HHD Pathophysiology - Pressure Overload
- Mechanism: Chronic ↑ afterload (e.g., systemic HTN, aortic stenosis) forces the left ventricle (LV) to generate higher pressures.
- Cellular Adaptation: Myocytes enlarge (hypertrophy) by adding new sarcomeres in parallel.
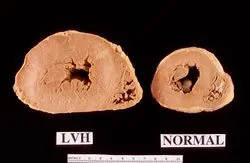
- This results in concentric hypertrophy → ↑ LV wall thickness, often with a ↓ in chamber radius.
- Physics: Compensatory hypertrophy normalizes wall stress per Laplace’s Law ($Wall Stress = (P \times r) / (2h)$) by increasing wall thickness (h).
⭐ The earliest manifestation of HHD is typically diastolic dysfunction, leading to Heart Failure with preserved Ejection Fraction (HFpEF). Systolic failure (HFrEF) is a late complication.
Systemic (Left) HHD - The Body's Burden
- Pathogenesis: Chronic systemic hypertension imposes a pressure overload (↑ afterload) on the left ventricle (LV), forcing it to work harder.
- LV Adaptation & Failure: The ventricle adapts via concentric hypertrophy (thickened wall) to normalize wall stress. This eventually leads to:
- Stiff LV → Impaired diastolic filling (diastolic dysfunction).
- ↑ Myocardial O₂ demand → Susceptibility to ischemia.
- Left atrial enlargement → Risk of atrial fibrillation.
- Morphology & Dx:
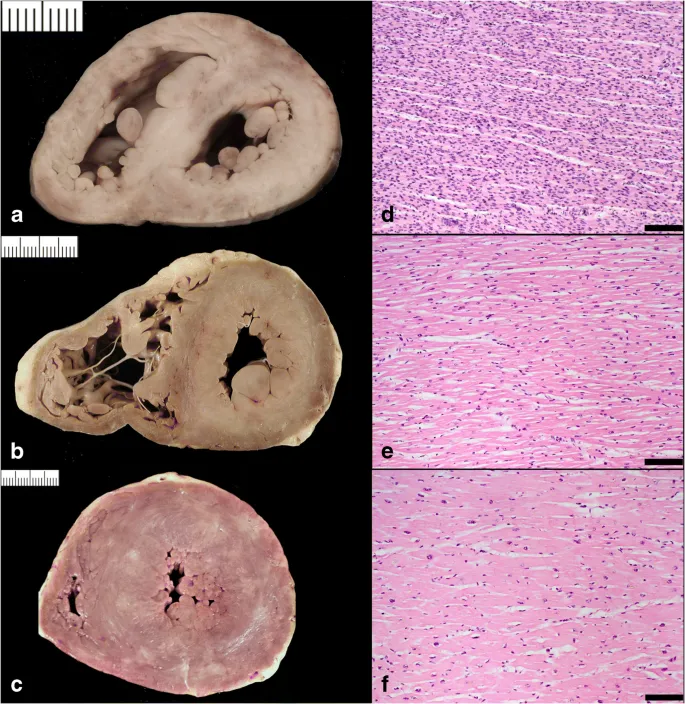
- Gross: Symmetrically thickened LV wall (>1.2 cm), ↑ heart weight.
- Micro: Enlarged myocytes with "boxcar" nuclei; interstitial fibrosis.
- ECG: May show LVH criteria (e.g., Sokolow-Lyon: S in V1 + R in V5/V6 > 35 mm).
⭐ The earliest manifestation is often diastolic dysfunction with preserved ejection fraction (HFpEF), as the stiff, hypertrophied ventricle cannot relax and fill properly.
