Physiology & Definition - The Dilution Effect
-
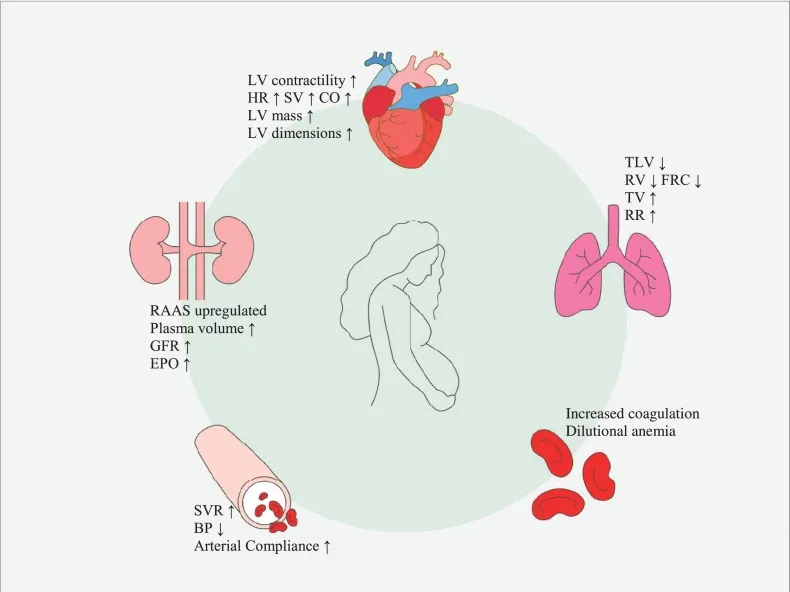
Pregnancy causes a greater expansion of plasma volume (↑ ~50%) compared to red blood cell (RBC) mass (↑ ~25-30%).
-
This disproportionate increase results in hemodilution, a physiologic decrease in hemoglobin (Hb) and hematocrit (Hct).
-
Anemia Thresholds (CDC):
- 1st Trimester: Hb < 11 g/dL
- 2nd Trimester: Hb < 10.5 g/dL
- 3rd Trimester: Hb < 11 g/dL
⭐ The nadir of physiologic anemia occurs in the late second trimester, coinciding with peak plasma volume.
Etiology & Diagnosis - Finding the Cause
- Initial Workup: Start with a Complete Blood Count (CBC).
- Anemia: Hemoglobin <11 g/dL (1st/3rd trimester) or <10.5 g/dL (2nd trimester).
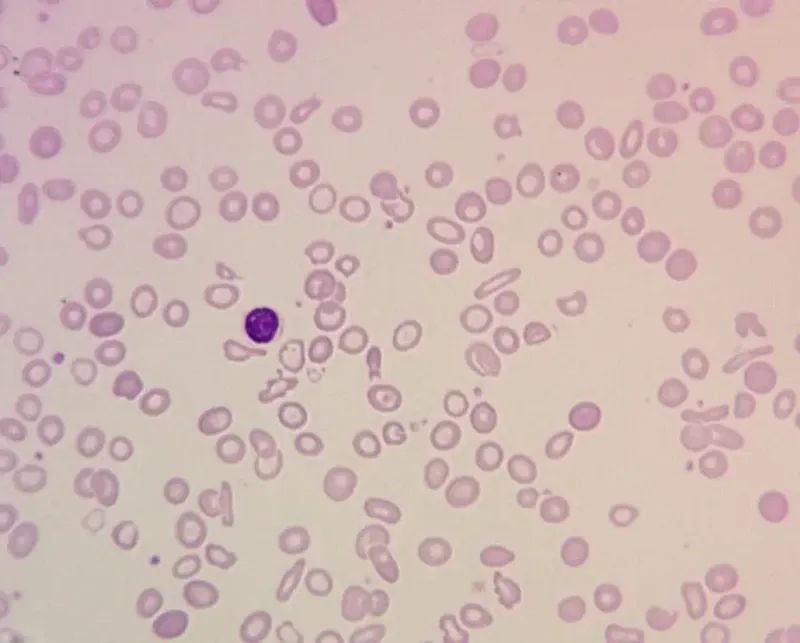
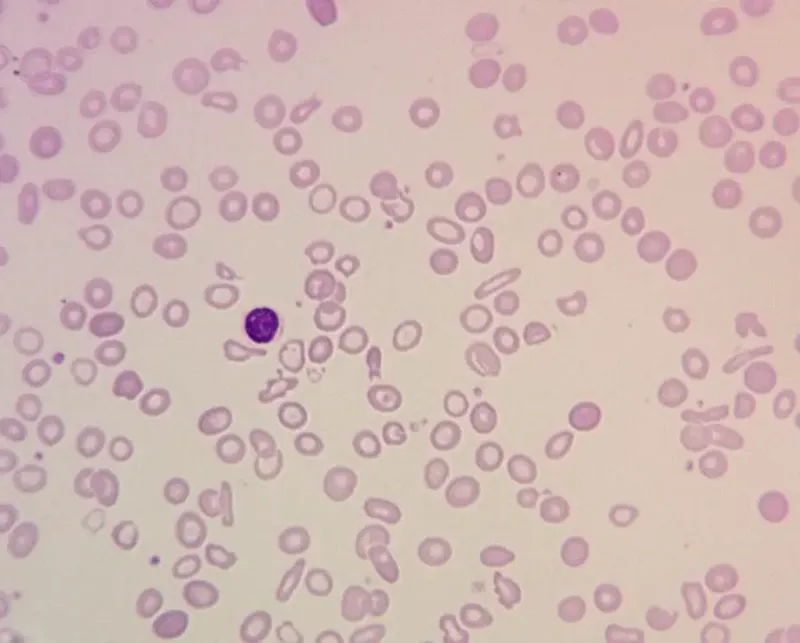
- Classification by MCV:
- Microcytic (MCV <80 fL): Most common type.
