Toxo Overview - The Cunning Cat Parasite
- Obligate intracellular, zoonotic protozoan with a worldwide distribution.
- Definitive host: Felines (cats) are the sole host for sexual reproduction.
- Transmission forms & routes:
- Oocysts: Ingested from soil or water contaminated with cat feces.
- Bradyzoites: Tissue cysts consumed in undercooked/raw meat (esp. pork, lamb).
- Tachyzoites: Active, replicating form; responsible for vertical (transplacental) transmission.
⭐ In immunocompromised patients (e.g., HIV with CD4 < 100), reactivation is common, classically causing multiple ring-enhancing brain lesions.
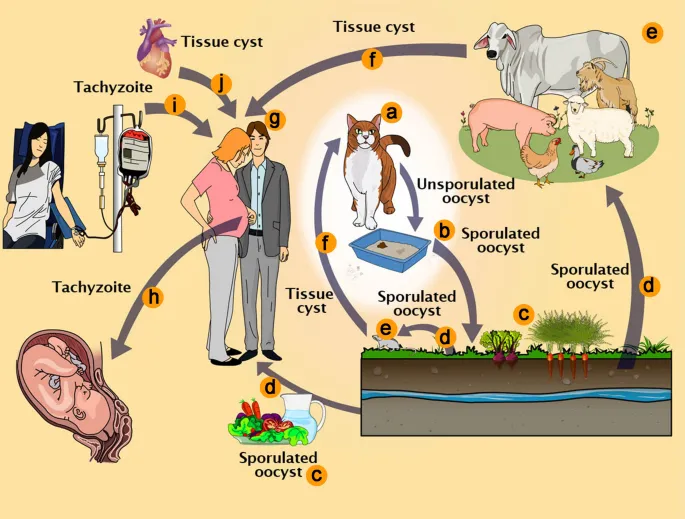
Transmission & Lifecycle - From Cat to Human

- Definitive Host: Cat. Oocysts are shed in feces.
- Intermediate Hosts: Humans, livestock, rodents.
- Human Infection Routes:
- Ingesting oocysts from contaminated water, soil, or cat litter.
- Ingesting tissue cysts (bradyzoites) in undercooked meat.
- Transplacental (congenital) transmission.
⭐ Risk of congenital transmission ↑ with gestational age (highest in 3rd trimester), but disease severity is greatest if infection occurs in the 1st trimester.
Clinical Syndromes - Brain, Eyes, & Baby
-
Immunocompromised (AIDS, CD4 < 100)
- Toxoplasmic Encephalitis (TE): Headache, confusion, fever, focal deficits, seizures.
- Imaging: Multiple ring-enhancing lesions on CT/MRI.

-
Immunocompetent & Congenital
- Chorioretinitis: Most common manifestation.
- Eye pain, floaters, vision loss. Fundoscopy shows "headlights in the fog."
- Often a reactivation of a congenital infection.
-
Congenital (Transplacental)
- Classic Triad: Chorioretinitis, hydrocephalus, and intracranial calcifications.
- Risk of transmission ↑ with gestational age, but severity ↓.
⭐ In AIDS patients, Toxoplasmic Encephalitis is the most common cause of a CNS mass lesion.
Diagnosis - Spotting the Intruder
- Serology: Primary method. Detects anti-Toxoplasma IgG & IgM antibodies. IgM indicates recent infection.
- Imaging (Immunocompromised): CT or MRI of the brain reveals multiple, ring-enhancing lesions, often with a predilection for the basal ganglia.
- Definitive Diagnosis: Brain biopsy showing tachyzoites is the gold standard but reserved for unclear cases.
- Congenital: PCR analysis of amniotic fluid.

⭐ In HIV patients, the presence of ring-enhancing lesions on brain imaging is most commonly caused by toxoplasmosis, especially with a CD4 count < 100 cells/μL.
Treatment & Prevention - The Toxo Takedown
- Primary Regimen (Immunocompromised & Severe Disease):
- Pyrimethamine + Sulfadiazine
- Plus Leucovorin (folinic acid) to prevent hematologic toxicity.
- Alternative: TMP-SMX (especially for prophylaxis), or regimens with Clindamycin/Atovaquone.
- Prophylaxis (e.g., HIV):
- Initiate when CD4 count < 100 cells/μL.
- TMP-SMX is the preferred agent.
- General Prevention:
- Thoroughly cook meat to kill cysts.
- Pregnant women should avoid contact with cat feces (litter boxes).
⭐ Leucovorin rescue is essential; it bypasses the dihydrofolate reductase (DHFR) block in human cells, preventing myelosuppression, but not in the parasite.
High‑Yield Points - ⚡ Biggest Takeaways
- Key transmission routes: cat feces (oocysts), undercooked meat (cysts), or transplacental (tachyzoites).
- Classic triad of congenital toxoplasmosis: chorioretinitis, hydrocephalus, and intracranial calcifications.
- In immunocompromised patients (AIDS < 100 CD4), presents with multiple ring-enhancing brain lesions.
- Diagnosis is confirmed with serology or PCR.
- Prophylaxis and treatment rely on pyrimethamine and sulfadiazine (plus leucovorin).
Unlock the full lesson and continue reading
Signup to continue reading this lesson and unlimited access questions, flashcards, AI notes, and more

