Trematodes - General Fluke Facts
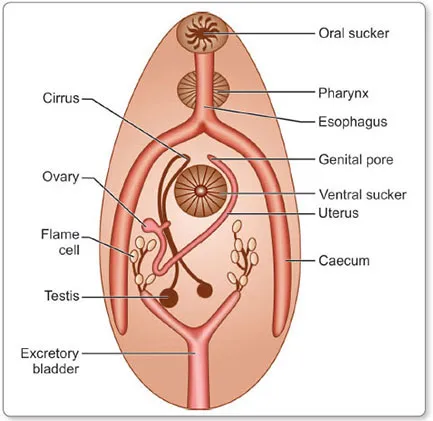
- Leaf-shaped, bilaterally symmetric flatworms.
- Most are hermaphroditic (monoecious).
- Possess two suckers: oral (feeding) and ventral (attachment).
- Life cycle requires snails as the first intermediate host.
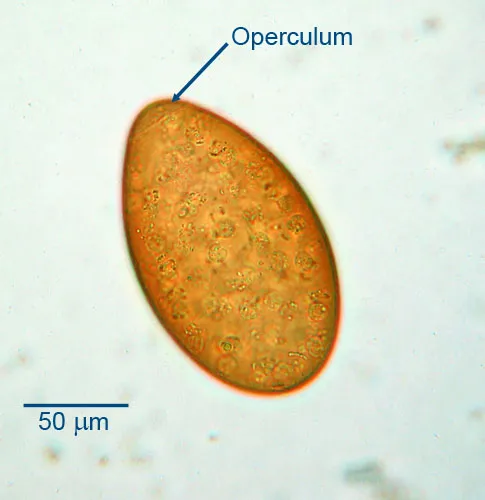
- Eggs are typically operculated (lidded), aiding in identification.
- Transmission involves ingestion of metacercariae or skin penetration by cercariae.
⭐ High-Yield Exception: Schistosoma species are not hermaphroditic (dioecious) and lay non-operculated eggs.
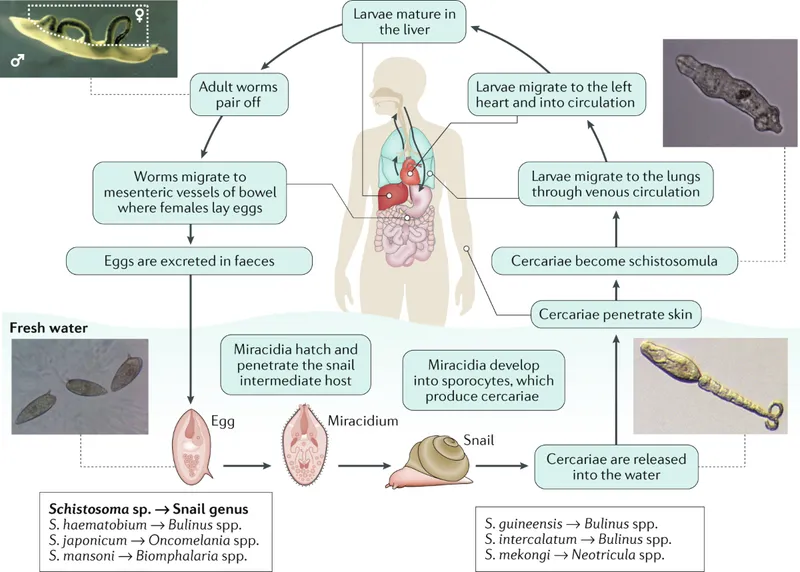
Schistosoma - Blood Fluke Blues
- Transmission: Free-swimming cercariae in freshwater (from snail hosts) penetrate human skin.
- Pathogenesis: It's the eggs, not the adult worms, that trigger a Th2-mediated granulomatous response, leading to fibrosis and organ damage.
- Clinical Syndromes:
- Intestinal: S. mansoni, S. japonicum → portal hypertension, hepatosplenomegaly, varices.