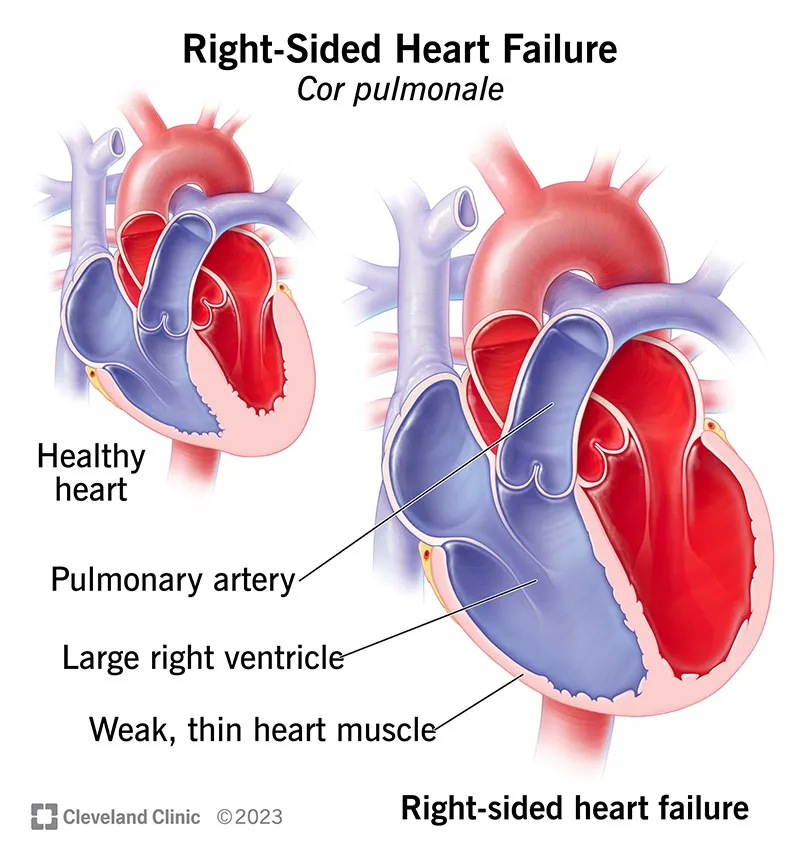
Pulmonary (Right) HHD - Cor Pulmonale
- Definition: Right ventricular (RV) hypertrophy and/or dilation resulting from pulmonary hypertension (PH) caused by diseases of the lung parenchyma or vasculature.
- Pathophysiology Flow:
- Common Causes:
- COPD (most frequent)
- Interstitial lung disease
- Chronic thromboembolic disease (CTEPH)
- Obstructive sleep apnea
- Clinical Findings:
- Symptoms of underlying lung disease + signs of right heart failure (JVD, peripheral edema, hepatomegaly).
- Loud P2, tricuspid regurgitation murmur.
- Diagnosis:
- Echo: Shows RVH, estimates pulmonary artery pressure.
- Right Heart Cath: Gold standard to confirm PH.
⭐ The most common cause of right-sided heart failure is left-sided heart failure. Cor pulmonale is specifically right-sided failure due to lung pathology.
HHD Morphology - Sizing Up Damage
- Systemic (Left) HHD:
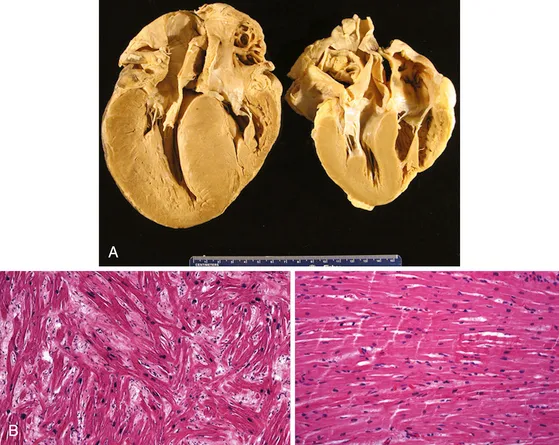
- Gross: Symmetrical, concentric left ventricular hypertrophy (LVH) without dilation initially. ↑ heart weight.
- Wall thickness can exceed 2.0 cm.
- Micro: Enlarged cardiomyocytes with prominent, hyperchromatic "boxcar" nuclei.
- Interstitial fibrosis develops over time.
- Pulmonary (Right) HHD / Cor Pulmonale:
- Gross: Right ventricular hypertrophy and dilation, often with wall thickness >1.0 cm.
⭐ A stiff, non-compliant LV from chronic hypertrophy leads to impaired diastolic filling, often manifesting as a prominent S4 heart sound.
High‑Yield Points - ⚡ Biggest Takeaways
- Systemic hypertension is the fundamental cause, creating pressure overload on the left ventricle.
- The heart adapts via concentric left ventricular hypertrophy (LVH).
- Histology classically shows enlarged myocytes with prominent "boxcar" nuclei.
- Clinically, it first manifests as diastolic dysfunction (HFpEF).
- An S4 gallop is a common auscultatory finding.
- Uncontrolled, it can progress to systolic dysfunction and overt heart failure.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

