas are scalp "turban tumors" showing a "jigsaw puzzle" pattern of basaloid islands on histology.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