- Urogenital: S. haematobium → hematuria, dysuria, hydronephrosis.
- Acute: Katayama fever (systemic hypersensitivity reaction).
- Diagnosis: Eggs in stool (mansoni/japonicum) or urine (haematobium).
- Treatment: Praziquantel.
⭐ Exam Favorite: Schistosoma haematobium is strongly associated with Squamous Cell Carcinoma of the bladder.
Clonorchis & Fasciola - Liver Invaders
-
Clonorchis sinensis (Chinese Liver Fluke)
- Transmission: Undercooked freshwater fish.
- Pathology: Lives in biliary ducts, causing inflammation, fibrosis, and pigmented gallstones.
- Major risk for cholangiocarcinoma.
- Diagnosis: Operculated eggs in stool.
- Treatment: Praziquantel.
-
Fasciola hepatica (Sheep Liver Fluke)
- Transmission: Ingesting aquatic plants like watercress.
- Pathology: Migrates through liver parenchyma, causing RUQ pain, fever, and hepatomegaly.
- Diagnosis: Large, operculated eggs in stool.
- Treatment: Triclabendazole (Praziquantel-resistant).
⭐ Marked eosinophilia during the acute migratory phase is characteristic of Fasciola infection.
Paragonimus - Lung Fluke Woes
- Organism: Paragonimus westermani (Lung Fluke).
- Transmission: Ingesting undercooked freshwater crabs or crayfish containing metacercariae.
- Clinical: Chronic cough with bloody sputum (hemoptysis), mimicking tuberculosis; pleuritic chest pain.
- Diagnosis: Oval, operculated eggs in sputum or feces; eosinophilia; chest X-ray shows infiltrates/cavities.
- Treatment: Praziquantel.
⭐ Ectopic migration to the brain can cause seizures and neurological deficits, a key differential for cysticercosis in endemic areas.
Fluke Dx & Rx - The Praziquantel Plan
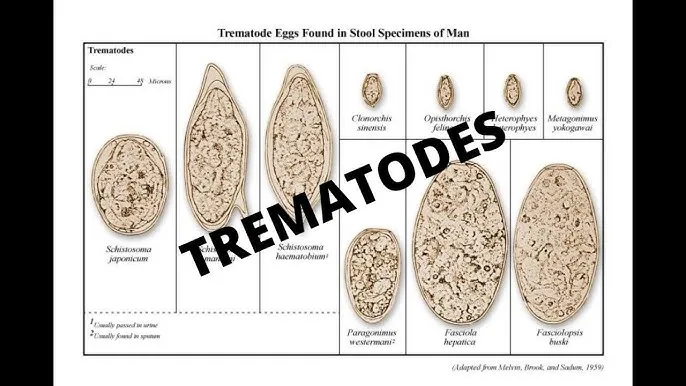
- Diagnosis (Dx): Stool/urine microscopy for eggs (O&P).
- S. haematobium: Urine (look for terminal spine).
- S. mansoni: Stool (look for lateral spine).
- S. japonicum: Stool (look for small, round egg).
- Paragonimus westermani: Sputum O&P.
- Treatment (Rx): Praziquantel is the drug of choice for most flukes.
⭐ Praziquantel works by increasing calcium permeability in the fluke, causing paralysis, contraction, and detachment from the host vessel wall.
High‑Yield Points - ⚡ Biggest Takeaways
- Schistosoma are blood flukes with separate sexes, unlike other trematodes; transmission involves snails and skin penetration.
- Paragonimus westermani (lung fluke), from undercooked crab, causes hemoptysis, mimicking TB.
- Clonorchis sinensis (liver fluke), from undercooked fish, is a major risk factor for cholangiocarcinoma.
- Fasciola hepatica (sheep liver fluke) is acquired from contaminated watercress.
- Diagnosis relies on identifying characteristic eggs in stool, urine, or sputum.
- Praziquantel is the drug of choice for nearly all fluke infections.
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

