Basics - The Great Dilations
- Aneurysm: Localized abnormal dilation of a blood vessel.
- True Aneurysm: Involves all three layers of the vessel wall (intima, media, adventitia).
- Saccular: Spherical outpouching (e.g., berry aneurysm).
- Fusiform: Circumferential, spindle-shaped dilation.
- False Aneurysm (Pseudoaneurysm): A breach in the vessel wall leading to an extravascular hematoma that communicates with the lumen.
- True Aneurysm: Involves all three layers of the vessel wall (intima, media, adventitia).
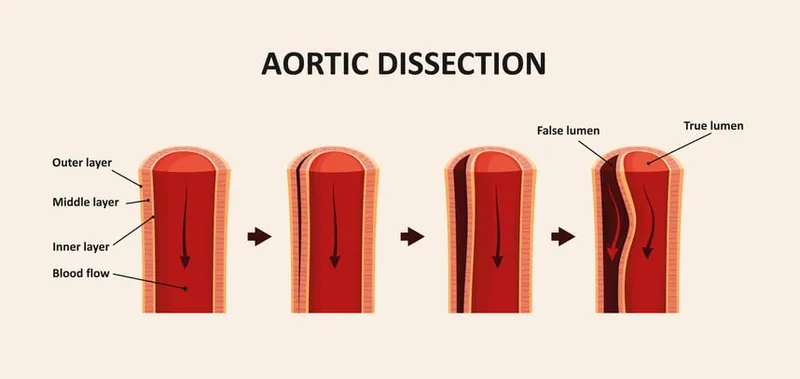
- Dissection: Blood enters the arterial wall itself, splitting the laminar planes of the media to form a blood-filled channel.
⭐ Hypertension is the single most important predisposing factor for aortic dissection.
📌 Primary Pathogenesis: Aneurysm → Atherosclerosis-induced wall weakening. Dissection → Chronic hypertension causing medial degeneration.
Abdominal Aortic Aneurysm (AAA) - Belly's Ballooning Bomb
- Patho: Atherosclerosis-driven chronic inflammation → ↑ Matrix Metalloproteinases (MMPs) → elastin/collagen degradation → aortic wall weakening & dilation.
- Risks: 📌 Smoking, Male, Age >60, Strong family hx, Hypertension. Smoking is the #1 modifiable risk factor.
- Presentation: Mostly asymptomatic. Classic triad for rupture: hypotension, pulsatile abdominal mass, and severe back/flank pain.
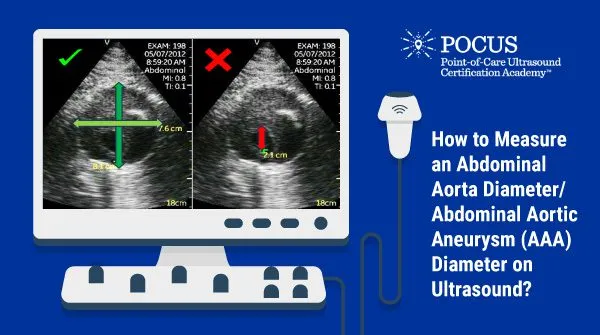
- Dx: Ultrasound for screening, initial diagnosis, and monitoring size. CT angiography for surgical planning.
- Rx:
- Monitor if < 5.5 cm.
- Elective repair if > 5.5 cm, growing > 0.5 cm/6 mo, or symptomatic.
⭐ Exam Favorite: Most AAAs occur infrarenally (below the renal arteries).
Aortic Dissection - The Great Divide
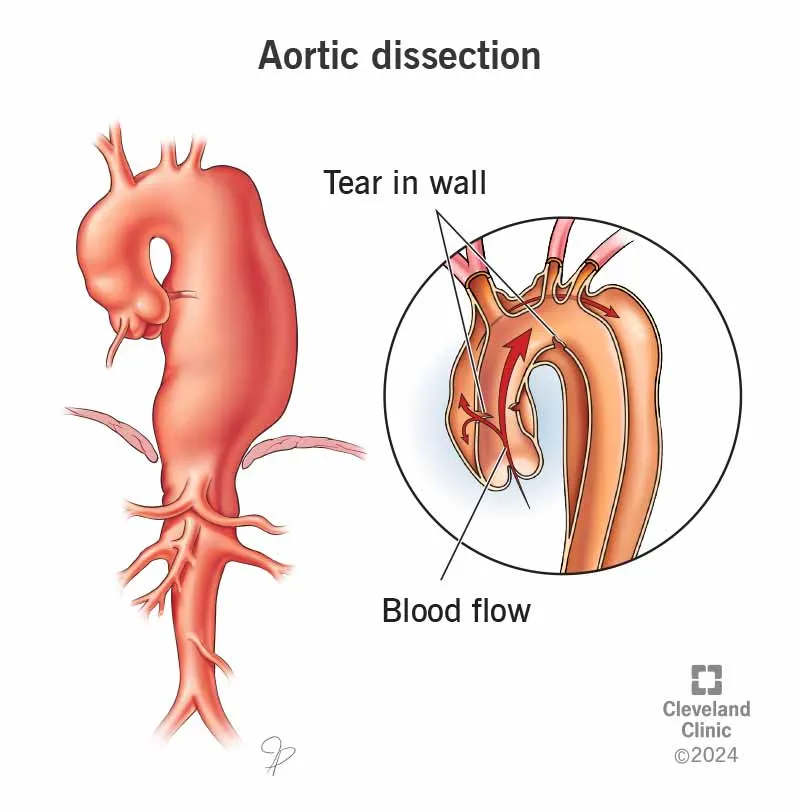
- Pathophysiology: A tear in the aortic intima allows blood to dissect through the media, creating a false lumen. Primarily driven by hypertension.