- Iron Deficiency Anemia (IDA): Check iron studies (↓ Ferritin, ↑ TIBC).
- Thalassemia: Hemoglobin electrophoresis.
- Normocytic (MCV 80-100 fL):
- Physiologic hemodilution, anemia of chronic disease.
- Macrocytic (MCV >100 fL):
- Folate or Vitamin B12 deficiency.
- Microcytic (MCV <80 fL): Most common type.
⭐ Serum ferritin is the most sensitive and specific test for iron deficiency in pregnancy; a level <30 ng/mL is diagnostic.
Screening & Workup - The Rightful Algorithm
- Universal Screening: CBC at the initial prenatal visit & repeated at 24-28 weeks.
- Anemia Thresholds:
- 1st & 3rd Trimesters: Hb < 11 g/dL
- 2nd Trimester: Hb < 10.5 g/dL
⭐ High-Yield: Serum ferritin is the most sensitive and specific test for iron deficiency. A level < 30 ng/mL confirms iron deficiency anemia in pregnancy.
Management - Boosting the Blood
- Iron Deficiency Anemia (IDA):
- First-line: Oral ferrous sulfate (325 mg daily).
- Take with Vitamin C to ↑ absorption.
- IV iron for malabsorption, PO intolerance, or severe anemia near term.
- Folate/B12 Deficiency: Replete the deficient vitamin.
- Packed RBC Transfusion: For Hgb < 7 g/dL, hemodynamic instability, or acute hemorrhage.
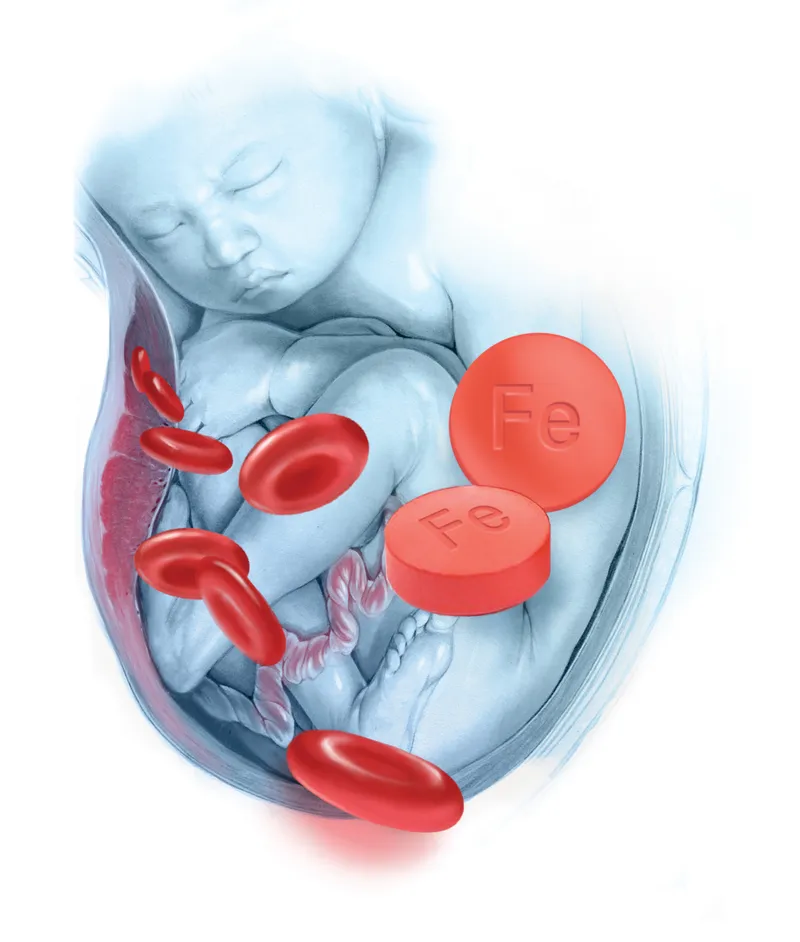
⭐ Fetal iron uptake is preserved even in severe maternal deficiency; the fetus effectively acts as an iron parasite.
Complications - Risks for Two
- Maternal Risks:
- Impaired cardiac function → high-output failure (if Hb < 6 g/dL)
- Preeclampsia
- ↑ Postpartum hemorrhage (PPH) & infection risk
- Poor tolerance to blood loss at delivery
- Fetal & Neonatal Risks:
- Low birth weight (LBW) & IUGR
- Preterm delivery
- Intrauterine fetal demise (IUFD)
- Lower iron stores → neonatal anemia
⭐ Maternal iron deficiency anemia, especially in the first two trimesters, is associated with an increased risk of autism spectrum disorder, ADHD, and intellectual disability in the child.
High‑Yield Points - ⚡ Biggest Takeaways
- Physiologic anemia of pregnancy is the most common type, resulting from hemodilution (plasma volume ↑ > RBC mass ↑).
- Iron deficiency is the most common pathologic cause; screen with a CBC at the first prenatal visit and again at 24-28 weeks.
- Diagnostic thresholds: Hb <11 g/dL in the 1st/3rd trimesters, and <10.5 g/dL in the 2nd.
- Low serum ferritin is the most sensitive and specific test for iron deficiency.
- Treat with oral ferrous sulfate; parenteral iron is reserved for severe cases or malabsorption.
- Folate deficiency causes megaloblastic anemia and increases the risk of neural tube defects.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

