Normal Labor - The Ideal Blueprint
- The 3 Ps: Labor progression is governed by Power (uterine contractions), Passenger (fetus), and Passage (pelvis).
- Stage 1 (Dilation): Onset to 10 cm.
- Latent Phase: 0 to <6 cm. Gradual, variable length.
- Active Phase: ≥6 cm. Dilation: ≥1.2 cm/hr (nullipara), ≥1.5 cm/hr (multipara).
- Stage 2 (Expulsion): 10 cm to delivery. <3 hrs (nullipara), <2 hrs (multipara). Add 1 hr for epidural.
- Stage 3 (Placental): Delivery of infant to placenta. <30 min.
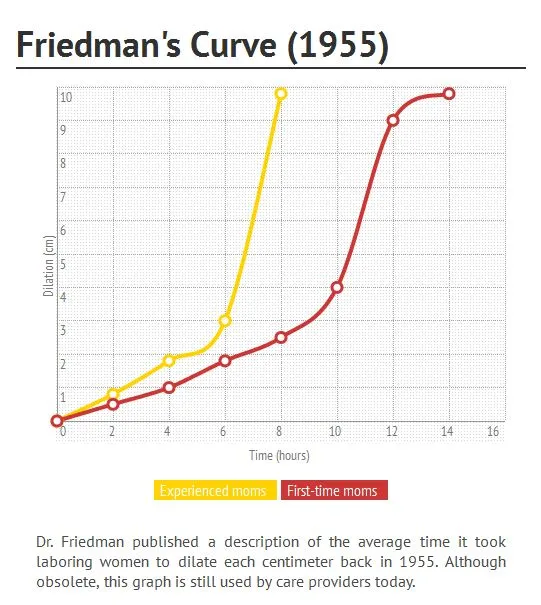
⭐ The definition of active labor shifted from 4 cm to 6 cm dilation, a critical threshold for diagnosing labor abnormalities.
Labor Dystocia - The 3 'P's Problem
📌 The "3 P's" framework helps diagnose the cause of abnormal labor, or dystocia.
- Power (Uterine Contractions): Inadequate strength or frequency.
- Defined as <200 Montevideo Units (MVUs) over 10 minutes.
- Management: Oxytocin augmentation.
- Passenger (Fetus): Issues with the fetus.
- Size: Macrosomia (birth weight >4000-4500 g).
- Presentation/Position: Breech, face, brow, transverse lie, occiput posterior.
- Anomalies: e.g., hydrocephalus.
- Passage (Pelvis/Birth Canal): Anatomic limitations.
- Pelvic Shape: Android or platypelloid pelvis.
- Cephalopelvic Disproportion (CPD): Mismatch between fetal head and maternal pelvis.
- Soft Tissue: Low-lying fibroids, cervical stenosis.
⭐ The most common cause of labor arrest in the first stage is inadequate uterine contractions (Power).
Precipitous Labor - The Express Lane
- Definition: Expulsion of the fetus in < 3 hours from the onset of regular, painful contractions.
- Risk Factors:
- High parity (multigravida)
- History of prior precipitous labor
- Cocaine abuse
- Pathophysiology: Abnormally strong uterine contractions with low resistance from the birth canal.
- Complications:
- Maternal: Uterine atony → PPH, extensive lacerations (cervical, vaginal), amniotic fluid embolism.
- Fetal: Hypoxia, intracranial hemorrhage, nerve injury (e.g., Erb's palsy).
⭐ High-Yield: The most significant maternal risk is postpartum hemorrhage (PPH) due to uterine atony from the overstimulated, exhausted myometrium.
Management Strategies - Course Correction
- Conservative: Maternal repositioning, pain management, and observation.
- Amniotomy (AROM): May enhance progress if membranes are intact.
- Oxytocin Augmentation: For hypotonic uterine contractions (inadequate power).
- Requires continuous fetal monitoring.
- Titrate to achieve adequate contractions (>200 MVUs).
- Operative Delivery:
- Cesarean Section: For arrest disorders with adequate contractions or cephalopelvic disproportion (CPD).
- Forceps/Vacuum: Option for second-stage arrest if criteria met.
⭐ If labor arrests with adequate contractions (>200 MVUs), oxytocin augmentation is inappropriate; proceed to cesarean delivery.
High‑Yield Points - ⚡ Biggest Takeaways
- Abnormal labor includes protraction (slow progress) and arrest (no progress).
- Etiology involves the 3 Ps: Power (inadequate contractions), Passenger (fetal malposition), or Passage (pelvic issues).
- Inadequate power (<200 MVUs) is the most common cause; initial management is oxytocin.
- Arrest of labor despite adequate contractions (>4 hrs with >200 MVUs) requires Cesarean delivery.
- Second-stage arrest is defined by prolonged pushing (e.g., >3 hrs in a primipara with epidural).
- Key risks include chorioamnionitis, postpartum hemorrhage, and fetal distress.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