- Risk Factors: Chronic hypertension (most common), Marfan syndrome, Ehlers-Danlos, bicuspid aortic valve, trauma.
- Clinical Presentation: Sudden, severe "tearing" or "ripping" chest pain radiating to the back. May present with syncope, stroke, or MI.
- Asymmetric BP (>20 mmHg difference) or pulses between arms.
⭐ A blood pressure differential of >20 mmHg between arms is a highly specific sign for aortic dissection.
- Management:
- Stanford A (Proximal): Surgical emergency.
- Stanford B (Distal): Medical management (IV beta-blockers, e.g., labetalol) unless complicated (malperfusion, rupture).
Other Aneurysms - Thoracic & Berry Tales
-
Thoracic Aortic Aneurysm (TAA)
- Etiology: Atherosclerosis, cystic medial degeneration (e.g., Marfan syndrome), or tertiary syphilis (obliterative endarteritis of vasa vasorum → "tree bark" aorta).
- Clinical: Often asymptomatic; may cause respiratory or esophageal symptoms.
-
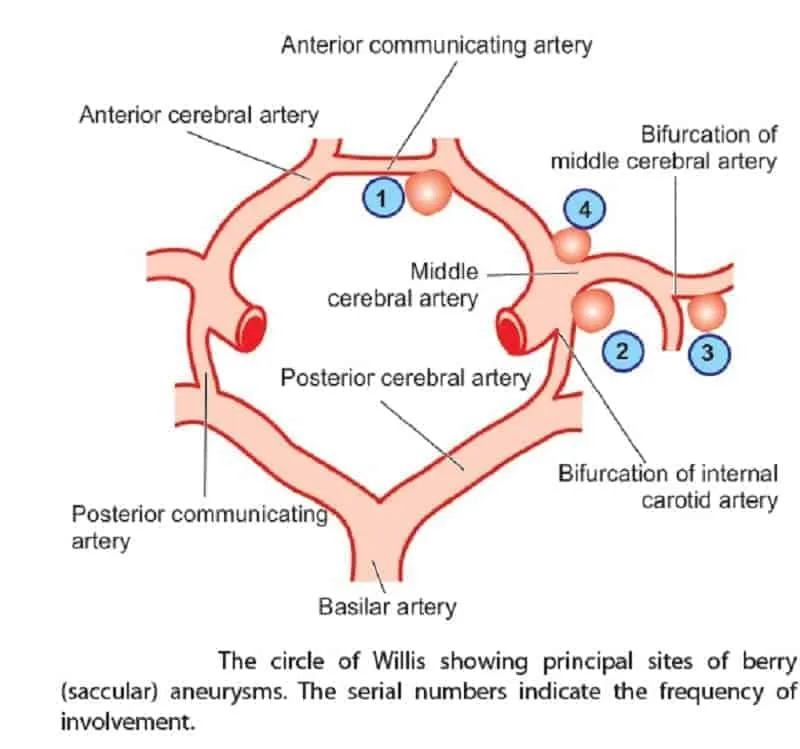
Berry (Saccular) Aneurysm
- Location: Occur at arterial branch points in the Circle of Willis; anterior communicating artery is most common.
- Associations: ADPKD, Ehlers-Danlos, Marfan syndrome.
- Rupture: Leads to subarachnoid hemorrhage (SAH).
⭐ A ruptured berry aneurysm classically presents as a sudden, severe "worst headache of my life."
High‑Yield Points - ⚡ Biggest Takeaways
- Abdominal Aortic Aneurysm (AAA), the most common true aneurysm, is linked to atherosclerosis and is typically infrarenal. Rupture triad: hypotension, pulsatile mass, flank pain.
- Aortic dissection is driven by hypertension and presents as tearing chest pain radiating to the back. Marfan syndrome is a key risk factor in the young.
- Tertiary syphilis classically causes Thoracic Aortic Aneurysm (TAA) by disrupting the vasa vasorum.
- Berry aneurysms are associated with ADPKD and risk subarachnoid hemorrhage.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

