Trypanosomes - The Basics
- Organism: Single-celled, flagellated protozoan parasites.
- Transmission: Vector-borne zoonoses.
- Key Species & Vectors:
- Trypanosoma brucei (African Sleeping Sickness): Tsetse fly.
- Trypanosoma cruzi (Chagas Disease): Reduviid bug (📌 "Kissing bug" - bites around the mouth).
- Morphology:
- Trypomastigote: Motile, C-shaped form with a flagellum found in blood smears.
- Amastigote: Non-motile, intracellular form (especially in T. cruzi).
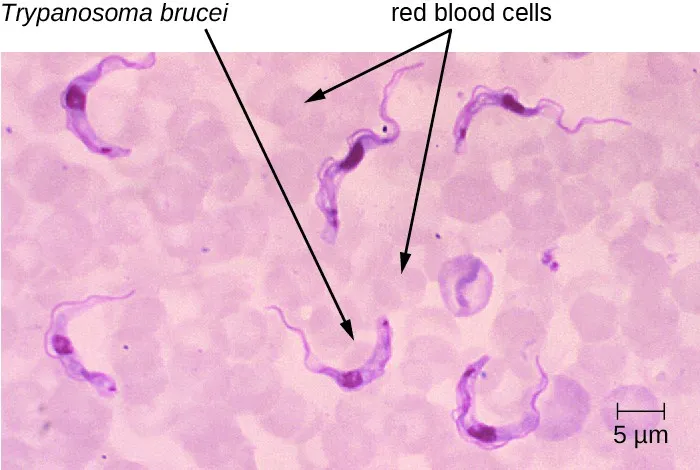
⭐ T. brucei exhibits remarkable antigenic variation by changing its variable surface glycoproteins (VSGs), leading to recurrent waves of fever and parasitemia.
T. cruzi - Chagas' Kiss
-
Vector: Triatomine bug ("Kissing Bug"), a reduviid bug.
-
Transmission: Bites, then defecates; scratching inoculates feces with trypomastigotes.
-
Pathogenesis: Intracellular amastigotes replicate in host cells, especially cardiac and GI muscle.
-
Acute Phase (weeks):
- Often asymptomatic; may have fever, malaise.
- Chagoma: Local inflammatory nodule at bite site.
- Romana's sign: Unilateral periorbital swelling (classic finding).
-
Chronic Phase (decades later):
- Cardiomyopathy: Apical aneurysm, mural thrombus, arrhythmia, heart failure.
- Mega-syndromes: Megaesophagus (dysphagia), megacolon (constipation).
⭐ A key finding in Chagasic cardiomyopathy is an apical aneurysm of the left ventricle.
T. brucei - Sleeping Sickness
- Vector: Tsetse fly (Glossina species).
- Subspecies & Region:
- T. b. gambiense: West/Central Africa (chronic course).
- T. b. rhodesiense: East Africa (acute, more virulent course).
- Clinical Progression:
- Early (Hemolymphatic): Painful chancre at bite site, intermittent fever, generalized lymphadenopathy.
- Winterbottom's sign: Posterior cervical lymphadenopathy is characteristic.
- Late (Meningoencephalitic): Invasion of the CNS leads to headaches, personality changes, daytime somnolence, nighttime insomnia, and eventually coma/death.
- Early (Hemolymphatic): Painful chancre at bite site, intermittent fever, generalized lymphadenopathy.
⭐ Antigenic Variation: Trypanosoma brucei evades the host immune system by periodically switching its dense coat of Variable Surface Glycoproteins (VSGs), leading to waves of parasitemia and fever.
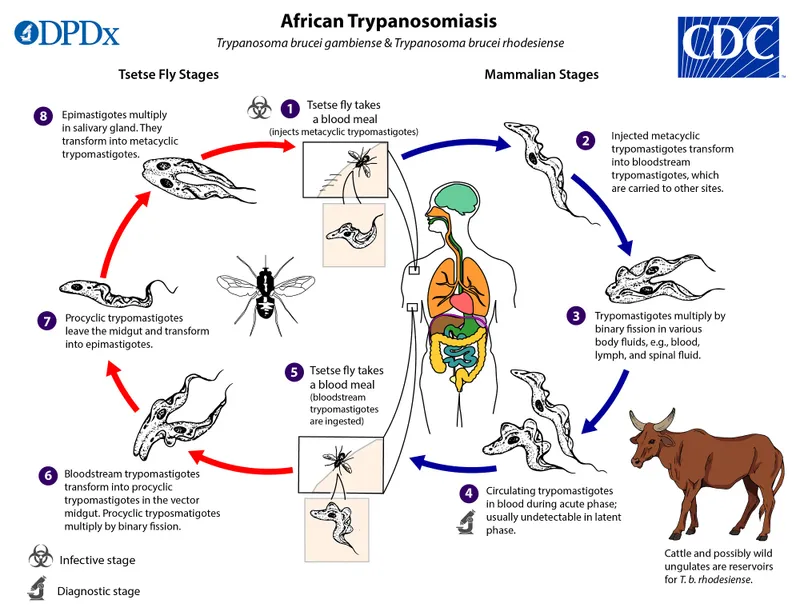
- Diagnosis: Motile trypomastigotes on blood smear, lymph node aspirate, or in CSF.
- Treatment: Varies by subspecies and disease stage (e.g., Pentamidine/Suramin for hemolymphatic; Melarsoprol for late-stage CNS).
Diagnosis & Rx - Find & Fight
-
Diagnosis:
- African (T. brucei): Find motile trypomastigotes on blood smear, lymph node aspirate, or in CSF for staging.
- American (T. cruzi): Giemsa-stained blood smear for acute phase; serology (ELISA, IFA) is crucial for diagnosing chronic disease.
-
Treatment:
- T. brucei: Suramin (rhodesiense) or Pentamidine (gambiense) for blood-stage. Melarsoprol or Eflornithine for CNS-stage.
- T. cruzi: Benznidazole or Nifurtimox for acute infection; chronic phase management is largely symptomatic.
⭐ Melarsoprol, an arsenic derivative for late-stage African trypanosomiasis, can cause a fatal reactive encephalopathy in 5-10% of patients.
High‑Yield Points - ⚡ Biggest Takeaways
- Trypanosoma cruzi causes Chagas disease, transmitted by reduviid bugs, leading to cardiomyopathy and mega-syndromes.
- Trypanosoma brucei causes African Sleeping Sickness, transmitted by tsetse flies, marked by a chancre and Winterbottom's sign.
- Diagnosis for both involves identifying trypomastigotes on a blood smear.
- Romana's sign (unilateral periorbital swelling) is a classic acute sign of Chagas disease.
- Treat Chagas with benznidazole or nifurtimox.
- Treat African sleeping sickness with suramin (blood-stage) or melarsoprol (CNS penetration).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

