Overview & Risk Factors - The Dangling Danger
- Obstetric Emergency: Umbilical cord descends ahead of the presenting fetal part, risking compression & fetal hypoxia.
- Core Problem: Anything preventing the fetal presenting part from snugly engaging in the pelvis after membrane rupture.
- Key Risk Factors:
- Fetal: Malpresentation (breech, transverse), prematurity, multiple gestation (2nd twin).
- Uterine/Pelvic: Polyhydramnios, unengaged presenting part.
- Iatrogenic: Artificial rupture of membranes (AROM) with a high station.
⭐ High-Yield: The most common cause is iatrogenic, from artificial rupture of membranes (AROM) when the fetal head is high and not engaged in the pelvis.
Clinical Presentation & Diagnosis - Code Blue Cord
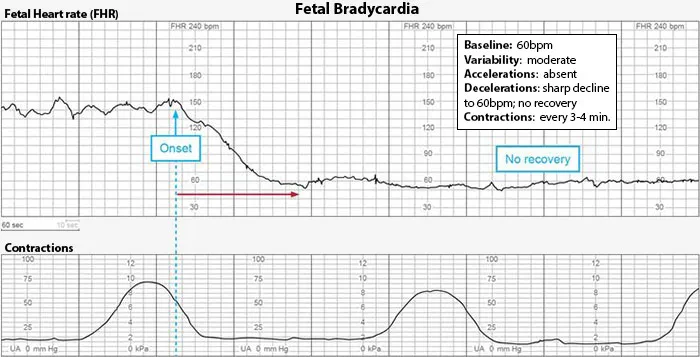
- Hallmark Event: Sudden, severe fetal heart rate (FHR) changes immediately following rupture of membranes (ROM), either spontaneous or artificial.
- Fetal Monitoring:
- Abrupt, prolonged fetal bradycardia (e.g., <110 bpm for >2 min).
- Severe, recurrent variable decelerations.
- Definitive Diagnosis:
- Made by direct sterile vaginal examination (SVE).
- Palpation of a pulsating, rope-like structure (the umbilical cord) in the vagina or at the cervical os, ahead of the fetal presenting part.
⭐ The most common initial sign is a sudden, severe fetal bradycardia or the onset of severe, recurrent variable decelerations on fetal monitoring, especially after membrane rupture.
Management - All Hands on Deck!
Immediate bedside actions to relieve cord compression while preparing for delivery.
- Call for help! (Anesthesiology, NICU, OR staff).
- Manually elevate the presenting part with a sterile-gloved hand. Keep hand in place until delivery.
- Reposition mother: Knee-chest or deep Trendelenburg position.
- Administer tocolytic (e.g., terbutaline 0.25 mg SC) to ↓ uterine contractions.
- Discontinue oxytocin if being administered.
⭐ Pearl: The single most important initial step is to manually lift the fetal presenting part off the umbilical cord to restore fetal blood flow. This is a life-saving maneuver.
High‑Yield Points - ⚡ Biggest Takeaways
- Umbilical cord prolapse is an obstetric emergency where the cord descends below the fetal presenting part.
- It causes cord compression, leading to fetal hypoxia, anoxia, and potential demise.
- The classic sign is sudden, severe fetal bradycardia or deep variable decelerations, typically after rupture of membranes.
- Key risk factors include malpresentation (e.g., breech), an unengaged presenting part, and polyhydramnios.
- Immediate management involves manually elevating the fetal head and placing the mother in the knee-chest position.
- Emergency cesarean section is the definitive treatment.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

